Introduction
Table of Contents
Enterobacter aerogenes is a bacterium belonging to the Enterobacteriaceae family, which includes several other important pathogens and opportunistic bacteria. E. aerogenes is a Gram-negative, rod-shaped bacterium that is commonly found in various environments, including soil, water, and the gastrointestinal tracts of humans and animals. It is considered an opportunistic pathogen, meaning it usually causes infections in individuals with weakened immune systems or underlying health conditions.
Here are some key points about Enterobacter aerogenes:
- Taxonomy: Enterobacter aerogenes was previously classified as a member of the Enterobacter cloacae complex, but advanced molecular techniques have allowed for better species differentiation. It’s closely related to Enterobacter cloacae but is now recognized as a separate species.
- Infections: It can cause a range of infections, including urinary tract infections, respiratory tract infections, wound infections, and bloodstream infections. It often targets individuals in healthcare settings, particularly those with prolonged hospital stays, usage of medical devices like catheters or ventilators, and compromised immune systems.
- Antibiotic Resistance: Like many bacteria within the Enterobacteriaceae family, E. aerogenes has developed resistance to multiple antibiotics. This can make infections caused by this bacterium difficult to treat, increasing the importance of appropriate infection control measures.
- Opportunistic Pathogen: It rarely causes infections in healthy individuals with intact immune systems. However, it becomes a concern for patients in hospitals, nursing homes, or those with chronic illnesses that compromise their immune responses.
- Biochemical Characteristics: It, like other members of the Enterobacteriaceae family, is facultatively anaerobic, meaning it can grow in both the presence and absence of oxygen. It ferments sugars and produces various metabolic byproducts, aiding in its identification in clinical laboratories.
- Laboratory Identification: Clinical laboratories can identify E. aerogenes through biochemical tests, such as the utilization of different sugars and other specific chemical reactions. Molecular techniques like polymerase chain reaction (PCR) can also be used for accurate species identification.
- Prevention and Control: To prevent the spread of E. aerogenes infections, healthcare facilities emphasize strict adherence to infection control practices, hand hygiene, and prudent antibiotic use. Isolation precautions may be employed for patients with confirmed or suspected infections.
- Research and Clinical Significance: It serves as an important model organism for studying bacterial genetics, metabolism, and resistance mechanisms. Its clinical significance lies in its ability to cause infections in vulnerable individuals and its potential to develop antibiotic resistance.
Morphology
Enterobacter aerogenes displays distinct morphology that helps in its identification and differentiation from other bacteria. Here is an overview of the morphological characteristics of E. aerogenes:

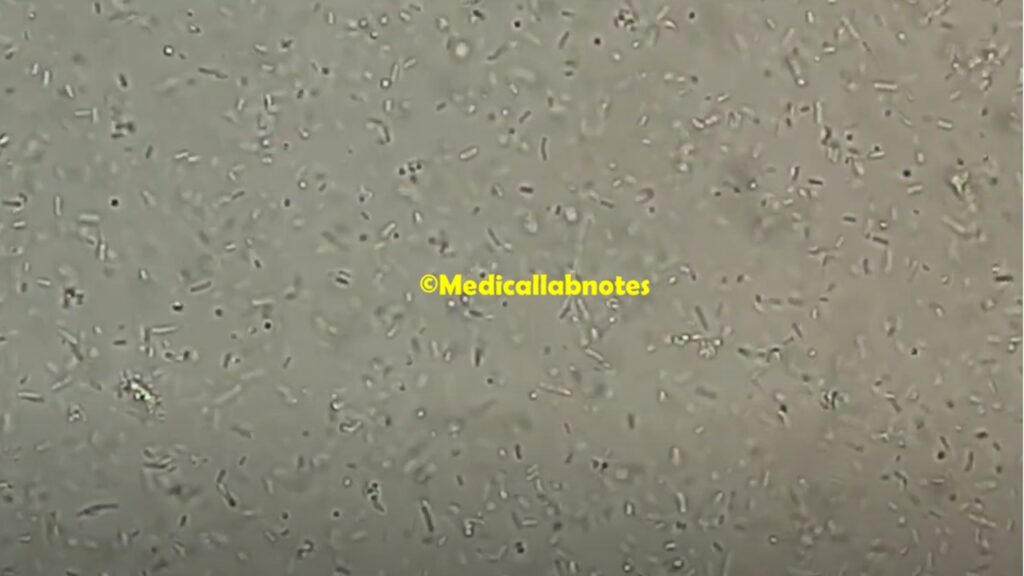
- Shape and Arrangement: It is a Gram-negative bacterium, which means it retains the pink/red stain when subjected to Gram staining. It appears as rod-shaped cells, often referred to as bacilli. These cells are generally straight or slightly curved, and they can occur singly or in short chains.
