Introduction
Table of Contents
Streptococcus oralis is a gram-positive bacterium that belongs to the genus Streptococcus. It is a commensal bacterium that commonly inhabits the human oral cavity, along with other oral streptococci. S. oralis is considered a part of the normal oral microbiota and can be found in dental plaque, saliva, and various oral surfaces.
The oral cavity is a complex environment with diverse microbial communities, and S. oralis is one of the predominant species found in this ecosystem. It is primarily found on the teeth, tongue, and mucosal surfaces of the mouth. S. oralis has a symbiotic relationship with its host, as it helps maintain oral health by competing with potentially harmful bacteria and contributing to the balance of the oral microbiota.
However, under certain circumstances, S. oralis can become pathogenic and cause infections. It has been associated with various infections, including dental caries (tooth decay), endocarditis (inflammation of the heart lining and valves), and other systemic infections. In immunocompromised individuals or those with underlying health conditions, S. oralis infections can be more severe.
It is part of a larger group of oral streptococci known as the “viridans streptococci.” These bacteria are characterized by their ability to produce a greenish discoloration of the blood agar, hence the name “viridans,” meaning green. The viridans streptococci are a diverse group of bacteria that play important roles in oral health and diseases.
Research on S. oralis is ongoing to better understand its pathogenic mechanisms, interactions with other oral bacteria, and its role in various infections. Advances in molecular techniques and genomic studies have provided insights into the virulence factors and genetic diversity of S. oralis strains, aiding in the development of diagnostic tools and potential therapeutic interventions.

Morphology
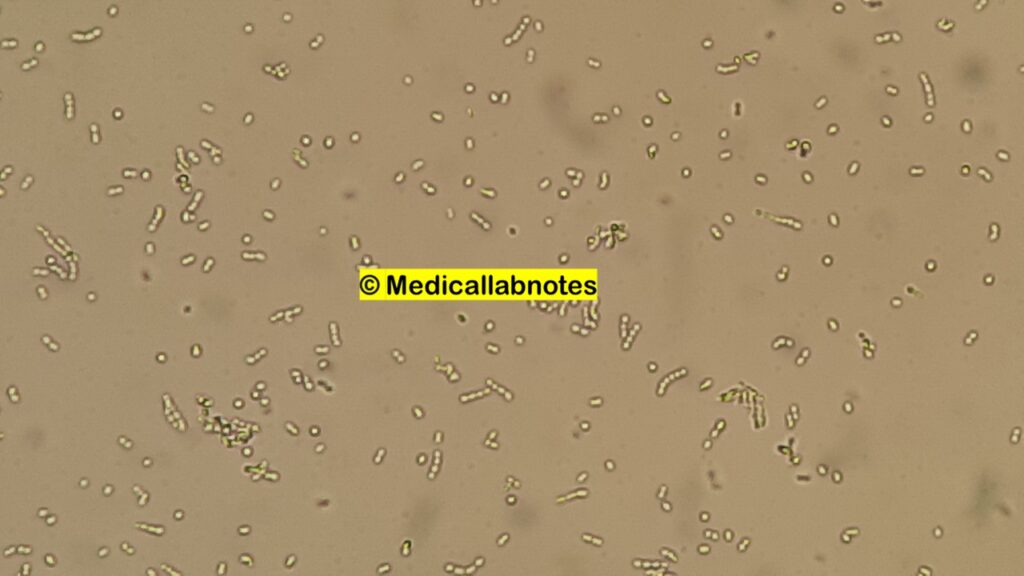
Streptococcus oralis is a gram-positive bacterium that exhibits a characteristic morphology consistent with other members of the Streptococcus genus. Here is an overview of the morphology of Streptococcus oralis:
- Shape: S. oralis typically appears as small, non-motile cocci (spherical cells). Cocci are round-shaped bacteria.
- Arrangement: Its cells can arrange themselves in pairs (diplococci), short chains (streptococci), or form clusters or aggregates.
