Introduction
Table of Contents
Dental caries, commonly known as tooth decay or cavities, is a prevalent and multifactorial oral health condition that affects people of all ages worldwide. It is one of the most common chronic diseases, with significant implications for oral and overall health. Dental caries results from a complex interplay of factors, including bacteria, diet, genetics, and oral hygiene practices. In this introduction, we’ll explore the key aspects of dental caries:

1. Etiology: Dental caries is primarily caused by the interaction of specific bacteria in the oral cavity, mainly Streptococcus mutans and Lactobacillus species, with dietary sugars (particularly sucrose). These bacteria produce acids as they metabolize sugars, leading to demineralization of tooth enamel and subsequent cavity formation.
2. Pathogenesis: The process of dental caries development involves several stages:
- Demineralization: Acid-producing bacteria lower the pH in dental plaque, leading to the dissolution of mineralized tooth enamel.
- Cavity Formation: Over time, as demineralization progresses, it may result in the formation of cavities or holes in the affected tooth structure.
- Secondary Infections: If left untreated, caries can progress into deeper layers of the tooth, affecting the pulp, leading to pain, and potentially causing dental abscesses.
3. Risk Factors: Various risk factors contribute to the development of dental caries:
- Diet: High consumption of sugary and acidic foods and beverages increases the risk.
- Oral Hygiene: Inadequate brushing and flossing allow bacterial plaque to accumulate.
- Saliva: Saliva helps neutralize acids and remineralize enamel; reduced saliva flow can increase susceptibility.
- Fluoride: Insufficient exposure to fluoride, a natural mineral that strengthens enamel, can be a risk factor.
- Microbiome: The presence of cavity-causing bacteria in the oral microbiome plays a crucial role.
4. Clinical Presentation: Dental caries can manifest in various ways, including tooth sensitivity, pain, visible holes or pits on tooth surfaces, discoloration, and enamel erosion.
5. Prevention and Management: Preventive measures include maintaining good oral hygiene, reducing sugar consumption, and ensuring adequate fluoride exposure. Dental sealants and fluoride treatments can be applied to protect teeth. In advanced cases, restorative treatments like fillings, crowns, or root canals may be necessary.
6. Impact: Dental caries can have significant consequences, including pain, infection, tooth loss, impaired speech and eating, and reduced quality of life. It also has economic implications due to the cost of dental treatment.
7. Public Health: Dental caries remains a major public health concern, affecting millions of people globally. Efforts to promote oral hygiene, access to dental care, and community fluoridation programs aim to reduce its prevalence.
Types
Dental caries, commonly known as tooth decay or cavities, can manifest in several different types, each with distinct characteristics and locations on the teeth. The main types of dental caries are:
- Smooth-Surface Caries: These caries occur on the flat, smooth surfaces of the teeth, particularly the enamel. Smooth-surface caries are often associated with poor oral hygiene and a diet high in sugars. They typically progress slowly and may go unnoticed in their early stages.
- Pit and Fissure Caries: These caries develop in the deep grooves (fissures) and pits of the chewing surfaces of molars and premolars. These areas are more susceptible to decay because they can trap food particles and are difficult to clean effectively with a toothbrush. Pit and fissure caries can progress quickly due to their location.
- Root Caries: Root caries occur on the roots of teeth, typically in older individuals or those with gum recession. When the roots are exposed, they become vulnerable to decay because they lack the protective enamel covering found on the crowns of teeth. Root caries can be especially problematic for individuals with conditions like gum disease.
- Secondary Caries (Recurrent Caries): Secondary caries develop near existing dental restorations, such as fillings or crowns. These areas are at increased risk because they can create nooks and crannies where bacteria and food particles can accumulate, leading to further decay. Proper maintenance and regular dental check-ups are essential to monitor and address secondary caries.
- Smooth-Surface and Root Surface Rampant Caries: Rampant caries are extensive and rapidly progressing decay that affects multiple teeth throughout the mouth. They can occur due to systemic factors like compromised immunity, dry mouth (xerostomia), or excessive sugar consumption. Rampant caries require immediate attention and comprehensive treatment.
- Early Childhood Caries (Baby Bottle Tooth Decay): This type of caries affects infants and young children, often due to prolonged exposure to sugary liquids (e.g., milk, juice) in baby bottles or sippy cups. Early childhood caries can lead to severe tooth decay and damage primary (baby) teeth.