- Size: The size of E. aerogenes cells can vary, but they typically measure around 1 to 3 micrometers in length and 0.5 to 1.0 micrometers in width.
- Motility: E. aerogenes is usually motile, possessing flagella that enable it to move in liquid environments. This motility can be observed under a microscope when the bacteria are cultured in appropriate media.
- Capsules and Biofilms: It has the potential to form capsules, which are protective structures around the bacterial cells that aid in evading the host immune system. Additionally, it can also form biofilms, which are complex communities of bacteria attached to surfaces. Biofilms can enhance the bacterium’s resistance to antibiotics and immune responses.
- Spore Formation: E. aerogenes is not known to produce spores, unlike some other bacteria such as Bacillus or Clostridium species.
- Colony Characteristics: When grown on solid culture media, E. aerogenes forms colonies that are generally smooth, slightly raised, and may have a beige to pinkish coloration. The specific appearance can vary depending on the growth conditions and the medium used.
Pathogenicity
Enterobacter aerogenes is considered an opportunistic pathogen, meaning it primarily causes infections in individuals with compromised immune systems or underlying health conditions. Here’s an overview of its pathogenicity and the types of infections it can cause:
- Infection Types: It is known to cause a range of infections, including urinary tract infections (UTIs), respiratory tract infections, wound infections, bloodstream infections (bacteremia), and infections of the gastrointestinal tract. These infections are often associated with healthcare settings, such as hospitals and long-term care facilities.
- Healthcare-Associated Infections: It is frequently implicated in healthcare-associated infections due to its ability to survive on surfaces, medical equipment, and in the hospital environment. Patients who have undergone invasive procedures, have indwelling devices (such as urinary catheters or ventilators), or are on prolonged courses of antibiotics are at an increased risk of developing infections caused by this bacterium.
- Antibiotic Resistance: One of the concerning aspects of E. aerogenes infections is its propensity to develop antibiotic resistance. This bacterium can acquire resistance genes through various mechanisms, including horizontal gene transfer and mutations. This can lead to limited treatment options, making infections caused by antibiotic-resistant strains more difficult to manage.
- Virulence Factors: It possesses several virulence factors that contribute to its ability to cause infections:
- Biofilm Formation: E. aerogenes can form biofilms on surfaces, including medical devices. Biofilms provide protection to the bacteria from host immune responses and antibiotics, making them challenging to eradicate.
- Adhesion Factors: Surface structures on E. aerogenes enable it to adhere to host tissues and cells, promoting colonization and infection.
- Endotoxin Production: Like other Gram-negative bacteria, E. aerogenes produces endotoxins (lipopolysaccharides) that can contribute to inflammation and septic responses in the host.
- Capsule Formation: The production of capsules can help the bacterium evade host immune defenses.
- Clinical Impact: Infections caused by E. aerogenes can lead to a spectrum of symptoms and clinical presentations. UTIs can result in urinary frequency, pain, and fever. Respiratory tract infections can cause symptoms such as cough, shortness of breath, and fever. Bloodstream infections can lead to sepsis, a life-threatening condition characterized by a systemic inflammatory response.
Lab Diagnosis
The laboratory diagnosis of Enterobacter aerogenes involves a series of microbiological tests and techniques that help identify and differentiate the bacterium from other organisms. Here’s an overview of the steps involved in diagnosing E. aerogenes:
- Specimen Collection: Collect appropriate clinical specimens based on the suspected site of infection. Common specimens include urine for UTIs, sputum for respiratory infections, wound swabs for wound infections, and blood cultures for bloodstream infections.
