Introduction
Table of Contents
Enterococcus is a genus of Gram-positive bacteria that are part of the normal microbial flora of humans and animals. They are facultative anaerobes, meaning they can survive in both the presence and absence of oxygen. Enterococcus species are known for their ability to thrive in a wide range of environments, including the gastrointestinal tract, oral cavity, urinary tract, and soil.

They are often associated with healthcare-associated infections (HAIs) and community-acquired infections. Among the most clinically relevant species is Enterococcus faecalis, which is a leading cause of urinary tract infections, bloodstream infections, and surgical site infections. Another notable species is Enterococcus faecium, which has been increasingly associated with multidrug-resistant infections in healthcare settings.
These bacteria possess several virulence factors that contribute to their pathogenicity, including adhesins that aid in colonization, biofilm formation, and resistance to host immune defenses. Enterococcus species are known for their ability to acquire antibiotic resistance genes, making them a significant concern in healthcare settings.

Laboratory diagnosis of Enterococcus infections involves culturing and identifying the bacteria from clinical specimens. Molecular techniques, such as polymerase chain reaction (PCR), can be used to detect specific virulence genes and antibiotic resistance determinants.

Treatment of theses infections can be challenging due to the intrinsic and acquired resistance to multiple antibiotics. The choice of antibiotics depends on the susceptibility profile of the specific strain and the site of infection. In addition to antimicrobial therapy, prevention and control measures are essential in healthcare settings to limit the spread of Enterococcus infections, including strict adherence to infection control practices and antimicrobial stewardship programs.
Morphology
Enterococcus bacteria are Gram-positive cocci that typically appear as pairs or short chains under the microscope. Here are some key characteristics of Enterococcus morphology:
Shape: Their cells are spherical or ovoid in shape, resembling cocci. They are round or slightly elongated.
Arrangement: Their cells can be found in pairs (diplococci) or arranged in short chains. The cells divide in one plane, leading to the formation of characteristic pairs or chains.
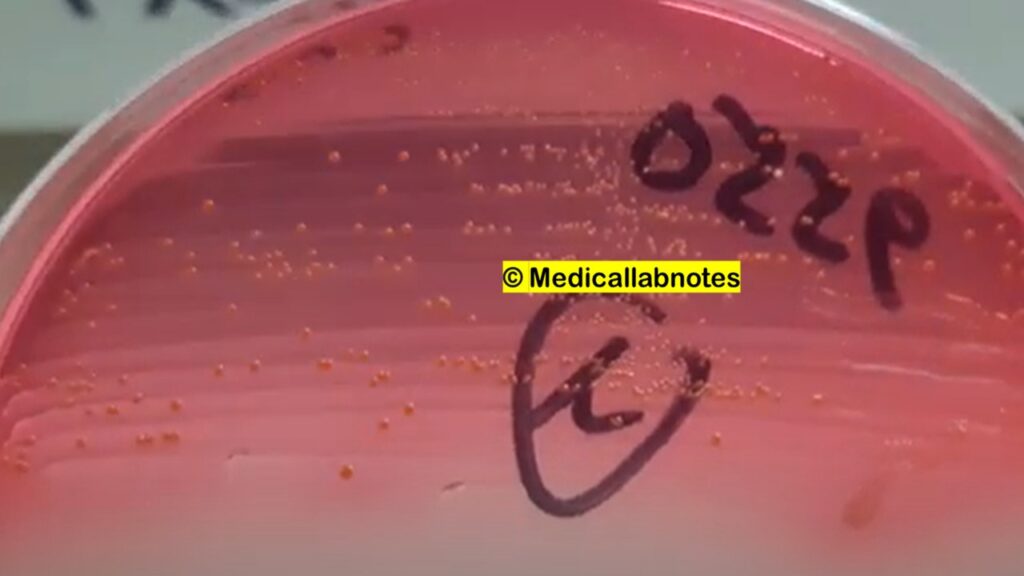
Size: Enterococcus cells are relatively small, with an average diameter ranging from 0.6 to 1.0 micrometers.

Cell Wall: These bacteria have a thick cell wall composed of peptidoglycan, which gives them their Gram-positive staining characteristic.
Capsule: Some Enterococcus species may produce a polysaccharide capsule, although it is not present in all strains.
Motility: Enterococcus species are non-motile, lacking flagella for movement.
