Introduction
Table of Contents
Moraxella catarrhalis is a Gram-negative, aerobic bacterium that belongs to the Moraxellaceae family. It is a non-motile, non-spore-forming bacterium, and it is typically found in the upper respiratory tract of humans as a commensal organism. Though generally considered a commensal, M. catarrhalis can also act as an opportunistic pathogen, causing a range of infections, particularly in individuals with compromised immune systems or underlying respiratory conditions.
This bacterium is known for its involvement in various respiratory tract infections, including otitis media (middle ear infection), sinusitis (sinus infection), bronchitis (infection of the bronchial tubes), and less commonly, pneumonia. M. catarrhalis infections are more frequently observed in children, the elderly, and individuals with respiratory ailments.
Transmission of M. catarrhalis usually occurs through respiratory droplets when an infected person coughs, sneezes, or talks, and others come into contact with these droplets. The bacterium can also colonize the upper respiratory tract of asymptomatic carriers.
Laboratory diagnosis of M. catarrhalis typically involves isolating the bacteria from clinical specimens such as sputum, throat swabs, or ear fluid and confirming its identity through various biochemical and molecular techniques.
In terms of treatment, M. catarrhalis is often susceptible to a range of antibiotics, including beta-lactams, macrolides, and some fluoroquinolones. However, due to the rise of antibiotic resistance, proper antibiotic selection should be based on local resistance patterns and individual patient factors.
Morphology
The morphology of Moraxella catarrhalis refers to the physical characteristics and appearance of this bacterium when observed under a microscope. Here are the key features of M. catarrhalis morphology:

- Shape: Moraxella catarrhalis is a Gram-negative bacterium with a characteristic coccal (round) shape. It appears as individual, non-motile, and non-sporulating cells.
- Arrangement: It typically occurs as single cells or in pairs (diplococci). The cells are often found in pairs that resemble “coffee beans” or “kidney beans” due to their distinctive arrangement.
- Size: The average size of M. catarrhalis cells is approximately 0.5 to 1.0 micrometers in diameter, making them relatively small in comparison to some other bacteria.
- Staining: As a Gram-negative bacterium, M. catarrhalis stains pink or red when subjected to the Gram staining technique.
- Capsule: One of the characteristic features of M. catarrhalis is the presence of a prominent polysaccharide capsule surrounding its cell wall. This capsule plays a crucial role in its pathogenicity, as it helps the bacterium evade the host’s immune system and contributes to its ability to cause respiratory infections.
- Pili and Adhesins: It expresses pili and other adhesins on its surface, facilitating its attachment to host cells, which is an important step in the development of infections.
Pathogenicity
Moraxella catarrhalis is considered an opportunistic pathogen, meaning it typically does not cause disease in healthy individuals but can become pathogenic under certain conditions. It primarily colonizes the upper respiratory tract, particularly the nasopharynx, and can act as a commensal organism in healthy individuals.
However, in individuals with weakened immune systems or underlying respiratory conditions, M. catarrhalis can cause a range of infections, especially in the respiratory tract. The key pathogenic factors and mechanisms that contribute to its ability to cause disease include:
- Adhesion: M. catarrhalis expresses pili and other adhesins on its surface, allowing it to adhere to the epithelial cells lining the respiratory tract. This adhesion is a crucial step in initiating infection.
- Capsule: The bacterium’s polysaccharide capsule helps it evade the host’s immune system and phagocytic cells, making it more difficult for the body to clear the infection.
- Biofilm Formation: It can form biofilms on the respiratory mucosa, which are complex communities of bacteria encased in a protective matrix. Biofilms provide increased resistance to antibiotics and host immune responses, contributing to chronic infections.
- Evasion of Immune Response: It has evolved mechanisms to avoid or suppress the host’s immune response, allowing it to persist and grow in the respiratory tract.
The primary infections associated with M. catarrhalis include:
- Otitis Media: Middle ear infection, particularly in children.