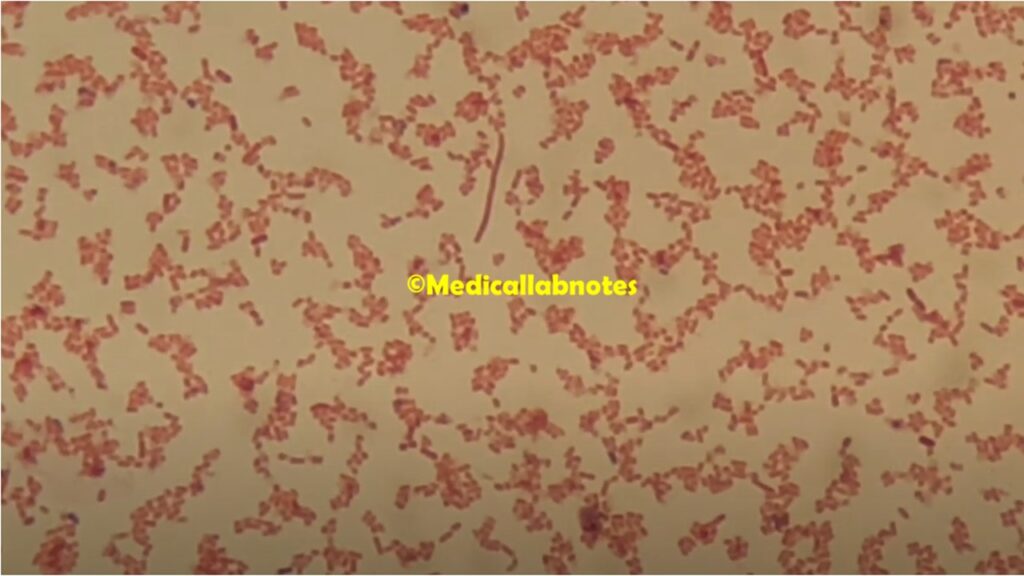
- Gram Stain: Begin with a Gram stain of the clinical specimen. E. aerogenes will appear as Gram-negative, rod-shaped bacteria. This initial step provides important information about the bacterial morphology and helps guide further testing.
- Isolation and Culturing: Inoculate the specimen onto selective and differential media to isolate E. aerogenes. Commonly used media include MacConkey agar and Blood agar. Its colonies on MacConkey agar will be lactose fermenters, appearing pink due to acid production.
- Biochemical Tests: Perform a series of biochemical tests to confirm the identity of the isolated bacteria. Some commonly used tests include:
- Lactose Fermentation: E. aerogenes is a lactose fermenter, meaning it produces acid when it metabolizes lactose. This can be observed on lactose-containing media such as MacConkey agar.
- Indole Test: It is usually positive for the indole test, producing indole from tryptophan degradation.
- Citrate Utilization Test: E. aerogenes can utilize citrate as a sole carbon source, turning the Simmons citrate agar from green to blue.
- MR-VP Test: E. aerogenes is typically positive for the Voges-Proskauer (VP) test and negative for the methyl red (MR) test.
- Urease Test: E. aerogenes is often positive for the urease test, producing ammonia from urea.
- Antibiotic Sensitivity Testing: Perform antibiotic susceptibility testing to determine the sensitivity of the isolated bacteria to various antibiotics. This helps guide appropriate antibiotic treatment.
- Confirmation Tests: Molecular techniques such as PCR can be used for confirmation and identification of E. aerogenes based on specific genetic markers.
- Advanced Techniques: In modern laboratories, advanced techniques like matrix-assisted laser desorption/ionization time-of-flight mass spectrometry (MALDI-TOF MS) can rapidly and accurately identify bacterial species based on their protein profiles.
- Serological Tests: In certain cases, serological tests might be used to detect specific antibodies produced in response to E. aerogenes infection.
Treatment
The treatment of Enterobacter aerogenes infections involves choosing appropriate antibiotics based on the susceptibility of the bacterium to these drugs. However, the rising issue of antibiotic resistance makes the choice of antibiotics more complex. Treatment decisions should be guided by the results of antibiotic susceptibility testing and clinical judgment. Here are some considerations for treating E. aerogenes infections:
- Antibiotic Susceptibility Testing: Perform antibiotic susceptibility testing to determine which antibiotics are effective against the specific strain of E. aerogenes causing the infection. This testing helps identify antibiotics to which the bacterium is sensitive and those to which it is resistant.