Spore Formation: Enterococcus species do not form spores. Spore formation is a characteristic of some bacterial species but is not observed in Enterococcus.
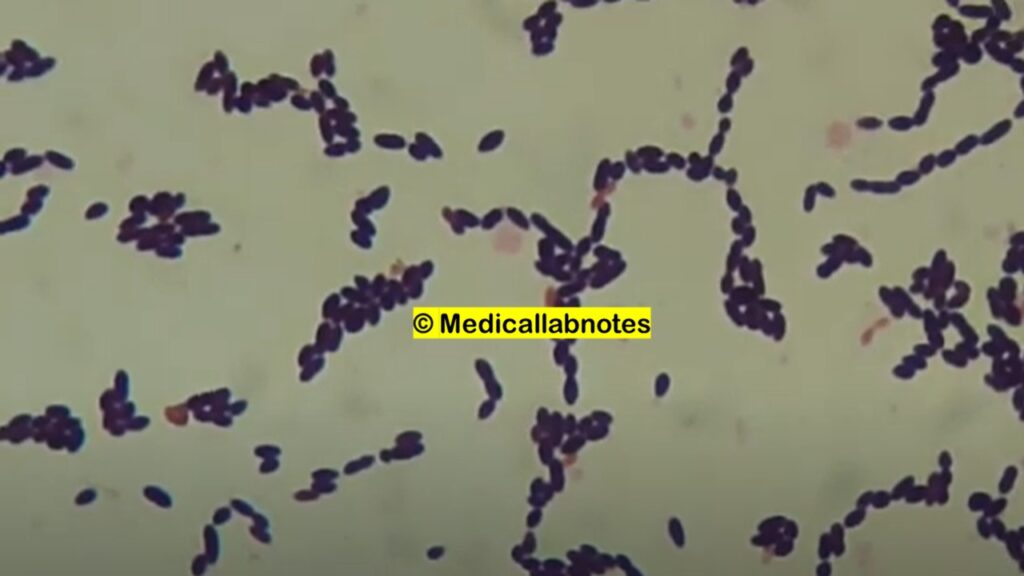
Staining: Their cells stain purple during the Gram staining procedure, indicating their Gram-positive nature.
Pathogenicity
Enterococcus species, particularly E. faecalis and E. faecium, can be both commensal organisms in the human gastrointestinal tract and opportunistic pathogens capable of causing a range of infections. While Enterococcus bacteria are generally considered less virulent compared to other pathogens, they possess certain virulence factors that contribute to their pathogenicity. Here are some key points about the pathogenicity of Enterococcus:
- Antibiotic Resistance: They are notorious for their ability to acquire and disseminate antibiotic resistance genes. They exhibit intrinsic resistance to many antibiotics and can develop resistance to even more through the acquisition of mobile genetic elements. This resistance can complicate the treatment of enterococcal infections, especially in healthcare settings.
- Biofilm Formation: Enterococci have the ability to form biofilms, which are communities of bacteria encased in a protective matrix. Biofilms enhance bacterial survival, resistance to host immune defenses, and resistance to antibiotics. Biofilms contribute to the persistence of Enterococcus infections and make them difficult to eradicate.
- Adherence and Colonization: They possess adhesins, surface proteins, and pili that allow them to adhere to host tissues and colonize various sites within the body. Adherence and colonization are crucial steps in the establishment of infections.
- Virulence Factors: Enterococci produce various virulence factors that aid in their pathogenicity. These include cytolysin, a pore-forming toxin that damages host cells; gelatinase, an enzyme that degrades extracellular matrix proteins; and aggregation substance, which promotes bacterial aggregation and facilitates horizontal gene transfer.
- Urinary Tract Infections (UTIs): E. faecalis is a leading cause of healthcare-associated and community-acquired UTIs. It can ascend from the urethra to the bladder, leading to cystitis, and can further progress to pyelonephritis in severe cases.
- Endocarditis: They are known to cause infective endocarditis, particularly in individuals with pre-existing heart valve abnormalities or prosthetic heart valves. The ability of Enterococcus to form biofilms on damaged heart valves contributes to the development of this serious infection.
- Bacteremia and Sepsis: Enterococcal bacteremia, the presence of Enterococcus bacteria in the bloodstream, can occur in immunocompromised individuals or those with invasive medical procedures. Bacteremia can progress to sepsis, a life-threatening condition characterized by a systemic inflammatory response.