- Arrested Caries: Arrested caries refer to areas of tooth decay that have become inactive or “arrested” in their progression. This may occur due to changes in oral hygiene habits, dietary improvements, or remineralization treatments. Arrested caries often appear as dark, stained areas on the teeth and may require ongoing monitoring.
Signs and Symptoms
Dental caries, commonly known as tooth decay or cavities, can manifest with a variety of signs and symptoms. The specific signs and symptoms can vary depending on the severity and location of the decay. Here are the common signs and symptoms of dental caries:
- Tooth Sensitivity: Tooth sensitivity, especially to hot, cold, sweet, or acidic foods and beverages, is a common early sign of dental caries. Sensitivity may occur when the enamel is compromised, exposing the underlying dentin.
- Toothache: As the decay progresses and reaches the inner layers of the tooth, it can cause a persistent or intermittent toothache or discomfort. The pain may be mild to severe and can be aggravated by eating or drinking.
- Visible Holes or Pits: In advanced stages of dental caries, visible holes, pits, or dark spots may appear on the tooth’s surface. These physical changes are often a clear indicator of cavity formation.
- White Spots: Early-stage caries may present as chalky white spots on the tooth’s surface, indicating demineralization of the enamel. This is reversible if addressed promptly through remineralization and improved oral hygiene.
- Staining or Discoloration: Dental caries can cause staining or discoloration of the affected tooth. The tooth may turn brown, black, or even greenish in severe cases.
- Bad Breath (Halitosis): The presence of dental caries can lead to bad breath (halitosis) due to the release of foul-smelling gases by decay-causing bacteria.
- Visible Decay Around Fillings or Dental Restorations: Secondary or recurrent caries can develop around existing dental fillings, crowns, or other restorations. This can be observed during a dental examination.
- Pain When Biting or Chewing: Dental caries can cause discomfort or pain when biting or chewing, particularly if the decay has reached deeper layers of the tooth, such as the dentin or pulp.
- Swelling and Abscess: In advanced cases, untreated dental caries can lead to localized swelling, pus formation, and the development of a dental abscess. Abscesses can cause severe pain and require immediate dental attention.
- Tooth Mobility: Severe dental caries can weaken the tooth’s structure, leading to tooth mobility or a feeling of looseness.
Common Pathogens
Dental caries, commonly known as tooth decay or cavities, is primarily caused by specific bacteria that form dental plaque on the tooth surfaces. These bacteria metabolize dietary sugars and produce acids, leading to demineralization of tooth enamel and the development of carious lesions. The most common pathogens associated with dental caries include:
- Streptococcus mutans: It is one of the primary culprits in dental caries. It has a high affinity for attaching to tooth surfaces, where it forms biofilm (plaque). S. mutans metabolizes dietary sugars, producing lactic acid, which can lead to enamel demineralization and cavity formation.
- Streptococcus sobrinus: It is another acid-producing bacterium frequently found in dental plaque. It shares similar characteristics with S. mutans and contributes to the acidification of the oral environment.
- Lactobacillus species: Various species of Lactobacillus, such as Lactobacillus acidophilus and Lactobacillus fermentum, can thrive in the acidic conditions created by other cariogenic bacteria. They further contribute to the demineralization of tooth enamel.
- Actinomyces species: Some Actinomyces species, like Actinomyces viscosus and Actinomyces naeslundii, are common inhabitants of dental plaque. They play a role in biofilm formation and the acidogenic process that leads to caries.
- Streptococcus oralis: Streptococcus oralis is another oral bacterium that can contribute to the production of acids and demineralization when present in dental plaque.
- Streptococcus gordonii: Like S. oralis, Streptococcus gordonii is capable of adhering to tooth surfaces and participating in plaque formation.
- Streptococcus sanguinis: It is part of the normal oral flora and can be involved in the initial stages of plaque formation, facilitating the attachment of more cariogenic bacteria like S. mutans.
- Bifidobacterium species: Some species of Bifidobacterium have been associated with dental caries, particularly in children.
Laboratory Diagnosis
The laboratory diagnosis of dental caries primarily involves the examination of clinical samples and dental imaging to confirm the presence, extent, and severity of carious lesions. Here are the main laboratory diagnostic methods used in dentistry to diagnose dental caries:
- Clinical Examination:
- Dentists and dental hygienists visually inspect the teeth and probe them using dental instruments to assess the presence of cavities, soft spots, and discoloration.
