Introduction
Table of Contents
Serratia liquefaciens is a species of Gram-negative, rod-shaped bacteria belonging to the genus Serratia. This bacterium is known for its diverse distribution in various environmental niches, including water, soil, plants, and human-related habitats. It has also been associated with clinical infections in humans, making it of interest to both microbiologists and healthcare professionals.

Here’s an introduction to some key aspects of Serratia liquefaciens:
- Taxonomy: Serratia liquefaciens is classified within the family Enterobacteriaceae, which includes other well-known genera like Escherichia, Salmonella, and Klebsiella. This family comprises Gram-negative bacteria that are often found in the gastrointestinal tracts of humans and animals.
- Physiological Characteristics: Serratia liquefaciens is facultatively anaerobic, which means it can grow in the presence or absence of oxygen.
- Environmental Distribution: This bacterium is widely distributed in the environment and can be found in water sources, soil, and plants. It has the ability to degrade various organic compounds and has been studied for its potential in bioremediation.
- Pathogenicity: While Serratia liquefaciens is generally considered to be of low virulence, it has been associated with opportunistic infections in humans, particularly in healthcare settings. These infections may include urinary tract infections, respiratory tract infections, and bloodstream infections. Infections are more common in immunocompromised individuals.
- Antibiotic Resistance: Like other members of the Serratia genus, Serratia liquefaciens can develop antibiotic resistance, which poses challenges in clinical settings. Monitoring antibiotic susceptibility is crucial for effective treatment.
- Research and Biotechnology: Beyond its clinical implications, It has been studied for its potential in biotechnology and genetic research. It can serve as a model organism for understanding various genetic and metabolic processes.
- Genome Sequencing: Advances in genome sequencing technology have enabled the study of Serratia liquefaciens at the genomic level, providing insights into its genetic diversity and potential functions.
Morphology
he morphology of Serratia liquefaciens refers to its physical characteristics and appearance under the microscope. Serratia liquefaciens is a Gram-negative bacterium, and its morphology can be described as follows:

- Cell Shape: Serratia liquefaciens is typically rod-shaped or bacillary. This means that its cells are elongated and cylindrical in shape.
- Cell Size: The size of Serratia liquefaciens cells can vary, but they are generally about 0.5 to 1.0 micrometers in width and 1.5 to 4.0 micrometers in length.
- Gram Stain: Serratia liquefaciens is Gram-negative. This means that it does not retain the crystal violet stain during Gram staining and appears pink or red under the microscope.
- Cell Arrangement: Cells of Serratia liquefaciens typically occur singly or in pairs, although they can also form short chains or clusters. They do not usually form the long chains characteristic of some other bacteria like Streptococcus species.
- Motility: Serratia liquefaciens is usually motile due to the presence of flagella. This motility allows the bacterium to move actively in liquid environments.
- Capsule: Some strains of Serratia liquefaciens may produce a polysaccharide capsule, which is a protective layer outside the cell wall.
- Endospore Formation: It is non-spore-forming, meaning it does not produce endospores as seen in some other bacterial species.
Pathogenicity
Serratia liquefaciens is a bacterium that can be considered an opportunistic pathogen, meaning it typically causes infections in individuals with weakened immune systems or underlying medical conditions. While not as well-known as some other pathogenic bacteria, S. liquefaciens can still be associated with various clinical infections and has the potential for pathogenicity. Here are some key aspects of its pathogenicity:
- Infections in Immunocompromised Individuals: Serratia liquefaciens infections are more common in individuals who have compromised immune systems, such as those with chronic illnesses, immunosuppressive therapy, or other predisposing factors. This includes patients in healthcare settings and those with severe underlying diseases.
- Infectious Sites: Serratia liquefaciens can cause a range of infections, including urinary tract infections (UTIs), respiratory tract infections (e.g., pneumonia), bloodstream infections (bacteremia), wound infections, and infections associated with medical devices (catheters, ventilators, etc.).
- Nosocomial Infections: S. liquefaciens is often associated with healthcare-associated infections (nosocomial infections), particularly in intensive care units and surgical wards. Contaminated medical equipment and poor infection control practices can contribute to its transmission.
- Antibiotic Resistance: Some strains of S. liquefaciens have developed antibiotic resistance, including resistance to commonly used antibiotics such as penicillins, cephalosporins, and aminoglycosides. This resistance can complicate treatment.
- Virulence Factors: Serratia species, including Serratia liquefaciens, possess various virulence factors that enable them to cause disease. These may include adhesins, toxins, and mechanisms for evading the host immune system.
- Biofilm Formation: S. liquefaciens can form biofilms on medical devices, making it more challenging to eradicate the infection. Biofilms protect bacteria from host defenses and antibiotics.