- Size: The size of individual S. oralis cells can vary, but they generally have a diameter ranging from 0.5 to 1.0 micrometers.
- Gram Staining: S. oralis stains purple when subjected to the Gram staining method, indicating that it has a thick peptidoglycan layer in its cell wall and retains the crystal violet dye.
- Capsule: Some strains of it can produce a capsule, which is an outer layer of polysaccharides or proteins that surrounds the bacterial cell. The capsule can play a role in protecting the bacterium from the host’s immune system.
- Colony Morphology: Its colonies on agar plates typically appear as small, smooth, and round colonies with a slight indentation in the center. The colonies may exhibit different colors depending on the specific strain.
Pathogenicity
Streptococcus oralis, although considered a commensal bacterium in the oral cavity, can also exhibit pathogenic behavior under certain conditions. Here are some aspects of the pathogenicity of Streptococcus oralis:
- Endocarditis: It is one of the leading causative agents of infective endocarditis, which is an infection of the heart valves or lining. It can enter the bloodstream during dental procedures or due to oral infections, and if it reaches the heart, it can cause inflammation and damage to the heart valves.
- Dental Caries: It is associated with dental caries, commonly known as tooth decay. It can metabolize carbohydrates from the diet and produce acids as byproducts, leading to demineralization of tooth enamel and the formation of cavities.
- Systemic Infections: In immunocompromised individuals or those with underlying health conditions, S. oralis can cause systemic infections. These infections can manifest as bacteremia (presence of bacteria in the bloodstream), sepsis, and infections in distant sites such as the lungs, joints, or central nervous system.
- Biofilm Formation: It has the ability to form biofilms, which are structured communities of bacteria enclosed in a self-produced matrix. Biofilms provide protection against antimicrobial agents and host immune responses, making infections more difficult to treat. S. oralis biofilms can contribute to dental plaque formation and increase the risk of dental diseases.
- Virulence Factors: It possesses various virulence factors that contribute to its pathogenicity. These include adhesins that help the bacterium attach to host tissues, enzymes that facilitate tissue invasion and degradation, and toxins that can damage host cells and promote inflammation.
It is important to note that the pathogenic potential of Streptococcus oralis can vary among different strains and in different host environments. Factors such as the individual’s immune status, oral hygiene practices, and the presence of other pathogenic bacteria in the oral microbiota can influence the likelihood and severity of infections caused by S. oralis.
Lab Diagnosis
The laboratory diagnosis of Streptococcus oralis infections typically involves the isolation and identification of the bacterium from clinical samples. Here is an overview of the laboratory diagnostic methods commonly used for the detection and identification of Streptococcus oralis:
- Sample Collection: Clinical samples are collected based on the suspected site of infection. These may include blood samples in cases of bacteremia or endocarditis, oral swabs or dental plaque samples for oral infections, or samples from other affected sites such as joints or cerebrospinal fluid.
- Culture: The primary method for isolating Streptococcus oralis is by culturing the bacteria on appropriate growth media. Blood agar plates or chocolate agar plates supplemented with blood are commonly used. Clinical specimens are streaked onto the agar plates and incubated under optimal conditions, usually at 37°C with 5-10% CO2 for 24-48 hours.
- Gram Staining: After incubation, a Gram stain is performed on suspected colonies to confirm the presence of gram-positive cocci, which is consistent with Streptococcus oralis. Gram staining can provide initial information about the morphology and arrangement of the bacteria.
- Biochemical Tests: Biochemical tests are performed to further identify and confirm the presence of Streptococcus oralis. These tests may include catalase test (S. oralis is catalase-negative), hemolysis patterns on blood agar (S. oralis typically exhibits alpha-hemolysis, which appears as a greenish discoloration), and carbohydrate fermentation tests.
- Antibiotic Susceptibility Testing: Once the identification of Streptococcus oralis is confirmed, antibiotic susceptibility testing is performed to determine the most effective antibiotic for treatment. The standardized methods, such as disk diffusion or broth microdilution, are used to assess the susceptibility of the isolate to different antibiotics.