- The International Caries Detection and Assessment System (ICDAS) is a standardized clinical scoring system used to evaluate the extent and severity of carious lesions.
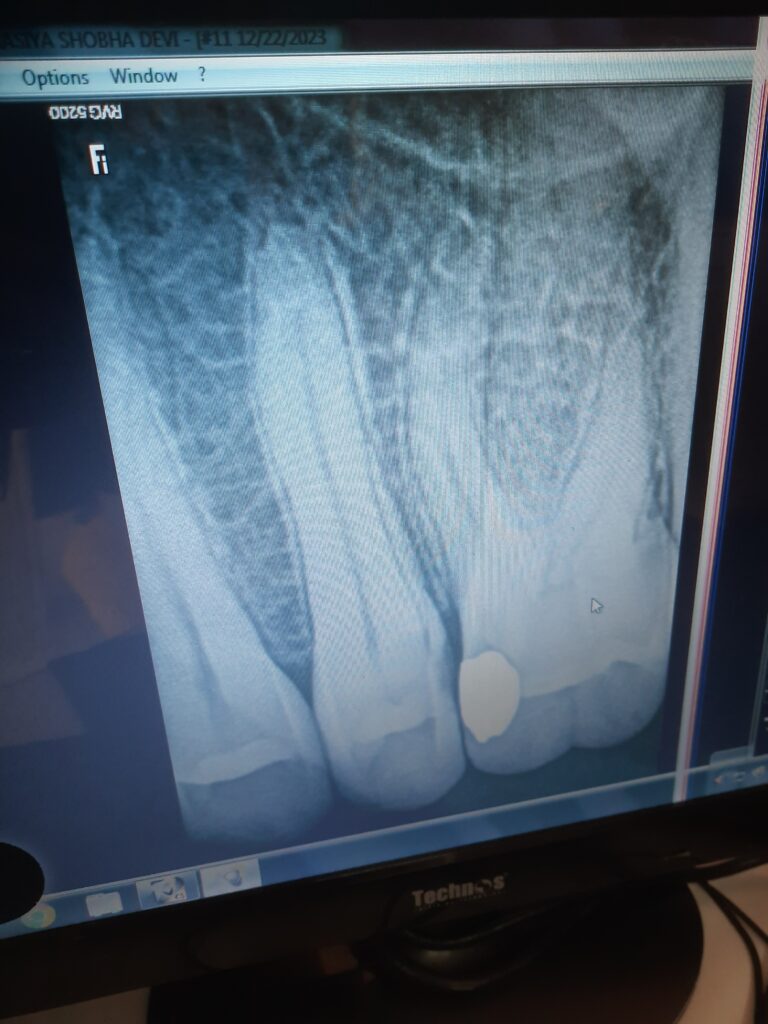
- Dental Radiography (X-Rays):
- Dental radiographs, such as bitewing and periapical X-rays, are commonly used to detect dental caries.
- X-rays can reveal carious lesions that are not visible to the naked eye, such as those between teeth and beneath the enamel surface.
- Fiber-Optic Transillumination (FOTI):
- FOTI involves shining a fiber-optic light source on the tooth to detect changes in light transmission. Carious lesions may appear darker or differently colored than healthy enamel.
- Digital Imaging:
- Digital imaging systems, including intraoral cameras, can capture high-resolution images of the teeth for diagnosis and monitoring of carious lesions.
- Quantitative Light-Induced Fluorescence (QLF):
- QLF is a technology that uses fluorescent light to detect early enamel demineralization, providing quantitative data on lesion severity and progression.
- Microbial Analysis:
- Microbiological testing can identify cariogenic bacteria (e.g., Streptococcus mutans) in dental plaque samples.
- Polymerase chain reaction (PCR) techniques can be employed for sensitive detection of specific caries-associated bacteria.
- Saliva Testing:
- The composition and flow rate of saliva can be assessed to evaluate its protective properties against dental caries.
- Low salivary flow rates and altered saliva composition can increase susceptibility to caries.
- Histological Examination:
- In cases where advanced caries necessitates tooth extraction or biopsy, histological analysis of tooth sections can confirm the extent and depth of decay.