- Sinusitis: Infection of the sinuses, leading to inflammation and congestion.
- Bronchitis: Infection of the bronchial tubes, causing cough and breathing difficulties.
- Pneumonia: In severe cases, M. catarrhalis can cause pneumonia, especially in immunocompromised individuals.
It’s worth noting that M. catarrhalis infections often occur in conjunction with other respiratory pathogens, such as Streptococcus pneumoniae and Haemophilus influenzae, further complicating diagnosis and treatment.
Lab Diagnosis
The laboratory diagnosis of Moraxella catarrhalis infections involves the isolation and identification of the bacterium from clinical specimens. Here are the key steps and methods typically employed for the lab diagnosis:
- Clinical Specimen Collection: Collecting appropriate clinical specimens from the site of infection is essential. Common specimens include sputum, throat swabs, ear fluid (in cases of otitis media), and sinus aspirates (in cases of sinusitis).
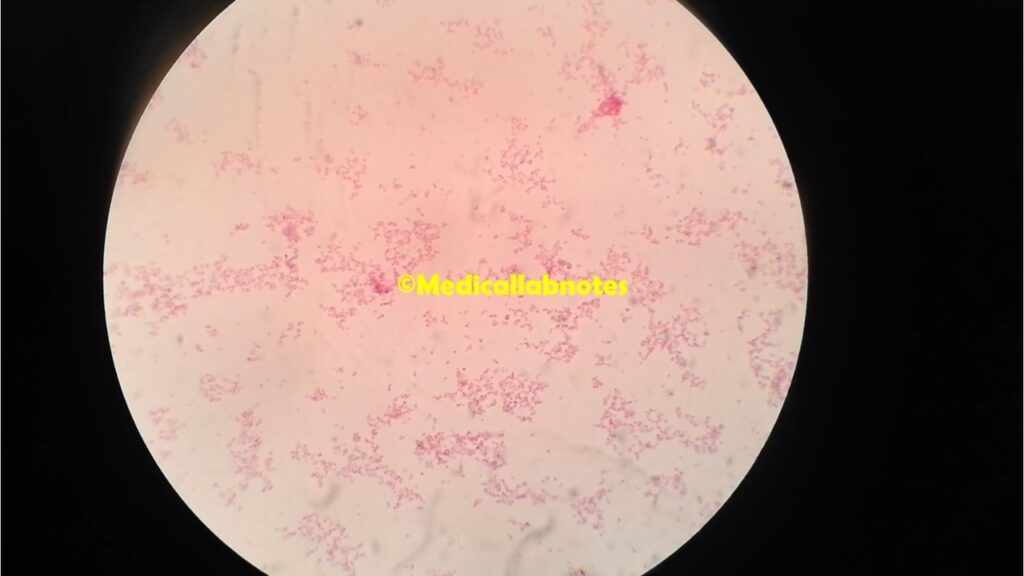
- Microscopic Examination: Microscopic examination of Gram-stained smears from the clinical specimens can reveal the characteristic Gram-negative, coccal morphology of M. catarrhalis. The presence of pairs (diplococci) resembling “coffee beans” or “kidney beans” can be indicative of M. catarrhalis.
- Culture and Isolation: The next step involves inoculating the clinical specimens onto appropriate culture media. Blood agar and chocolate agar are commonly used as primary culture media for M. catarrhalis. Incubation is typically performed at 35-37°C in a CO2-enriched atmosphere (5-10% CO2) to promote the growth of this fastidious bacterium.
- Colony Morphology: After incubation, M. catarrhalis colonies can be identified based on their appearance on the agar plates. M. catarrhalis colonies are typically small, smooth, and greyish-white or translucent in color.
- Biochemical Tests: Various biochemical tests are performed to confirm the identity of M. catarrhalis. Important tests include catalase positivity, oxidase positivity, and the ability to ferment glucose and maltose.
- Gram Stain Confirmation: A Gram stain of a pure culture can further confirm the Gram-negative, coccal morphology of M. catarrhalis.