- Endotoxin Production: Like many Gram-negative bacteria, Serratia liquefaciens can produce endotoxins (lipopolysaccharides) that contribute to the inflammatory response in the host.
- Inflammatory Response: Infections with S. liquefaciens can trigger an inflammatory response, leading to symptoms such as fever, localized pain, and increased white blood cell counts.
- Treatment Challenges: Due to its potential for antibiotic resistance and the need for appropriate antibiotic therapy, the treatment of S. liquefaciens infections can be challenging. Susceptibility testing is crucial for guiding therapy.
- Prevention: Preventing Serratia liquefaciens infections involves strict adherence to infection control practices in healthcare settings, including hand hygiene, sterilization of medical equipment, and surveillance for outbreaks.
Lab Diagnosis
The laboratory diagnosis of Serratia liquefaciens typically involves a series of microbiological and biochemical tests to identify and characterize the bacterium. Here are the key steps and methods involved in the lab diagnosis of S. liquefaciens:

- Sample Collection: The first step is to obtain a clinical specimen, such as blood, urine, sputum, or a wound swab, from a patient suspected of having an infection caused by S. liquefaciens.
- Culturing: The collected specimen is streaked onto appropriate culture media. Common media for Serratia species include MacConkey agar, blood agar, and nutrient agar. It may also grow on selective media specific to Enterobacteriaceae.
- Incubation: The culture plates are incubated at a suitable temperature (typically 35-37°C) for 18-24 hours to allow bacterial growth.
- Colonial Morphology: After incubation, the colonies are examined for their appearance, size, shape, color, and other characteristics.
- Gram Staining: A Gram stain is performed to determine the Gram reaction of the bacteria. Serratia liquefaciens is Gram-negative, so it will appear pink or red under the microscope.
- Biochemical Tests:
- Oxidase Test: Serratia liquefaciens is typically oxidase-negative.
- Catalase Test: It is positive for catalase activity.
- Indole Test: It is usually indole-negative.
- Triple Sugar Iron (TSI) Agar Test: This test assesses the ability of the bacterium to ferment sugars and produce gas. S. liquefaciens typically shows an alkaline slant and acid butt with no gas production.
- Methyl Red and Voges-Proskauer (MR-VP) Test: These tests help differentiate between different Enterobacteriaceae. S. liquefaciens is often MR-negative and VP-negative.
- Citrate Utilization Test: Serratia liquefaciens is usually citrate-positive.
- API or Analytical Profile Index System: Commercial identification kits like the API system may be used for more accurate species identification. These kits are based on the reactions of the bacterium to various biochemical tests.
- Antibiotic Susceptibility Testing: The antibiotic susceptibility of S. liquefaciens should be determined using methods like disk diffusion or automated systems. This is important for guiding appropriate antibiotic therapy.
- Molecular Identification: In some cases, molecular techniques such as polymerase chain reaction (PCR) and DNA sequencing may be employed to confirm the identity of S. liquefaciens, especially if more precise identification is required.
- Serotyping: Serratia species can be serotyped based on their surface antigens, but this is not commonly performed in routine clinical settings.
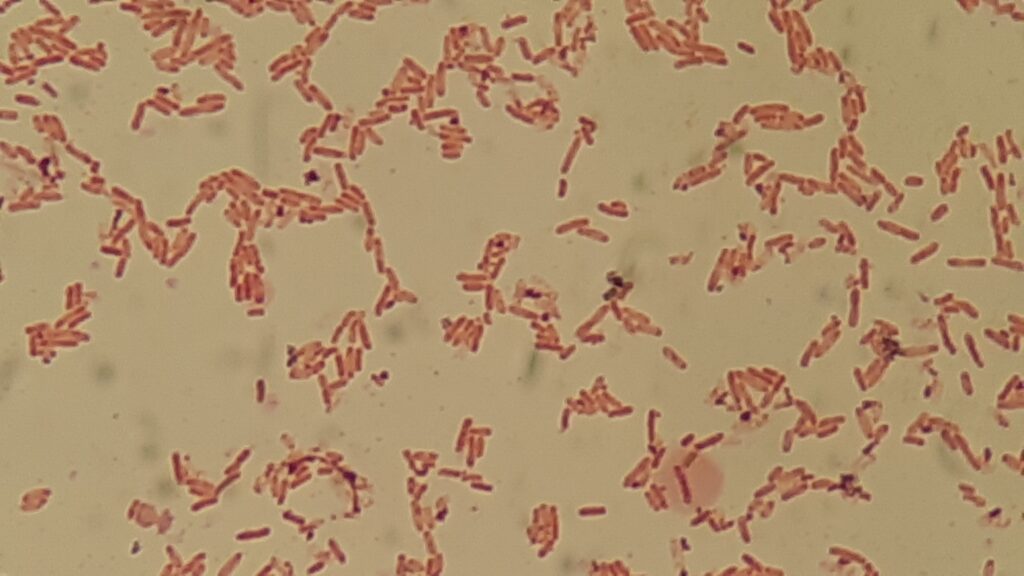
It’s essential to conduct these diagnostic tests in a clinical microbiology laboratory, and the results should be interpreted by trained microbiologists. Identification of Serratia liquefaciens helps guide appropriate treatment in cases of infection and contributes to the understanding of the epidemiology and antibiotic resistance of this bacterium.
