Introduction
Table of Contents
Mucor is a genus of fungi belonging to the family Mucoraceae within the phylum Zygomycota. These fungi are commonly known as mold and are ubiquitous in the environment, found in soil, decaying organic matter, and on various surfaces. Mucor species play essential roles in ecosystem nutrient cycling as they are involved in the decomposition of organic material.
Characteristically, they exhibit fast growth rates, producing fluffy, cotton-like colonies with a white or light coloration. They reproduce asexually through the formation of spores, which are small, resistant structures that enable them to survive harsh environmental conditions.
One distinguishing feature of Mucor is its ability to form zygospores during sexual reproduction. Zygospores are thick-walled resting spores that form when two compatible hyphae of different mating types come together and fuse. This unique process gives the phylum Zygomycota its name.
While Mucor fungi are ecologically important, they can also be opportunistic pathogens. Immunocompromised individuals, such as those with weakened immune systems, diabetes, or other underlying health conditions, are particularly susceptible to Mucor infections, known as mucormycosis or zygomycosis. Mucormycosis can be a severe and potentially life-threatening condition if not treated promptly.
They (Mucor fungi)have drawn attention from researchers and scientists due to their potential applications in various biotechnological processes, including food fermentation, production of enzymes, and biofuel generation.
Morphology
The morphology of Mucor refers to the physical characteristics and structures of the fungi belonging to the genus Mucor. Here are the main features-
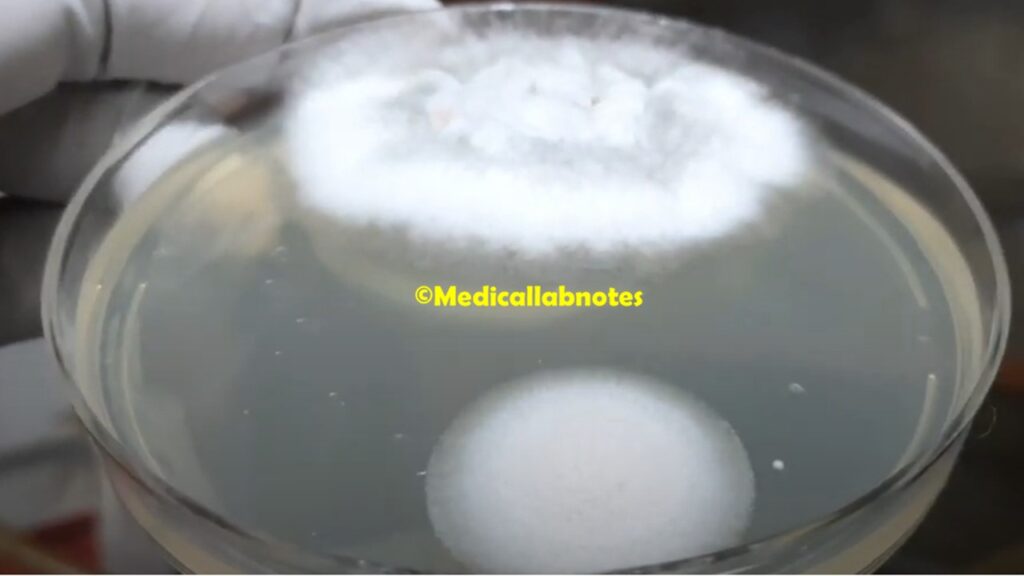
- Hyphae: They are composed of thread-like structures called hyphae. These hyphae are long, non-septate (lacking cross-walls), and coenocytic, which means they have multiple nuclei within a continuous cytoplasmic mass. This coenocytic nature allows for rapid nutrient and resource transport within the hyphae.
- Mycelium: The hyphae of Mucor form a complex network known as the mycelium. The mycelium spreads out and grows across the substrate, such as soil or decaying organic matter, to extract nutrients for the fungus.
- Sporangia: It produces specialized structures called sporangia, which are sac-like or spherical structures located at the tips of specialized hyphae called sporangiophores. The sporangia contain numerous spores inside, which are the reproductive units of the fungus.