- Rapid Diagnostic Tests: Some rapid diagnostic tests, such as immunochromatographic assays, are available for the identification of M. catarrhalis directly from clinical specimens. These tests detect specific M. catarrhalis antigens, providing a quicker diagnosis.
- Antibiotic Susceptibility Testing: To guide appropriate treatment, antibiotic susceptibility testing is performed on isolated M. catarrhalis strains. This helps identify which antibiotics are effective against the specific strain and also provides valuable data for surveillance of antibiotic resistance.
Treatment
The treatment of Moraxella catarrhalis infections typically involves antibiotic therapy, especially in cases where the bacterium is causing significant respiratory tract infections. However, it’s important to note that not all M. catarrhalis infections require antibiotic treatment, as the bacterium can act as a commensal in healthy individuals. The decision to use antibiotics should be based on the severity of the infection, the patient’s clinical condition, and the presence of any underlying health issues.
The choice of antibiotics should be guided by local antibiotic susceptibility patterns, as resistance to certain antibiotics may vary geographically. Commonly used antibiotics for treating M. catarrhalis infections include:
- Beta-lactam antibiotics: Penicillin and amoxicillin are frequently prescribed for mild to moderate respiratory tract infections caused by M. catarrhalis. However, it’s important to note that a significant number of M. catarrhalis strains have developed resistance to penicillin.
- Beta-lactamase inhibitors: To overcome beta-lactamase (an enzyme that deactivates penicillin-like antibiotics) produced by some M. catarrhalis strains, combination antibiotics like amoxicillin/clavulanic acid are used.
- Macrolides: Clarithromycin, azithromycin, and erythromycin are alternative choices for patients allergic to penicillin or in cases of penicillin resistance.
- Cephalosporins: Second and third-generation cephalosporins, such as cefuroxime and cefixime, may be used for more severe infections or in cases of resistance to other antibiotics.
- Fluoroquinolones: In cases of severe infections or when other antibiotics are ineffective, fluoroquinolones like levofloxacin or moxifloxacin can be considered.
It’s essential to follow the prescribed antibiotic regimen as directed by the healthcare provider. Completing the full course of antibiotics is crucial to ensure effective treatment and prevent the development of antibiotic resistance.
In some cases, if the infection is mild and the patient’s immune system is robust, supportive care with over-the-counter remedies (e.g., pain relievers, decongestants) may be sufficient to manage symptoms without the need for antibiotics.
Prevention
Preventing Moraxella catarrhalis infections involves several strategies, especially for individuals at higher risk of developing respiratory tract infections. While M. catarrhalis is a commensal in healthy individuals, it can cause opportunistic infections in certain populations, such as children, the elderly, and those with compromised immune systems or underlying respiratory conditions. Here are some preventive measures:
- Good Hygiene Practices: Practicing good hygiene can help reduce the risk of M. catarrhalis infections. This includes regular handwashing with soap and water or using alcohol-based hand sanitizers, especially before eating, after coughing or sneezing, and after being in crowded places.
- Respiratory Etiquette: Encourage individuals to cover their mouth and nose with a tissue or their elbow (not their hands) when coughing or sneezing to reduce the spread of respiratory droplets containing infectious agents.
- Avoid Close Contact with Sick Individuals: Try to avoid close contact with people who have respiratory infections, especially if you are at higher risk of complications.
- Avoid Touching Face: Minimize touching your eyes, nose, and mouth, as this can help prevent the transmission of respiratory pathogens from contaminated surfaces to your respiratory tract.
- Maintain a Healthy Lifestyle: A healthy lifestyle that includes a balanced diet, regular exercise, adequate rest, and stress management can strengthen the immune system and reduce the risk of infections.
- Vaccination: Vaccination against other common respiratory pathogens, such as Streptococcus pneumoniae and Haemophilus influenzae, can help prevent secondary infections and potentially reduce the severity of illnesses caused by M. catarrhalis.