- Surgical Site Infections: Enterococci are among the pathogens implicated in surgical site infections, particularly in abdominal, pelvic, and wound infections. They can contaminate surgical sites during invasive procedures and cause postoperative complications.
Lab Diagnosis
The laboratory diagnosis of Enterococcus infections involves the identification and characterization of the bacteria in clinical specimens. Here is an overview of the laboratory methods commonly used for the diagnosis:
- Microscopy: Gram staining is the initial step in the laboratory diagnosis of Enterococcus. EThey appear as Gram-positive cocci in pairs or short chains under the microscope.
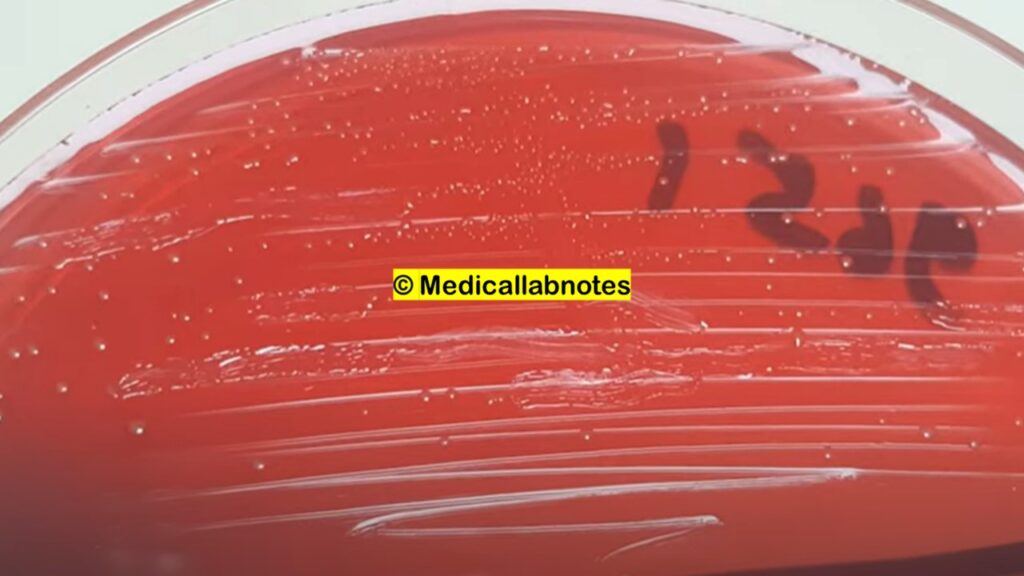
- Culture: They can be isolated from clinical specimens using various culture media, such as blood agar or selective media like bile esculin agar. The specimens commonly tested include urine, blood, wound swabs, and other relevant samples depending on the suspected site of infection.
- Biochemical Tests: Once the bacteria are isolated, biochemical tests are performed to confirm the identification of Enterococcus. These tests include catalase test (Enterococcus is catalase-negative), bile esculin hydrolysis (positive), and pyrrolidonyl arylamidase (PYR) test (positive for most Enterococcus species).

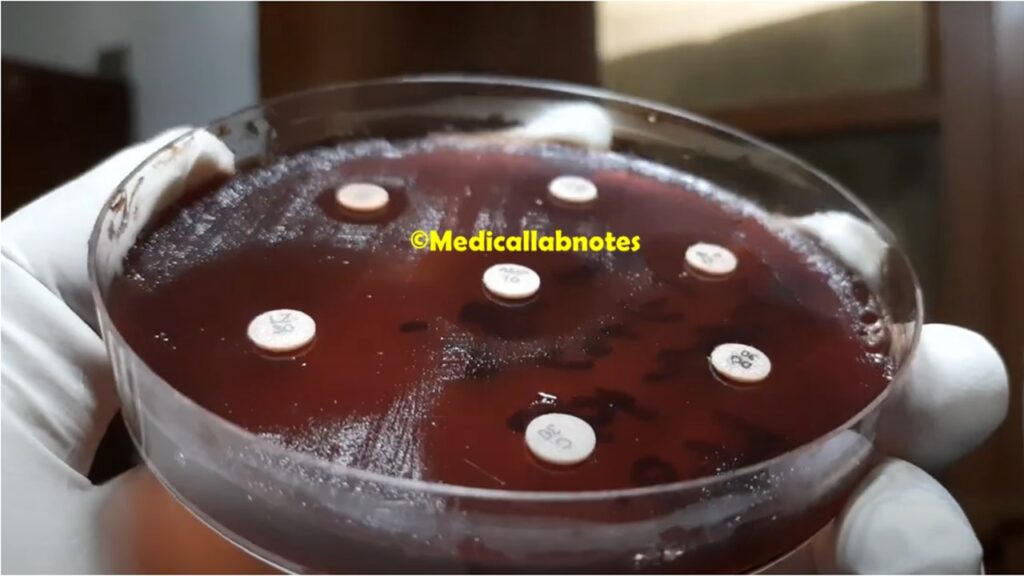
- Antimicrobial Susceptibility Testing: They are known for their resistance to multiple antibiotics. Antimicrobial susceptibility testing is crucial to determine the appropriate treatment options. The disk diffusion method or automated systems can be used to test the susceptibility of Enterococcus isolates to different antibiotics.