- Molecular Techniques: In some cases, molecular techniques such as polymerase chain reaction (PCR) may be employed to detect and identify specific genes or genetic markers associated with Streptococcus oralis. These techniques can provide rapid and accurate identification of the bacterium.

It’s worth noting that the laboratory diagnostic methods may vary depending on the specific resources and capabilities of the laboratory. Additionally, the interpretation of results should be done by trained professionals who can consider the clinical context and epidemiological factors.
Treatment
The treatment of Streptococcus oralis infections typically involves the use of antibiotics to target and eliminate the bacterial infection. The choice of antibiotics may vary depending on the specific infection site, severity, and the susceptibility of the bacterial strain to different antimicrobial agents. It’s important to note that the selection of antibiotics should be based on the guidance of a healthcare professional, taking into account factors such as local resistance patterns and individual patient factors. Here are some commonly used antibiotics for treating Streptococcus oralis infections:
- Penicillin: Streptococcus oralis is generally susceptible to penicillin and its derivatives, such as amoxicillin. These antibiotics inhibit the bacterial cell wall synthesis, leading to bacterial cell death. Penicillin is often the drug of choice for treating S. oralis infections, especially in cases of endocarditis or other systemic infections.
- Cephalosporins: Cephalosporin antibiotics, such as ceftriaxone or cefotaxime, may be used as an alternative to penicillin in individuals with penicillin allergies or when penicillin resistance is suspected. Cephalosporins have a similar mode of action to penicillin and can effectively target Streptococcus oralis.
- Macrolides: Macrolide antibiotics, including erythromycin, clarithromycin, or azithromycin, are sometimes prescribed for individuals with penicillin allergies or when resistance to penicillin is detected. Macrolides inhibit bacterial protein synthesis and can be effective against Streptococcus oralis.
- Vancomycin: Vancomycin is a potent antibiotic that is reserved for the treatment of severe infections caused by methicillin-resistant Streptococcus oralis strains or in cases where resistance to other antibiotics is suspected. Vancomycin is usually administered intravenously.
The duration of antibiotic treatment depends on the type and severity of the infection. In cases of endocarditis or other systemic infections, a prolonged course of treatment, typically 4-6 weeks or longer, may be necessary to ensure complete eradication of the bacteria.
Prevention
Preventing Streptococcus oralis infections primarily involves maintaining good oral hygiene practices and implementing preventive measures to minimize the risk of transmission. Here are some key preventive strategies:
- Oral Hygiene: Maintain proper oral hygiene practices, including regular brushing of teeth at least twice a day with fluoride toothpaste, flossing daily, and using an antimicrobial mouthwash. These practices help remove dental plaque and reduce the growth of Streptococcus oralis and other oral bacteria.
- Dental Care: Schedule regular dental check-ups and cleanings with a dentist or dental hygienist. Professional cleanings help remove plaque and tartar buildup, reducing the risk of dental caries and gum disease.
- Healthy Lifestyle: Adopt a healthy lifestyle that supports a strong immune system. Eat a balanced diet, exercise regularly, get sufficient sleep, and manage stress effectively. A robust immune system helps in preventing infections, including Streptococcus oralis.
- Avoid Smoking and Tobacco Use: Smoking and tobacco use can compromise oral health and weaken the immune system, making the oral cavity more susceptible to infections, including those caused by Streptococcus oralis. Quitting smoking or avoiding tobacco products is beneficial for overall oral health.
- Dental Procedures: Follow proper infection control measures during dental procedures to minimize the risk of transmission of Streptococcus oralis and other infectious agents. Dentists and dental healthcare professionals should adhere to strict sterilization and disinfection protocols.
- Endocarditis Prophylaxis: Individuals at high risk of developing infective endocarditis, such as those with pre-existing heart conditions, may need antibiotic prophylaxis before certain dental procedures. The purpose is to prevent bacteria, including Streptococcus oralis, from entering the bloodstream and causing infections in the heart. It is essential to consult with a healthcare provider to determine if prophylactic antibiotics are necessary in specific cases.