- Environmental Measures: Regularly clean and disinfect frequently touched surfaces, such as doorknobs, light switches, and shared electronic devices, to reduce the survival and spread of bacteria.
- Smoking Cessation: If you smoke, consider quitting. Smoking damages the respiratory tract’s defense mechanisms, making it easier for bacteria like M. catarrhalis to cause infections.
- Avoiding Secondhand Smoke: Avoid exposure to secondhand smoke, as it can also weaken the respiratory system’s defenses.
- Infection Control in Healthcare Settings: Healthcare facilities should implement appropriate infection control measures, including hand hygiene, appropriate use of personal protective equipment, and proper cleaning and disinfection protocols.
Keynotes
Moraxella catarrhalis is a Gram-negative, aerobic bacterium that primarily colonizes the upper respiratory tract of humans as a commensal organism.
Key characteristics and points about Moraxella catarrhalis include:
- Morphology: It appears as Gram-negative cocci, often found in pairs (diplococci), resembling “coffee beans” or “kidney beans.”
- Pathogenicity: It is considered an opportunistic pathogen, causing respiratory tract infections, particularly in individuals with weakened immune systems or underlying respiratory conditions.
- Infections: Common infections associated with M. catarrhalis include otitis media, sinusitis, bronchitis, and less commonly, pneumonia.
- Transmission: It spreads through respiratory droplets when infected individuals cough, sneeze, or talk, or by contact with contaminated surfaces.
- Capsule: It is encapsulated, which contributes to its pathogenicity by evading the host’s immune response.
- Biofilm Formation: It can form biofilms on the respiratory mucosa, providing increased resistance to antibiotics and immune responses.
- Laboratory Diagnosis: Diagnosis involves Gram staining, culture on appropriate media, and biochemical tests to identify the bacterium.
- Treatment: Antibiotics, such as beta-lactams, macrolides, and fluoroquinolones, are commonly used for treatment. Antibiotic choice should be based on local resistance patterns and individual patient factors.
- Prevention: Preventive measures include good hygiene practices, respiratory etiquette, avoiding close contact with sick individuals, vaccination, maintaining a healthy lifestyle, and avoiding exposure to secondhand smoke.
- Risk Groups: M. catarrhalis infections are more common in children, the elderly, and individuals with respiratory ailments or compromised immune systems.
- Co-infections: M. catarrhalis infections often occur along with other respiratory pathogens, such as Streptococcus pneumoniae and Haemophilus influenzae.
- Antimicrobial Resistance: Antibiotic resistance is a growing concern with M. catarrhalis, emphasizing the need for judicious antibiotic use and ongoing research.
Further Readings
- “Pathogenesis and Immune Response in Moraxella catarrhalis Infections” – This topic delves into the mechanisms by which M. catarrhalis causes infections and how the host’s immune response reacts to the bacterium.
- “Antibiotic Resistance in Moraxella catarrhalis” – This area of research focuses on the emergence and prevalence of antibiotic resistance in M. catarrhalis and the implications for treatment strategies.
- “Epidemiology of Moraxella catarrhalis Infections” – This topic covers the prevalence, distribution, and risk factors associated with M. catarrhalis infections in different populations and geographic regions.
- “Virulence Factors of Moraxella catarrhalis” – This research area explores the various virulence factors employed by M. catarrhalis to cause infections and evade the host’s immune defenses.
- “Biofilm Formation and Persistence in Moraxella catarrhalis” – This topic focuses on the role of biofilm formation in chronic infections caused by M. catarrhalis and its implications for treatment.
- “Diagnostic Techniques for Moraxella catarrhalis” – This area covers the latest advancements in diagnostic methods, including molecular techniques and rapid tests for identifying M. catarrhalis infections.
- “Vaccine Development for Moraxella catarrhalis” – This research explores ongoing efforts to develop vaccines against M. catarrhalis to prevent infections and reduce their impact.
