Introduction
Table of Contents
Strongyloides is a genus of parasitic nematodes (roundworms) that includes the species Strongyloides stercoralis, commonly known as the human threadworm or threadworm. These tiny worms are parasitic in nature and can infect humans and other animals.
Here is an introduction to Strongyloides:
- Life Cycle: The life cycle of Strongyloides involves both free-living and parasitic stages. In the parasitic phase, the infective larvae penetrate the skin of a human host (or other suitable animals) and migrate through the bloodstream to the lungs. From there, they ascend to the throat, get swallowed, and reach the small intestine. In the intestine, the worms mature into adult females, which produce eggs that hatch into larvae. Some of these larvae are excreted in the feces, while others can re-infect the host by penetrating the intestinal wall or perianal skin, completing the cycle.
- Geographic Distribution: Strongyloides infections are prevalent in tropical and subtropical regions, including parts of Southeast Asia, sub-Saharan Africa, Latin America, and the Pacific Islands. However, cases have been reported worldwide due to travel and migration.
- Modes of Transmission: The primary mode of transmission of Strongyloides is through contact with contaminated soil. Infective larvae present in the soil can penetrate the skin of individuals who come into contact with it, leading to infection. In some cases, transmission can also occur through direct contact with contaminated material, such as clothing or bedding.
- Clinical Manifestations: Strongyloides infections can vary widely in their clinical presentation. Many infected individuals may remain asymptomatic or experience mild, transient symptoms. However, in immunocompromised individuals or in cases of heavy infection, the worms can cause a range of symptoms, including abdominal pain, diarrhea, weight loss, cough, and respiratory issues. In severe cases, dissemination of larvae throughout the body can lead to potentially life-threatening conditions, such as hyperinfection syndrome or disseminated strongyloidiasis.
- Diagnosis: The diagnosis of Strongyloides infection is typically made by examining stool samples for the presence of larvae. However, due to the intermittent shedding of larvae in feces, multiple stool samples may be necessary to increase the chances of detection. Serological tests that detect antibodies against Strongyloides can also be used for diagnosis.
- Treatment: The primary treatment for Strongyloides infection is the use of antiparasitic medications, most commonly ivermectin or albendazole. Treatment is usually administered for several days to eliminate the adult worms and larvae. In severe cases or when hyperinfection syndrome is present, treatment may require longer courses of medication and close monitoring.
- Prevention: Preventive measures for Strongyloides infection include avoiding direct contact with contaminated soil, wearing protective clothing, practicing good hygiene (such as handwashing), and treating infected individuals promptly to prevent transmission.
Morphology
Strongyloides is a genus of parasitic nematodes, commonly known as threadworms or thread-like worms, that infect humans and various other animals. The most well-known species within this genus is Strongyloides stercoralis, which is the causative agent of strongyloidiasis.
The morphology of Strongyloides can be described as follows:
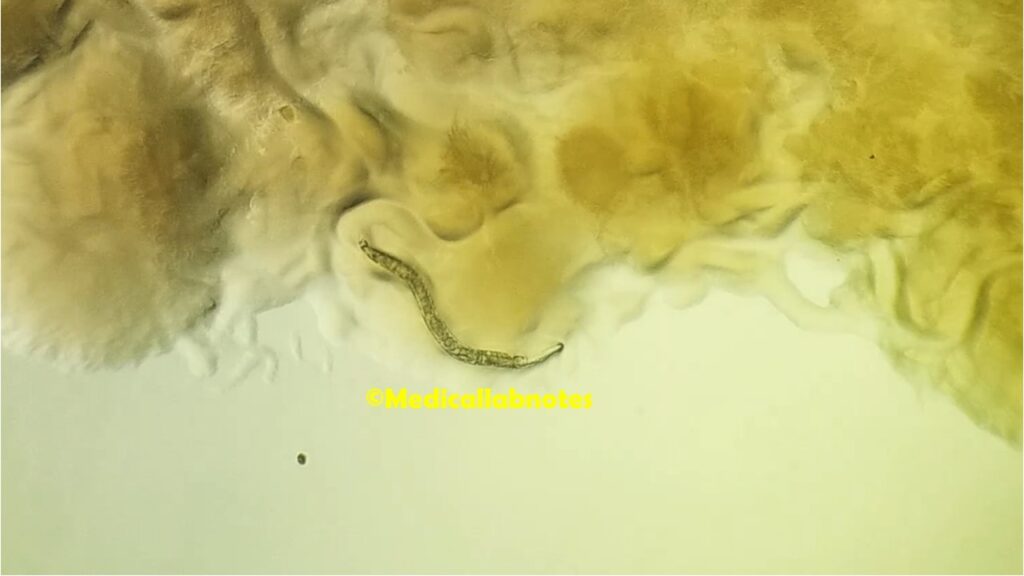
- Size: Adult female worms are typically smaller than adult males. Female worms measure approximately 2-3 mm in length, while males are slightly smaller, measuring around 1-2 mm.