- Healthy Habits for Children: Encourage good oral hygiene practices in children from an early age. Teach them proper toothbrushing techniques, supervise their oral care routine, and limit their consumption of sugary foods and beverages. Regular dental check-ups for children are also important to identify and address any oral health issues.
- Avoid Sharing Personal Items: Avoid sharing toothbrushes, dental floss, or other personal oral care items, as these can potentially transmit bacteria, including Streptococcus oralis.
- Immunization: Follow recommended immunization schedules to protect against specific infections that can contribute to the development of oral diseases or compromise oral health.
Keynotes
- Streptococcus oralis is a gram-positive bacterium commonly found in the human oral cavity as a part of the normal oral microbiota.
- It can exist as a commensal bacterium, contributing to oral health, but can also become pathogenic under certain conditions.
- S. oralis is associated with infections such as dental caries (tooth decay), endocarditis, and other systemic infections.
- It is a member of the viridans streptococci, a group of oral streptococci that share similar characteristics.
- It exhibits a characteristic morphology of gram-positive cocci and can arrange in pairs, short chains, or clusters.
- Laboratory diagnosis involves sample collection, culture on appropriate media, Gram staining, biochemical tests, and sometimes molecular techniques for identification.
- Treatment typically involves antibiotics such as penicillin, cephalosporins, or macrolides, depending on the susceptibility and site of infection.
- Prevention of Streptococcus oralis infections includes maintaining good oral hygiene practices, regular dental check-ups, avoiding tobacco use, and following infection control measures during dental procedures.
- Individuals at high risk of infective endocarditis may require antibiotic prophylaxis before certain dental procedures.
- Streptococcus oralis infections can be prevented and managed effectively through a combination of oral health care, healthy lifestyle practices, and appropriate medical interventions.
- Seeking professional healthcare advice and adhering to prescribed treatments are crucial for the management of Streptococcus oralis infections.

Further Readings
- Kilian, M., & Tannock, G. W. (Eds.). (2011). Streptococcus: Molecular and Functional Aspects. Caister Academic Press. This book provides a comprehensive overview of the genus Streptococcus, including Streptococcus oralis, covering various aspects of its molecular biology, pathogenesis, and clinical significance.
- Nobbs, A. H., & Jenkinson, H. F. (2015). Interkingdom Networking within the Oral Microbiome. Microbes and Infection, 17(7), 484-492. This review article explores the interactions between Streptococcus oralis and other microorganisms within the oral microbiome, highlighting the importance of interkingdom communication.
- Wyss, C., & Choi, B. K. (2018). Streptococcus oralis. In: Ferretti JJ, Stevens DL, Fischetti VA, editors. Streptococcus pyogenes: Basic Biology to Clinical Manifestations. University of Oklahoma Health Sciences Center. This chapter provides insights into the pathogenesis, virulence factors, and clinical manifestations associated with Streptococcus oralis.
- Loo, C. Y., Mitrakul, K., Voss, I. B., & Hughes, C. V. (2019). Novel Applications of Streptococcus oralis for Biotechnological and Medical Purposes. Journal of Oral Microbiology, 11(1), 1551595. This article explores the potential biotechnological and medical applications of Streptococcus oralis, including probiotic and vaccine development.
- Chaffin, W. L. (2020). Viridans Streptococcal Infections. In: Bennett JE, Dolin R, Blaser MJ, editors. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases (9th ed.). Elsevier. This chapter provides a broader perspective on viridans streptococcal infections, including Streptococcus oralis, within the context of infectious diseases.

Good post. I study something tougher on completely different blogs everyday. It would all the time be stimulating to read content material from other writers and apply a little bit something from their store. I’d favor to use some with the content on my blog whether you don’t mind. Natually I’ll provide you with a link in your internet blog. Thanks for sharing.