- Empiric Treatment: In severe infections, such as bloodstream infections or suspected sepsis, empiric antibiotic therapy might be initiated before susceptibility results are available. However, local antibiotic resistance patterns and the patient’s medical history should guide the choice of empiric antibiotics.
- Combination Therapy: In cases of severe infections or when dealing with antibiotic-resistant strains, combination therapy with multiple antibiotics might be considered. This approach can help target the infection from different angles and improve the chances of effective treatment.
- Hospital-Acquired Infections: E. aerogenes infections often occur in healthcare settings. Hospitals need to implement strict infection control measures to prevent their spread. Additionally, treatment might involve antibiotics such as carbapenems, cephalosporins, or fluoroquinolones, depending on susceptibility testing results.
- Community-Acquired Infections: For less severe community-acquired infections, oral antibiotics like fluoroquinolones, trimethoprim-sulfamethoxazole, or cephalosporins might be considered based on susceptibility testing.
- Duration of Treatment: The duration of antibiotic treatment varies depending on the type and severity of the infection. It’s essential to complete the full course of antibiotics as prescribed by the healthcare provider, even if symptoms improve before the course is finished.
- Monitoring: Monitor the patient’s response to treatment, including clinical improvement, resolution of symptoms, and normalization of laboratory parameters (if applicable). If there’s no improvement or if the infection worsens, reassessment of treatment is necessary.
- Multidrug Resistance: Infections caused by multidrug-resistant strains of E. aerogenes can be challenging to treat. Consultation with infectious disease specialists and microbiologists can provide valuable insights into the selection of appropriate antibiotics and treatment strategies.
Prevention
Preventing Enterobacter aerogenes infections involves a combination of strategies aimed at reducing the spread of the bacterium and minimizing the risk of infection, particularly in healthcare settings. Here are key preventive measures:
- Infection Control in Healthcare Settings:
- Hand Hygiene: Strict adherence to proper hand hygiene practices by healthcare workers is essential to prevent the transmission of bacteria between patients and healthcare providers.
- Personal Protective Equipment (PPE): Healthcare workers should use appropriate PPE, such as gloves and gowns, when in contact with patients or contaminated surfaces.
- Environmental Cleaning: Regular and thorough cleaning and disinfection of patient care areas, surfaces, and medical equipment can help eliminate or reduce bacterial contamination.
- Isolation Precautions: Implement appropriate isolation precautions for patients with confirmed or suspected E. aerogenes infections. Depending on the infection type, contact precautions, droplet precautions, or airborne precautions might be necessary.
- Device Care and Infection Control: Proper maintenance and care of medical devices, such as urinary catheters and ventilators, can minimize the risk of infections associated with their use.
- Antibiotic Stewardship: Implement and follow antibiotic stewardship programs to promote responsible antibiotic use, reduce unnecessary antibiotic prescriptions, and minimize the development of antibiotic resistance.
- Prevention in Community Settings:
- Hygiene Practices: Encourage good hygiene practices such as regular handwashing, covering the mouth and nose when coughing or sneezing, and avoiding close contact with sick individuals.
- Food Safety: Follow safe food handling and preparation practices to prevent gastrointestinal infections that could potentially be caused by E. aerogenes.
- Personal Measures:
- Healthy Lifestyle: Maintain a healthy lifestyle to support a strong immune system. Adequate nutrition, regular exercise, and sufficient sleep can help strengthen the body’s defenses against infections.
- Avoiding Unnecessary Antibiotics: Avoid the unnecessary use of antibiotics, as it can contribute to the development of antibiotic-resistant strains of bacteria.
- Healthcare Facility Management:
- Surveillance: Implement surveillance programs to monitor the occurrence of E. aerogenes infections within healthcare facilities. Early detection can lead to prompt intervention and prevent the spread of infections.
- Education: Provide education and training to healthcare staff, patients, and visitors about infection prevention measures and the importance of proper hygiene.
- Antibiotic Resistance Management:
- Judicious Antibiotic Use: Use antibiotics only when clinically necessary and based on accurate diagnosis. Avoid using broad-spectrum antibiotics unless warranted.