- Laboratory Cultures (Rarely Used):
- Culturing cariogenic bacteria from dental plaque samples can be performed in research settings to study the microbial aspects of caries.
It’s important to note that the laboratory diagnosis of dental caries often complements clinical findings and aids in treatment planning. Early diagnosis and intervention can prevent the progression of carious lesions and help preserve tooth structure. Dentists and dental professionals use a combination of clinical assessment, dental imaging, and sometimes additional diagnostic tools to provide a comprehensive evaluation of a patient’s oral health and recommend appropriate treatment, such as dental fillings, crowns, or other restorative procedures.
Treatment
The treatment of dental caries, commonly known as tooth decay or cavities, varies depending on the extent and severity of the decay. The primary goal of treatment is to remove the decayed tissue, restore the affected tooth to its normal function and appearance, and prevent further progression of the disease. The following are common treatment options for dental caries:
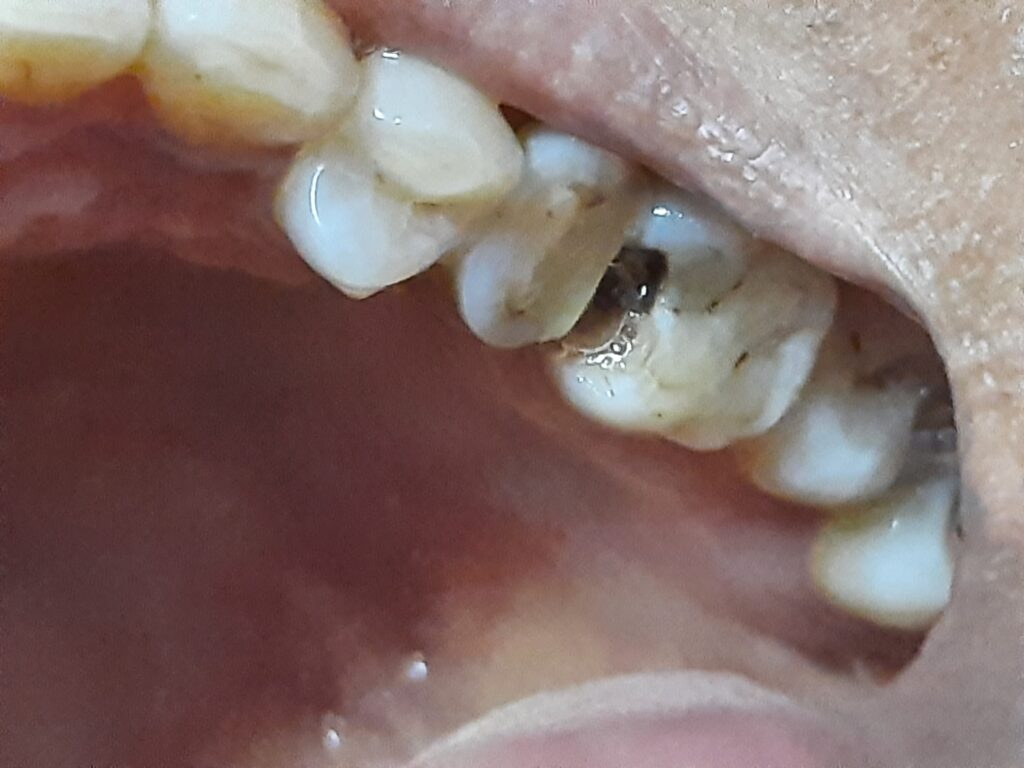
- Dental Fillings (Restorations):
- Dental fillings are the most common and conservative treatment for dental caries.
- The dentist removes the decayed tissue using a dental drill and then fills the resulting cavity with a restorative material, such as composite resin, amalgam, or glass ionomer cement.
- The choice of filling material depends on factors like the location of the cavity, the patient’s preference, and esthetic considerations.
- Dental Crowns (Caps):
- When the carious lesion is extensive, affecting a significant portion of the tooth or compromising its structural integrity, a dental crown may be recommended.
- The dentist removes the decayed tissue and shapes the tooth to accommodate the crown. The crown is then placed over the tooth to protect and strengthen it.
- Inlays and Onlays:
- In cases where the caries involves a large portion of the tooth but does not require a full crown, inlays and onlays may be used.