- Spores: Spores are the primary mode of reproduction in Mucor. They are small, single-celled structures that are produced within the sporangia. When conditions are favorable, the sporangium bursts open, releasing the spores into the environment. These spores can disperse and germinate under suitable conditions to form new hyphae and mycelium.
- Zygospores: In addition to asexual spores, they can also produce zygospores through sexual reproduction. Zygospores are formed when two genetically different strains of Mucor come into contact and fuse their hyphae. This process leads to the formation of thick-walled, resting structures called zygospores, which can survive harsh environmental conditions until conditions become favorable for germination.
- Colonies: When grown on a solid medium, Mucor colonies appear fluffy, cotton-like, and may have a white, gray, or light coloration.

Pathogenicity
They can be opportunistic pathogens, meaning they typically cause infections in individuals with weakened immune systems or those with underlying health conditions. The most common form of infection is known as mucormycosis or zygomycosis. Here are some key points regarding the pathogenicity of Mucor:
- Host Susceptibility: Mucormycosis primarily affects individuals with compromised immune systems, such as those with poorly controlled diabetes, organ transplant recipients, cancer patients undergoing chemotherapy, individuals with HIV/AIDS, and those taking immunosuppressive medications. People with these conditions have a reduced ability to fight off fungal infections, making them more susceptible to Mucor infections.
- Infection Route: It enters the body through the inhalation of fungal spores present in the environment. Once inside the body, the spores can germinate and invade the host tissues, particularly in the nasal sinuses, lungs, skin, and brain.
- Angioinvasion and Tissue Necrosis: It has a unique ability to invade and damage blood vessels (angioinvasion). This invasion can lead to the destruction of blood vessel walls and the death of surrounding tissues (necrosis). The rapid spread of the infection can result in severe tissue damage and potential complications.
- Clinical Forms: Mucormycosis can manifest in different clinical forms, including:
- Rhinocerebral Mucormycosis: The most common form affecting the sinuses, nasal passages, and brain. It can be life-threatening, especially when the infection reaches the brain.
- Pulmonary Mucormycosis: Affecting the lungs, often seen in people with pre-existing lung conditions or those on mechanical ventilation.
- Cutaneous Mucormycosis: Affecting the skin after direct inoculation of spores through wounds or burns.
- Gastrointestinal Mucormycosis: Affecting the gastrointestinal tract, usually seen in people with compromised gut integrity.
- Rapid Progression: Mucormycosis can progress quickly, leading to severe tissue damage and systemic complications. Early diagnosis and prompt intervention are crucial for improving patient outcomes.
- Treatment: Treatment typically involves antifungal medications, such as amphotericin B, posaconazole, or isavuconazole. Surgical debridement of infected tissues may also be necessary to remove the affected areas and control the infection. Since mucormycosis often affects immunocompromised patients, addressing the underlying immune condition is vital for successful treatment.
Lab Diagnosis
The laboratory diagnosis of Mucor involves the identification of the fungal pathogen in patient samples. Since mucormycosis is a potentially life-threatening infection, a prompt and accurate diagnosis is crucial for initiating appropriate treatment. Here are the key steps involved in the lab diagnosis of Mucor:
- Clinical Evaluation: The first step is a thorough clinical evaluation of the patient. The healthcare provider will assess the patient’s medical history, risk factors for mucormycosis (e.g., immunocompromised status, diabetes, organ transplant, etc.), and any signs and symptoms they are experiencing.
- Sample Collection: To identify Mucor, samples are collected from the suspected infected site. The choice of the sample will depend on the clinical presentation of the infection:
- Rhinocerebral Mucormycosis: Samples from the nasal discharge, biopsy from nasal tissues, or cerebrospinal fluid (in cases of brain involvement).
- Pulmonary Mucormycosis: Respiratory secretions, bronchoalveolar lavage (BAL), or lung biopsy.
- Cutaneous Mucormycosis: Tissue biopsy from the affected skin area.
- Gastrointestinal Mucormycosis: Biopsy of gastrointestinal tissues.