Treatment
The treatment of Serratia liquefaciens infections typically involves antibiotic therapy. However, the choice of antibiotics and the duration of treatment may vary depending on the site and severity of the infection, as well as the antibiotic susceptibility of the specific strain of S. liquefaciens. Here are some general considerations for the treatment of Serratia liquefaciens infections:
- Antibiotic Susceptibility Testing: It is crucial to perform antibiotic susceptibility testing on the isolated strain of Serratia liquefaciens to determine which antibiotics are effective against it. Serratia species are known for their potential resistance to multiple antibiotics, so the choice of antibiotics should be guided by susceptibility results.
- Empirical Therapy: In some cases, initial antibiotic therapy may be started empirically before susceptibility results are available. However, it is important to adjust the treatment based on susceptibility data once it becomes available.
- Combination Therapy: In severe infections or cases of bacteremia, combination antibiotic therapy may be considered. This involves using two or more antibiotics with different mechanisms of action to increase the likelihood of effective treatment.
- Duration of Treatment: The duration of antibiotic treatment depends on the type and location of the infection. For uncomplicated urinary tract infections (UTIs), a shorter course of antibiotics may be sufficient, whereas more serious infections may require a longer course.
- Intravenous vs. Oral Therapy: The route of administration (intravenous or oral) depends on the severity of the infection. Severe infections or cases of bacteremia often require intravenous antibiotics, while less severe infections can be treated with oral antibiotics.
- Monitoring: Patients undergoing antibiotic therapy for Serratia liquefaciens infections should be closely monitored for clinical improvement. In cases of bacteremia or other serious infections, blood cultures should be repeated to confirm clearance of the infection.
- Infection Control: In healthcare settings, infection control measures are essential to prevent the spread of Serratia liquefaciens and other healthcare-associated infections. This includes strict hand hygiene, proper disinfection of medical equipment, and isolation of infected patients when necessary.
- Biofilm-Related Infections: In cases where S. liquefaciens has formed biofilms on medical devices (e.g., catheters or prosthetic devices), removal or replacement of the contaminated device may be necessary in addition to antibiotic therapy.
- Consulting an Infectious Disease Specialist: In complex or recurrent cases of Serratia liquefaciens infections, consultation with an infectious disease specialist is advisable to optimize treatment and management.
Prevention
Preventing Serratia liquefaciens infections involves a combination of infection control measures, both in healthcare settings and in the community. Here are some key strategies for preventing S. liquefaciens infections:
In Healthcare Settings:
- Hand Hygiene: Healthcare workers should practice thorough hand hygiene with soap and water or alcohol-based hand sanitizers before and after patient contact. Proper handwashing is one of the most effective ways to prevent the spread of bacteria, including S. liquefaciens.
- Infection Control Practices: Strict adherence to infection control protocols, including the use of personal protective equipment (e.g., gloves, gowns, masks, and eye protection), is crucial when caring for patients with known or suspected S. liquefaciens infections.
- Environmental Cleaning: Regular and thorough cleaning and disinfection of patient care areas and medical equipment are essential. Serratia liquefaciens can survive on surfaces, so effective disinfection is critical to prevent transmission.
- Isolation Precautions: Implement isolation precautions when necessary, especially for patients with known or suspected S. liquefaciens infections. This may involve placing the patient in a private room and using additional precautions as appropriate.
- Proper Sterilization: Ensure that medical equipment and devices are properly sterilized before use. Contaminated medical equipment can be a source of infection.
- Antibiotic Stewardship: Healthcare facilities should have antibiotic stewardship programs in place to promote the judicious use of antibiotics. Overuse or misuse of antibiotics can contribute to the development of antibiotic-resistant strains of bacteria, including S. liquefaciens.
In the Community:
- Hand Hygiene: Practice good hand hygiene in everyday life, particularly before eating and after using the restroom. This helps prevent the spread of bacteria from contaminated surfaces to the mouth and nose.
- Food Safety: Follow safe food handling practices to prevent foodborne illnesses. Proper cooking, storage, and hygiene when handling food are essential.