- Inlays are used to fill cavities within the tooth’s cusps (bumps), while onlays cover one or more cusps and are also known as partial crowns.
- Pulpotomy or Pulpal Therapy:
- When dental caries extends into the pulp (the innermost part of the tooth containing nerves and blood vessels), a pulpotomy or pulpal therapy may be necessary.
- In a pulpotomy, the infected pulp tissue is removed, and the remaining healthy pulp is treated and sealed. This procedure is often performed on primary (baby) teeth.
- Root Canal Treatment (Endodontic Therapy):
- In cases of advanced caries that have reached the dental pulp and caused infection or inflammation, root canal treatment may be required.
- During a root canal, the dentist removes the infected or damaged pulp, cleans and shapes the root canals, and seals them. The tooth is then restored with a crown.
- Tooth Extraction:
- In severe cases where the tooth is extensively decayed, fractured, or cannot be restored, extraction (removal) of the tooth may be necessary.
- After extraction, options for replacing the missing tooth include dental implants, bridges, and partial dentures.
- Preventive Measures:
- In addition to treating existing caries, preventive measures such as fluoride treatments, dental sealants, and improved oral hygiene practices are essential to prevent the development of new carious lesions.
The choice of treatment depends on various factors, including the location and severity of the caries, the patient’s age and oral health, and esthetic considerations. Early diagnosis and prompt treatment are crucial to prevent the progression of dental caries and preserve tooth structure. Regular dental check-ups and cleanings are also essential for early detection and prevention of caries.
Prevention and Control
Prevention and control of dental caries, commonly known as tooth decay or cavities, involve a combination of oral hygiene practices, dietary modifications, and professional dental care. Here are key strategies for preventing and controlling dental caries:
- Oral Hygiene Practices:
- Regular Brushing: Brush teeth at least twice a day, preferably in the morning and before bedtime, using fluoride toothpaste.
- Proper Brushing Technique: Use a soft-bristle toothbrush and brush all tooth surfaces, including the front, back, and chewing surfaces. Brush for at least two minutes.
- Flossing: Floss daily to remove plaque and food particles from between teeth and along the gumline.
- Use of Fluoridated Toothpaste: Fluoride helps strengthen tooth enamel and prevent demineralization. Use fluoride toothpaste appropriate for your age.
- Dietary Modifications:
- Limit Sugary and Acidic Foods: Reduce consumption of sugary and acidic foods and beverages, including candies, sodas, fruit juices, and sticky snacks.
- Snack Wisely: Choose tooth-friendly snacks like fruits, vegetables, nuts, and dairy products over sugary or starchy options.
- Avoid Frequent Snacking: Limit between-meal snacking to reduce exposure to sugars and acids.
- Fluoride Exposure:
- Fluoridated Water: If your community water supply is fluoridated, drink tap water to benefit from the protective effects of fluoride.
- Fluoride Supplements: In areas with low fluoride levels in the water, fluoride supplements may be recommended by a dentist or healthcare provider, especially for children.
- Fluoride Treatments: Dentists may apply fluoride varnishes or gels during dental check-ups to strengthen tooth enamel.
- Dental Sealants:
- Dental sealants are thin protective coatings applied to the chewing surfaces of molars and premolars.
- Sealants create a barrier that prevents food particles and bacteria from settling in the grooves of teeth, reducing the risk of cavities.
- Regular Dental Check-ups:
- Visit a dentist for regular check-ups and cleanings at least every six months or as recommended by your dental professional.
- Early detection of caries allows for prompt treatment and prevention of further damage.
- Saliva Flow and Composition:
- Maintain good oral hydration to support saliva production, as saliva helps neutralize acids and remineralize enamel.
- Some medications can cause dry mouth (xerostomia), so inform your healthcare provider or dentist if you experience this side effect.
- Behavioral and Lifestyle Modifications:
- Avoid tobacco products and limit alcohol consumption, as both can contribute to oral health problems, including an increased risk of dental caries.
- Education and Awareness:
- Educate yourself and your family about proper oral hygiene practices, healthy dietary choices, and the importance of regular dental care.
- Community Water Fluoridation:
- Support community water fluoridation efforts, as it is a cost-effective public health measure to reduce the prevalence of dental caries.