- Microscopic Examination: The collected samples are then examined under a microscope. Mucor fungi appear as large, non-septate hyphae (coenocytic) with irregular branching. The presence of characteristic sporangia and sporangiospores can be indicative of Mucor infection.
- Culture: The collected samples can be cultured on appropriate fungal growth media, such as Sabouraud dextrose agar. They grow rapidly, and the colonies appear fluffy, cotton-like, and may have a white to light coloration. The culture helps confirm the presence of Mucor and also allows for species identification, which can be important for treatment decisions.
- Histopathology: In addition to culture and microscopy, histopathological examination of tissue samples obtained from biopsies can reveal the invasion of hyphae and presence of characteristic sporangia within the host tissues, confirming the diagnosis.
- Molecular Tests: In some cases, molecular techniques like polymerase chain reaction (PCR) may be used for a more rapid and specific identification of Mucor species.

Treatment
The treatment of Mucor, specifically mucormycosis, involves a multi-pronged approach that includes antifungal medications, surgical intervention, and addressing any underlying risk factors. Prompt and aggressive treatment is essential to improve patient outcomes, as mucormycosis can be a rapidly progressing and life-threatening infection. Here are the main components of the treatment:
- Antifungal Medications:
- Amphotericin B: Amphotericin B is the drug of choice for the treatment of mucormycosis. It is typically administered intravenously. Lipid formulations of amphotericin B are often preferred as they have less nephrotoxicity compared to conventional formulations. Amphotericin B works by disrupting the fungal cell membrane, leading to the death of the fungus.
- Posaconazole and Isavuconazole: These newer antifungal agents are also used for the treatment of mucormycosis, especially in cases where amphotericin B cannot be used or as a second-line option.
- Surgical Debridement: In many cases of mucormycosis, surgical intervention is necessary to remove the infected and necrotic tissues. This procedure is called surgical debridement. By removing the infected tissue, the spread of the fungus can be controlled, and it also helps in better penetration of antifungal medications to the remaining infected areas.
- Control of Underlying Risk Factors: Addressing the underlying risk factors, such as managing diabetes, reducing immunosuppressive therapy, or treating any other immunocompromising conditions, is crucial to improve the body’s ability to fight off the infection.
- Adjunct Therapies: In severe cases, patients may require additional supportive therapies, such as blood transfusions, wound care, and management of other complications resulting from the infection.
- Recovery and Follow-up: Recovery from mucormycosis can be a lengthy process, and patients may need to continue antifungal treatment for an extended period. Close monitoring and regular follow-up with healthcare providers are essential to assess the response to treatment and detect any signs of recurrence.

It’s important to note that early diagnosis and treatment significantly improve the chances of successful outcomes. Delayed treatment can lead to the progression of the infection and increase the risk of complications and mortality.
Prevention
Preventing mucormycosis involves several measures aimed at reducing the risk of exposure to Mucor fungi, especially in individuals who are more susceptible to fungal infections. Here are some preventive measures:
- Maintain Good Hygiene: Practicing good hygiene is essential to reduce the risk of fungal infections. Wash hands regularly with soap and water, especially after handling soil, gardening, or being in potentially contaminated environments.
- Control Underlying Health Conditions: Mucormycosis primarily affects individuals with weakened immune systems or underlying health conditions, such as poorly controlled diabetes or immunosuppression. Managing these conditions effectively, under the guidance of healthcare professionals, can help reduce the risk of infection.
- Diabetes Management: If you have diabetes, it’s crucial to maintain tight control of blood sugar levels. Elevated blood sugar levels can create a favorable environment for fungal growth and increase the risk of mucormycosis.
- Avoid Environmental Exposure: Individuals at higher risk of mucormycosis, such as those with compromised immunity, should avoid unnecessary exposure to environments where Mucor fungi may thrive. This includes avoiding construction sites, areas with decaying organic matter, and other potentially contaminated areas.
- Protective Clothing: If you work in environments where exposure to soil or other potential sources of Mucor is likely, consider wearing appropriate protective clothing, such as gloves, masks, and long-sleeved shirts, to minimize contact with fungal spores.