- Molecular Methods: Molecular techniques, such as polymerase chain reaction (PCR), can be employed to detect specific genes associated with Enterococcus species and their virulence factors. These tests can provide additional information about the strain’s genetic characteristics and potential antibiotic resistance genes.
- Serological Testing: Serological tests, such as enzyme immunoassays (EIAs) or latex agglutination tests, can be used to detect specific antibodies or antigens associated with Enterococcus infections. These tests may be helpful in diagnosing certain types of enterococcal infections, such as endocarditis.
Treatment
The treatment of Enterococcus infections can be challenging due to the intrinsic and acquired resistance of these bacteria to multiple antibiotics. The choice of treatment depends on several factors, including the site of infection, the severity of the infection, the identified species of Enterococcus, and the antimicrobial susceptibility pattern of the isolate. Here are some key points regarding the treatment of theses infections:
- Antibiotic Therapy: E. faecalis and E. faecium are the two most common species associated with clinical infections. Antibiotics commonly used to treat Enterococcus infections include:
- Ampicillin or amoxicillin: E. faecalis is usually susceptible to ampicillin or amoxicillin, either alone or in combination with an aminoglycoside antibiotic.Vancomycin: E. faecium is often resistant to ampicillin and amoxicillin. Vancomycin is the drug of choice for treating infections caused by vancomycin-susceptible E. faecium strains.Linezolid: Linezolid is an alternative antibiotic for treating vancomycin-resistant Enterococcus infections, including vancomycin-resistant Enterococcus faecium (VRE).Daptomycin: Daptomycin is another option for the treatment of Enterococcus infections, particularly in cases of endocarditis or complicated infections.
- Combination Therapy: In certain severe or complicated Enterococcus infections, combination therapy may be considered. This typically involves combining an aminoglycoside (such as gentamicin) with a cell wall-active agent (such as ampicillin or vancomycin). The synergistic effect of combination therapy can improve treatment outcomes.
- Surgical Intervention: In cases of Enterococcus infections involving prosthetic devices, such as heart valves or joint prostheses, surgical intervention may be necessary to remove or replace the infected device. This is often done in conjunction with antibiotic therapy.
- Antibiotic Resistance Considerations: They, particularly E. faecium, can exhibit high levels of antibiotic resistance, including resistance to vancomycin (VRE). In such cases, alternative treatment options, such as newer antibiotics or combination therapies, may be required.
Prevention
Preventing Enterococcus infections involves implementing a combination of infection control measures and promoting good hygiene practices. Here are some key strategies for the prevention of Enterococcus:
- Hand Hygiene: Proper hand hygiene is essential in preventing the transmission of Enterococcus. Regular and thorough handwashing with soap and water for at least 20 seconds, especially before and after handling food, using the restroom, and caring for individuals with known or suspected Enterococcus infections, is crucial.
- Infection Control in Healthcare Settings: In healthcare facilities, strict adherence to infection control protocols is necessary to prevent the spread of Enterococcus infections. This includes proper hand hygiene, the use of personal protective equipment (such as gloves and gowns), proper disinfection of surfaces and equipment, and implementing isolation precautions when necessary.
- Antimicrobial Stewardship: The appropriate and judicious use of antibiotics is crucial in preventing the emergence and spread of antibiotic-resistant Enterococcus strains. Healthcare professionals should follow antimicrobial stewardship guidelines, including selecting the right antibiotic, using the correct dosage and duration, and avoiding unnecessary or prolonged antibiotic therapy.