- Personal Hygiene: Maintain good personal hygiene, including regular bathing and changing of clothes. This can help reduce the risk of skin and wound infections.
- Avoid Close Contact with Ill Individuals: If someone in your household or community is sick with an infection, take precautions to avoid close contact to prevent transmission.
- Environmental Cleanliness: Keep living spaces and shared areas clean and well-maintained to reduce the presence of potential sources of infection.
- Vaccination: Ensure that you and your family are up-to-date with recommended vaccinations. Some vaccines protect against specific bacterial infections that can cause illness.
- Responsible Antibiotic Use: If prescribed antibiotics, take them exactly as directed by a healthcare professional. Never use antibiotics without a prescription, and complete the full course of treatment, even if you feel better.
Keynotes
here are key points to note about S. liquefaciens:
- Classification: It is a Gram-negative bacterium belonging to the genus Serratia within the family Enterobacteriaceae.
- Morphology: It has a rod-shaped (bacillary) morphology and is typically motile due to the presence of flagella.
- Environmental Distribution: It is commonly found in various environmental niches, including soil, water, plants, and human-related habitats.
- Pathogenicity: Serratia liquefaciens is considered an opportunistic pathogen, causing infections primarily in immunocompromised individuals. Infections can include urinary tract infections, respiratory tract infections, bloodstream infections, wound infections, and infections associated with medical devices.
- Nosocomial Infections: It is often associated with healthcare-associated infections (nosocomial infections), particularly in intensive care units and surgical wards.
- Antibiotic Resistance: Some strains of S. liquefaciens have developed antibiotic resistance, making treatment challenging.
- Virulence Factors: It possesses various virulence factors, including adhesins and toxins, that contribute to its ability to cause disease.
- Biofilm Formation: S. liquefaciens can form biofilms on medical devices, complicating infection control and treatment.
- Endotoxin Production: Like other Gram-negative bacteria, it can produce endotoxins (lipopolysaccharides).
- Infection Control: Strict infection control practices, such as hand hygiene, disinfection of medical equipment, and isolation precautions, are essential in healthcare settings to prevent its spread.
- Treatment: Effective treatment involves antibiotic therapy guided by susceptibility testing. In severe infections, combination therapy may be considered. Removal of contaminated medical devices may be necessary.
- Prevention: Preventing Serratia liquefaciens infections includes general infection control measures, antibiotic stewardship, and environmental cleanliness in healthcare and community settings.
- Community Infections: In the community, maintaining good personal hygiene, practicing food safety, and avoiding close contact with ill individuals can help reduce the risk of infection.
- Vaccination: Ensuring up-to-date vaccinations against specific bacterial infections can offer protection.
- Responsible Antibiotic Use: Responsible use of antibiotics, including completing the full course of treatment as prescribed, is essential to prevent antibiotic resistance.
Further Readings
- Scientific Journals: Explore research articles and reviews related to Serratia liquefaciens in microbiology, clinical microbiology, and infectious diseases journals. Some journals to consider include:
- “Journal of Clinical Microbiology”
- “Microbiology and Immunology”
- “Infection Control & Hospital Epidemiology”
- “Antimicrobial Agents and Chemotherapy”
- “Frontiers in Microbiology”
- Textbooks: Look for microbiology textbooks that cover the Serratia genus and its various species. These textbooks often provide in-depth information on morphology, physiology, pathogenicity, and laboratory identification. Examples include “Brock Biology of Microorganisms” and “Manual of Clinical Microbiology.”
- Public Health and Clinical Guidelines: Check guidelines and recommendations from healthcare organizations and public health agencies regarding the prevention and management of healthcare-associated infections and antibiotic resistance. These guidelines often include information on Serratia species.
- Online Resources:
- Explore websites and databases such as the Centers for Disease Control and Prevention (CDC) or the World Health Organization (WHO) for information on antibiotic resistance, infection prevention, and global health trends related to Serratia species.
- Academic institutions often provide resources and publications related to clinical microbiology and infectious diseases. Look for university-affiliated websites and research centers specializing in microbiology.
- PubMed: Use the PubMed database to search for specific research articles and reviews related to Serratia liquefaciens. You can refine your search by using keywords like “Serratia liquefaciens pathogenicity,” “Serratia liquefaciens antibiotic resistance,” or “Serratia liquefaciens epidemiology.”
- Microbiology Conferences: Review presentations and abstracts from microbiology conferences, as they may include the latest research findings on Serratia species. Conferences like the American Society for Microbiology (ASM) Microbe and the International Congress of Bacteriology and Applied Microbiology cover topics related to microbial pathogens.
- Medical and Microbiology Texts: Investigate medical textbooks and microbiology reference texts for comprehensive information on Serratia liquefaciens and its clinical significance.