- Avoiding Contaminated Water: Avoid using water sources that might be contaminated with these fungi, especially for those with weakened immune systems. This includes avoiding the use of stagnant water or untreated water for drinking or cleaning wounds.
- Sterile Medical Equipment: In healthcare settings, proper sterilization of medical equipment and adherence to infection control protocols are crucial to prevent the spread of fungal infections.
- Prophylactic Antifungal Treatment: In some cases, high-risk individuals undergoing certain medical treatments, such as stem cell transplantation or chemotherapy, may be prescribed prophylactic antifungal medications to prevent fungal infections, including mucormycosis.
- Education and Awareness: Healthcare providers should be aware of the risk factors and clinical signs of mucormycosis to facilitate early diagnosis and treatment. Additionally, educating patients with underlying risk factors about preventive measures can help them take necessary precautions.
Keynotes
Here are some keynotes on Mucor:
- Genus Name: It is a genus of fungi belonging to the family Mucoraceae within the phylum Zygomycota.
- Morphology: They are characterized by their fast growth, fluffy, cotton-like colonies, and white to light-colored appearance. They have non-septate, coenocytic hyphae and reproduce both asexually through sporangiospores and sexually through zygospores.
- Ubiquitous Distribution: They are widespread and commonly found in soil, decaying organic matter, and various surfaces in the environment.
- Opportunistic Pathogen: Mucor can cause mucormycosis, which is an opportunistic infection primarily affecting individuals with weakened immune systems or underlying health conditions, such as uncontrolled diabetes or immunosuppression.
- Modes of Infection: Mucormycosis can occur through the inhalation of fungal spores, direct inoculation into wounds or burns, or ingestion of spores.
- Clinical Forms: Mucormycosis can present in various clinical forms, including rhinocerebral (sinuses and brain), pulmonary (lungs), cutaneous (skin), and gastrointestinal (gut).
- Angioinvasion and Necrosis: Mucor can invade blood vessels (angioinvasion), leading to necrosis of surrounding tissues, contributing to the rapid progression and severity of the infection.
- Treatment: The treatment of mucormycosis involves a combination of antifungal medications, such as amphotericin B, posaconazole, or isavuconazole, surgical debridement, and management of underlying risk factors.
- Prevention: Preventive measures for mucormycosis include good hygiene practices, controlling underlying health conditions, avoiding environmental exposure, wearing protective clothing in high-risk environments, and educating healthcare providers and at-risk individuals.
- Risk Groups: Individuals at higher risk of mucormycosis include those with poorly controlled diabetes, organ transplant recipients, cancer patients undergoing chemotherapy, individuals with HIV/AIDS, and those taking immunosuppressive medications.
Further Readings
- PubMed: PubMed is a comprehensive database of biomedical literature, and you can find numerous research articles and reviews on Mucor and mucormycosis by searching for relevant keywords.
- Medical Mycology Textbooks: Textbooks focused on medical mycology often cover various fungal infections, including mucormycosis. Look for books like “Clinical Mycology” by Elias J. Anaissie, Michael R. McGinnis, and Michael A. Pfaller or “Medical Mycology: A Self-Instructional Text” by Martha E. Kerns.
- Medical Journals: Journals like “Mycoses,” “Medical Mycology,” and “Mycopathologia” regularly publish research articles and reviews related to fungal infections, including mucormycosis.
- CDC (Centers for Disease Control and Prevention) Website: The CDC website offers valuable information on mucormycosis, its risk factors, prevention, and treatment options.
- Scientific Review Articles: Look for review articles written by experts in the field of mycology and infectious diseases. These articles summarize the current state of knowledge on mucormycosis and can provide in-depth insights.
- Mycology Conferences and Proceedings: Check out the proceedings and abstracts from conferences related to mycology and infectious diseases, as they often include the latest research on mucor and mucormycosis.
- University and Research Institution Websites: Academic institutions with strong mycology research departments may have publications and resources available online.
- Fungal Disease Databases: Explore online databases and repositories dedicated to fungal diseases, which may include specific information on Mucor species and mucormycosis.