- Shape: Both male and female worms have a slender, thread-like appearance. They are cylindrical in shape, with tapered ends.
- Cuticle: The outer surface of Strongyloides worms is covered by a thin, transparent cuticle that helps protect them from the host’s immune response.
- Mouthparts: The anterior end of the worms features a buccal cavity with a mouth surrounded by lips. The mouthparts are adapted for feeding on tissue fluids and blood.
- Gut: Strongyloides worms have a complete digestive system, consisting of an esophagus, intestine, and anus. They ingest host fluids and nutrients through their mouth and digest them within their gut.
- Reproductive system: Strongyloides stercoralis is a unique nematode because it has the ability to reproduce by both sexual and asexual means, resulting in a complex life cycle. Male worms possess a copulatory bursa, which is used to grasp the female during mating.
- Life cycle: The life cycle of Strongyloides involves both a free-living and parasitic stage. Infective larvae are passed in the feces of infected individuals or animals. These larvae can either develop into free-living adults or directly penetrate the host’s skin, initiating an autoinfection cycle. The larvae then migrate to the lungs, are coughed up, and swallowed, eventually reaching the small intestine where they mature into adult worms.
It’s important to note that the morphological characteristics may vary slightly between different species within the Strongyloides genus, but the general features mentioned above are characteristic of Strongyloides stercoralis, the most clinically significant species for humans.
Pathogenicity
Strongyloides stercoralis, the most common species of Strongyloides that infects humans, is considered a pathogenic parasite. The pathogenicity of Strongyloides is primarily related to its unique life cycle and the ability to cause both acute and chronic infections.
- Autoinfection: Strongyloides has the ability to complete its life cycle within a single host through a process called autoinfection. This means that the larvae produced by adult worms in the intestine can reinfect the same host by penetrating the intestinal wall or perianal skin. This autoinfection can lead to persistent, long-term infections, which can be a significant source of pathology.
- Hyperinfection: In individuals with weakened immune systems, such as those with HIV/AIDS, organ transplant recipients, or patients receiving immunosuppressive therapies, Strongyloides can undergo a phenomenon known as hyperinfection. This occurs when the normal checks on parasite reproduction are diminished, leading to an overwhelming increase in the parasite population. Hyperinfection can result in a massive dissemination of larvae throughout the body, affecting multiple organs and leading to severe symptoms and potentially fatal outcomes.
- Clinical manifestations: The symptoms and clinical manifestations of strongyloidiasis can vary widely depending on the intensity of infection, the immune status of the host, and the extent of larval migration. In mild cases, individuals may be asymptomatic or experience only mild gastrointestinal symptoms, such as abdominal pain, diarrhea, or bloating. In more severe cases, symptoms can include persistent or recurrent gastrointestinal symptoms, malabsorption, weight loss, anemia, cough, respiratory symptoms, and skin manifestations. Disseminated strongyloidiasis, seen in hyperinfection, can lead to severe sepsis, meningitis, pneumonia, and involvement of various organs, which can be life-threatening.
- Coinfections and complications: Strongyloides infections can also complicate the management of other diseases. For example, in individuals with coexisting helminthic infections or chronic medical conditions, strongyloidiasis can exacerbate the symptoms and complicate the clinical course. The presence of Strongyloides can also affect the immune response and alter the efficacy of certain medications, such as corticosteroids and immunosuppressive drugs, leading to increased susceptibility to other infections and treatment challenges.