- Environmental Cleaning: Regular and thorough cleaning and disinfection of environmental surfaces in healthcare facilities and public settings can help reduce the transmission of Enterococcus. Proper disinfection techniques should be followed, paying attention to high-touch surfaces.
- Food Safety Practices: They can be present in food, particularly raw or undercooked meat, poultry, and unpasteurized dairy products. Practicing good food safety measures, such as proper food handling, cooking foods to recommended temperatures, avoiding cross-contamination, and ensuring the safety of water sources, can help prevent these infections through foodborne transmission.
- Safe Sex Practices: They can be transmitted through sexual contact. Practicing safe sex, including using condoms, can help reduce the risk of sexually transmitted Enterococcus infections.
- Prevention in High-Risk Individuals: Individuals with weakened immune systems, underlying medical conditions, or those who have undergone invasive procedures or surgeries are at higher risk of Enterococcus infections. Special precautions, such as strict adherence to infection control measures, may be necessary in these populations.
- Surveillance and Outbreak Response: Active surveillance of Enterococcus infections, particularly in healthcare settings, can help identify outbreaks and implement appropriate control measures promptly.
Keynotes
- Enterococcus is a genus of Gram-positive bacteria that are part of the normal flora of the human gastrointestinal tract and can also be found in various environmental sources.
- They, particularly E. faecalis and E. faecium, are the most clinically significant and commonly isolated species within the genus.
- They can cause a range of infections in humans, including urinary tract infections, bloodstream infections, wound infections, endocarditis, and intra-abdominal infections.

- They are known for their intrinsic and acquired resistance to many antibiotics, making them challenging to treat.
- They can develop resistance through various mechanisms, including the acquisition of resistance genes and the ability to form biofilms.
- In healthcare settings, They can contribute to nosocomial (hospital-acquired) infections, especially in individuals with compromised immune systems or those undergoing invasive procedures.
- They can also be transmitted through contaminated food, leading to foodborne infections.
- Proper infection control measures, including hand hygiene, appropriate use of antibiotics, environmental cleaning, and surveillance, are crucial in preventing the spread of Enterococcus infections.
- The selection of antibiotic therapy for Enterococcus infections should be guided by the specific species, antimicrobial susceptibility testing, and consideration of the site and severity of infection.
- Enterococcus infections can be associated with higher morbidity and mortality rates, particularly in immunocompromised individuals.
- Ongoing research is focused on understanding the mechanisms of antibiotic resistance in Enterococcus and developing new treatment strategies to combat these infections.
Further Readings
“Enterococcal Infections: Epidemiology, Microbiology, and Treatment” – Lam MMC, Seemann T, Bulach DM, et al. Clinical Microbiology Reviews, 2012.
- This comprehensive review provides an in-depth understanding of Enterococcus infections, including their epidemiology, microbiology, and treatment options.
“Enterococcal Infections: Host Response, Therapeutic, and Diagnostic Considerations” – Arias CA, Murray BE. Clinical Microbiology and Infection, 2012.
- The article covers the host response to Enterococcus infections, diagnostic approaches, and current therapeutic strategies, including the management of antibiotic resistance.
“Enterococci: From Commensals to Leading Causes of Drug Resistant Infection” – Sava IG, Heikens E, Huebner J. BMJ, 2010.
- This review article discusses the transition of Enterococcus from commensal bacteria to leading causes of drug-resistant infections, highlighting the challenges in their treatment and control.
“Enterococcus faecium Infections in Humans: Virulence Determinants, Clinical Presentation, and Treatment Options” – Lebreton F, Willems RJL, Gilmore MS. The Lancet Infectious Diseases, 2021.
- The article provides an overview of Enterococcus faecium infections in humans, including the virulence determinants, clinical manifestations, and available treatment options.
“Antimicrobial Resistance in Enterococcus spp.” – Higuita NIA, Huycke MM. Clinical Microbiology Newsletter, 2013.
- This article focuses on the mechanisms and patterns of antimicrobial resistance in Enterococcus species, discussing the implications for clinical management.
“Molecular Mechanisms of Antibiotic Resistance in Enterococcus spp.” – Arias CA, Murray BE. Microbiology Spectrum, 2012.
- The article explores the molecular mechanisms of antibiotic resistance in Enterococcus species, including the acquisition and dissemination of resistance genes.