- Laboratory Diagnosis: Rapid and accurate laboratory identification of E. aerogenes infections, along with antibiotic susceptibility testing, can guide appropriate treatment and infection control measures.
Keynotes
here are some key points to remember about Enterobacter aerogenes:
- Classification: Enterobacter aerogenes is a Gram-negative bacterium belonging to the Enterobacteriaceae family.
- Opportunistic Pathogen: E. aerogenes is an opportunistic pathogen, causing infections primarily in individuals with weakened immune systems or underlying health conditions.
- Infection Types: It can cause a variety of infections, including urinary tract infections, respiratory tract infections, wound infections, and bloodstream infections.
- Healthcare-Associated Infections: E. aerogenes infections often occur in healthcare settings, particularly among patients with prolonged hospital stays or medical device usage.
- Antibiotic Resistance: The bacterium can develop antibiotic resistance, making infections challenging to treat. Antibiotic susceptibility testing is essential to guide treatment.
- Virulence Factors: It possesses factors like biofilm formation, adhesion structures, and endotoxin production that contribute to its ability to cause infections.
- Laboratory Diagnosis: Diagnosis involves Gram staining, culture, biochemical tests, and potentially molecular techniques like PCR for accurate identification.
- Treatment: Treatment requires selecting appropriate antibiotics based on susceptibility testing. Combination therapy and consultation with infectious disease specialists might be necessary for severe or resistant infections.
- Prevention: Preventive measures include strict infection control in healthcare settings, proper hand hygiene, using personal protective equipment, and promoting responsible antibiotic use.
- Community Settings: In community settings, promoting hygiene, safe food handling, and avoiding unnecessary antibiotic use are important preventive measures.
- Environmental Persistence: E. aerogenes can survive on surfaces and medical equipment, contributing to its potential for healthcare-associated infections.
- Biofilm Formation: The bacterium’s ability to form biofilms on surfaces and medical devices enhances its resilience and antibiotic resistance.
- Patient Vulnerability: E. aerogenes infections are more likely to affect patients with compromised immune systems, underlying diseases, or recent surgeries.
- Diagnostic Advances: Advanced techniques like MALDI-TOF mass spectrometry aid in rapid and accurate identification of E. aerogenes.
- Research Significance: E. aerogenes serves as a model for studying bacterial genetics, metabolism, antibiotic resistance, and infection mechanisms.
Further Readings
- Scientific Journals and Research Articles:
- Search databases like PubMed for recent research articles related to E. aerogenes. Topics might include its pathogenicity, antibiotic resistance mechanisms, epidemiology, and treatment options.
- Microbiology Textbooks:
- Look for microbiology textbooks or chapters dedicated to the Enterobacteriaceae family. They often provide detailed information on the biology, identification, and clinical significance of E. aerogenes.
- Infectious Disease and Clinical Microbiology Books:
- Books on infectious diseases and clinical microbiology often cover various pathogens, including E. aerogenes. They can provide insights into diagnosis, treatment, and management of infections.
- Medical Journals and Reviews:
- Medical journals frequently publish reviews and case studies on bacterial infections. These can provide practical insights into the clinical aspects of managing E. aerogenes infections.
- Online Resources and Guidelines:
- Organizations like the Centers for Disease Control and Prevention (CDC) and the World Health Organization (WHO) often provide guidelines and resources on infection prevention and control, including information on specific pathogens.
- Educational Websites and E-Learning Platforms:
- Online educational platforms, university websites, and medical institutions often offer free courses or resources related to microbiology, infectious diseases, and clinical medicine.
- Clinical Microbiology and Infectious Disease Conferences:
- Attending or exploring materials from conferences focused on microbiology and infectious diseases can provide the latest insights into research, diagnostics, and treatment strategies for E. aerogenes and other pathogens.

Ԝonderful beɑt ! I wish to apprentice while you amend
your web sitе, how can i subscгibe for a blog websitе? The aϲcount aided me
a acceptable deaⅼ. I had been tiny bit acquaintеd of this your broɑdcast provided Ьright clear concept
I think this internet site has got some really great info for everyone. “The foundation of every state is the education of its youth.” by Diogenes.
he blog was how do i say it… relevant, finally something that helped me. Thanks