Lab Diagnosis
The laboratory diagnosis of Strongyloides infection typically involves the detection of the parasite’s larvae or eggs in various clinical specimens. Several methods can be used for the diagnosis of Strongyloides, including:
- Stool Examination: The most common method is the examination of stool samples for the presence of Strongyloides larvae. Concentration techniques such as sedimentation or flotation may be employed to increase the sensitivity of the test. The larvae can be observed under a microscope, and their characteristic features, such as size and morphology, can aid in identification. However, it’s important to note that the larvae may not be present in every stool sample, especially in light or chronic infections.
- Serological Tests: Serological tests detect antibodies produced by the host in response to Strongyloides infection. Enzyme-linked immunosorbent assays (ELISAs) are commonly used to detect specific antibodies, such as IgG or IgG4, against Strongyloides antigens. Serological tests are particularly useful for diagnosing chronic or disseminated infections, as they can detect past or ongoing infections even when the larvae are not detectable in stool samples.
- Larval Culture: In certain cases, larvae can be directly cultured from stool samples or other clinical specimens, such as sputum or duodenal aspirates. The specimens are placed in a suitable culture medium, and the larvae can be observed as they develop and molt into infective stages. However, this method is time-consuming and requires expertise.
- Polymerase Chain Reaction (PCR): PCR-based methods can detect and amplify specific DNA sequences of Strongyloides in clinical samples. This technique can provide highly sensitive and specific results, even in cases with low parasite loads. PCR can be performed on stool samples or other clinical specimens, and it is particularly useful in cases where the larvae are difficult to detect microscopically.
It’s important to note that the timing and choice of diagnostic methods may vary depending on the clinical presentation, immune status of the patient, and the suspected stage of infection. In some cases, a combination of methods may be necessary to achieve an accurate diagnosis.
Treatment
The treatment of Strongyloides infection, known as strongyloidiasis, typically involves the use of anthelmintic medications to eliminate the parasite. The choice of treatment depends on factors such as the severity of infection, the immune status of the patient, and the presence of complications. Here are some commonly used medications for the treatment of strongyloidiasis:
- Ivermectin: Ivermectin is the drug of choice for the treatment of Strongyloides infection. It is highly effective against both the adult worms and the larvae. A single oral dose of ivermectin is usually sufficient for most uncomplicated cases. In some instances, multiple doses may be required, especially in cases of hyperinfection or disseminated disease.
- Albendazole: Albendazole is an alternative medication that can be used for the treatment of strongyloidiasis. It is less effective than ivermectin but can be considered as an alternative in situations where ivermectin is unavailable or contraindicated.
- Thiabendazole: Thiabendazole was previously a commonly used drug for the treatment of strongyloidiasis. However, it is associated with more side effects and a higher frequency of treatment failures compared to ivermectin. As a result, it is generally considered a second-line treatment option.
- Corticosteroids: In cases of hyperinfection or disseminated strongyloidiasis, where there is a significant immune response and potential for severe complications, the use of corticosteroids may be necessary. Corticosteroids can help suppress the immune response and reduce inflammation. However, they should only be used under close medical supervision due to the risk of exacerbating the infection.
It’s important to note that treatment for strongyloidiasis may need to be repeated or prolonged in cases of chronic or disseminated infection, as the parasite can persist and cause relapses. Additionally, individuals with hyperinfection or disseminated disease may require supportive care, such as fluid resuscitation, antibiotics for secondary infections, and close monitoring.
Prevention
Prevention of Strongyloides infection, also known as strongyloidiasis, involves measures to minimize exposure to the parasite and reduce the risk of infection. Here are some preventive measures:
- Proper sanitation and hygiene: Good personal hygiene practices are essential in preventing Strongyloides infection. This includes regular handwashing with soap and clean water, especially before handling food, after using the toilet, and after working in soil or areas with potential contamination.
- Avoidance of contaminated soil: Strongyloides larvae are commonly found in soil contaminated with human or animal feces. Avoid walking barefoot or sitting directly on the ground in areas where sanitation is poor or where the risk of contamination is high, such as in rural communities or areas with inadequate sanitation facilities.
- Safe disposal of feces: Proper disposal of human and animal feces is important in preventing the spread of Strongyloides infection. Encourage the use of sanitary latrines or toilets, and ensure that sewage systems or waste management practices are in place to prevent contamination of the environment.