Keynotes
Here are keynotes summarizing important points about dental caries:
Dental Caries (Tooth Decay or Cavities) Keynotes:
- Definition: Dental caries is a common oral health condition characterized by the demineralization of tooth enamel, leading to the formation of cavities or holes in the teeth.
- Etiology: Dental caries primarily results from the interaction of specific bacteria, such as Streptococcus mutans and Lactobacillus species, with dietary sugars (particularly sucrose). These bacteria produce acids that erode tooth enamel.
- Pathogenesis: The process of dental caries development includes stages of demineralization, cavity formation, and potential pulp involvement if untreated.
- Risk Factors: Factors contributing to dental caries include poor oral hygiene, high sugar consumption, acidic foods and beverages, reduced saliva flow, and genetic susceptibility.
- Signs and Symptoms: Common signs and symptoms of dental caries include tooth sensitivity, pain, visible holes or pits in teeth, white spots, staining, bad breath, and pain while eating or drinking.
- Diagnosis: Diagnosis involves clinical examination, dental imaging (X-rays), and sometimes laboratory tests to assess the extent and severity of caries.
- Prevention: Prevention strategies include regular oral hygiene practices (brushing and flossing), limiting sugar intake, drinking fluoridated water, receiving fluoride treatments, applying dental sealants, and visiting the dentist for check-ups and cleanings.
- Treatment: Treatment options for dental caries depend on the extent of decay and may include dental fillings, crowns, root canals, or tooth extraction.
- Fluoride: Fluoride is a key preventive measure as it strengthens enamel, promotes remineralization, and inhibits acid production by cariogenic bacteria.
- Saliva: Saliva plays a protective role by neutralizing acids, helping with remineralization, and washing away food particles and bacteria.
- Community Efforts: Community water fluoridation, public health education, and access to dental care are crucial components of caries prevention efforts.
- Early Intervention: Early detection and treatment of dental caries are essential to prevent further damage and complications.
- Lifelong Commitment: Oral health practices should be maintained throughout life to prevent the development of new carious lesions and preserve dental health.
- Professional Care: Regular dental check-ups and professional cleanings are essential for monitoring oral health and receiving personalized guidance.
- Behavioral Factors: Lifestyle choices, such as avoiding tobacco and limiting alcohol consumption, can contribute to better oral health.
- Patient Education: Patient education and awareness are key in promoting oral hygiene, healthy dietary habits, and regular dental visits.
Further Readings
Textbooks:
- “Dentistry for the Child and Adolescent” by Ralph E. McDonald and David R. Avery – This comprehensive textbook covers various aspects of pediatric dentistry, including the prevention, diagnosis, and treatment of dental caries in children and adolescents.
- “Cariology” by Domenick T. Zero and Kim A. Hara – This textbook delves into the science of cariology, providing a detailed understanding of dental caries, its etiology, prevention, and treatment.
- “Sturdevant’s Art and Science of Operative Dentistry” by Andre V. Ritter, Harald O. Heymann, and William H. Sturdevant – This textbook focuses on operative dentistry techniques, including restorative procedures for dental caries.
Research Articles:
- “Dental Caries: A Dynamic Disease Process” – An article published in the Journal of Dentistry Research that discusses the dynamic nature of dental caries and its management.
- “Fluoride in Dental Public Health Programs” – A review article in the Journal of Dental Research that explores the role of fluoride in caries prevention.
- “Dental Caries: Diagnosis, Prevention, and Management” – An article in the Medical Clinics of North America that provides an overview of caries diagnosis, prevention strategies, and management options.
Websites and Organizations:
- American Dental Association (ADA) – The ADA website offers a wealth of resources on dental caries, including information on prevention, treatment, and oral health guidelines. Visit ADA
- American Academy of Pediatric Dentistry (AAPD) – The AAPD website provides guidelines and resources related to pediatric dentistry and the management of dental caries in children. Visit AAPD
- Centers for Disease Control and Prevention (CDC) – The CDC’s oral health section contains valuable information on dental caries epidemiology, prevention programs, and resources. Visit CDC Oral Health
- World Health Organization (WHO) – The WHO provides global insights into dental caries prevention and oral health initiatives. Visit WHO Oral Health
- Academy of General Dentistry (AGD) – The AGD offers articles and continuing education resources on various aspects of dental caries management. Visit AGD