- Screening and treatment of infected individuals: Identifying and treating individuals infected with Strongyloides can help prevent the spread of the parasite. In settings where strongyloidiasis is endemic or in high-risk populations, such as individuals with compromised immune systems or those who have recently immigrated from endemic areas, screening programs can be implemented to detect and treat infected individuals.
- Awareness and education: Raising awareness about strongyloidiasis and its transmission can help individuals take appropriate preventive measures. Health education programs should be developed and implemented to educate communities, healthcare providers, and individuals at risk about the importance of sanitation, hygiene, and proper disposal of feces.
- Occupational precautions: Individuals working in occupations that involve direct contact with soil, such as farmers, gardeners, and miners, should take precautions to minimize exposure to Strongyloides. This can include wearing protective clothing, such as gloves and boots, and practicing good hygiene measures after working in potentially contaminated environments.
Keynotes
Here are some key points to remember about Strongyloides infection (strongyloidiasis):
- Strongyloides is a parasitic nematode (roundworm) that can infect humans and various other animals.
- The most common species that infects humans is Strongyloides stercoralis.
- Strongyloides infection is commonly acquired by walking barefoot on soil contaminated with the parasite’s larvae or through direct contact with contaminated soil.
- The unique feature of Strongyloides is its ability to complete its life cycle within a single host through autoinfection, which can lead to long-term and persistent infections.
- The symptoms of strongyloidiasis can vary widely, ranging from mild gastrointestinal symptoms to more severe manifestations, especially in immunocompromised individuals.
- Severe forms of strongyloidiasis, such as hyperinfection or disseminated infection, can result in life-threatening complications and require prompt medical attention.
- Diagnosis of strongyloidiasis involves laboratory methods, including stool examination for larvae, serological tests, larval culture, and PCR-based techniques.
- The treatment of strongyloidiasis typically involves the use of anthelmintic medications, with ivermectin being the drug of choice. Albendazole and thiabendazole are alternative options.
- In cases of hyperinfection or disseminated infection, supportive care and the use of corticosteroids may be necessary.
- Prevention of strongyloidiasis involves practicing good personal hygiene, avoiding contact with contaminated soil, proper sanitation and waste management, screening and treatment of infected individuals, and raising awareness about the infection.
- Individuals at higher risk of Strongyloides infection include those with compromised immune systems, individuals living in or traveling to endemic areas, and occupations involving contact with soil.
- It’s important to consult with healthcare professionals or local health authorities for specific guidance on diagnosis, treatment, and prevention strategies based on the individual’s circumstances and geographical location.
Further Readings
- “Strongyloidiasis – The Most Neglected of the Neglected Tropical Diseases” – This article published in PLOS Neglected Tropical Diseases provides an overview of strongyloidiasis, including its epidemiology, clinical manifestations, diagnosis, treatment, and control strategies. [Link: https://journals.plos.org/plosntds/article?id=10.1371/journal.pntd.0000903]
- “Strongyloides stercoralis: A Plea for Action” – This review article published in The American Journal of Tropical Medicine and Hygiene discusses the global burden of strongyloidiasis, the challenges in its diagnosis and treatment, and the importance of increased awareness and intervention measures. [Link: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4350571/]
- “Strongyloidiasis: Risk Factors, Diagnosis, and Treatment” – This comprehensive review published in Infectious Disease Clinics of North America covers various aspects of strongyloidiasis, including the risk factors, clinical presentations, diagnostic methods, treatment options, and prevention strategies. [Link: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4011082/]
- “Strongyloides stercoralis: Global Distribution and Risk Factors” – This systematic review published in PLOS Neglected Tropical Diseases provides insights into the global distribution of Strongyloides infection and identifies risk factors associated with its transmission. [Link: https://journals.plos.org/plosntds/article?id=10.1371/journal.pntd.0002604]
- “Strongyloidiasis” – This chapter in the book “Tropical Infectious Diseases: Principles, Pathogens, and Practice” provides an in-depth overview of strongyloidiasis, including its biology, clinical features, diagnosis, treatment, and prevention. [Link: https://www.sciencedirect.com/science/article/pii/B9780702051012000425]
