Introduction of Coagulation Test
Table of Contents
A coagulation test is a group of clinical laboratory tests pertaining to the coagulation profile that is performed to evaluate the blood’s ability to form clots. These tests are important for the diagnosis and management of bleeding disorders, as well as for monitoring patients who are receiving anticoagulant therapy.
The coagulation process involves a series of complex steps that result in the formation of a stable clot. The process begins when the blood vessel is injured, and platelets are activated to form a plug at the site of injury. This is followed by the activation of the coagulation cascade, which leads to the formation of fibrin, a protein that stabilizes the platelet plug and forms a clot.
There are several coagulation tests that are commonly used in clinical practice, including the prothrombin time (PT), activated partial thromboplastin time (aPTT), thrombin time (TT), and fibrinogen level. These tests can be performed using whole blood or plasma, and they provide important information about the different components of the coagulation process.
The interpretation of coagulation test results requires a thorough understanding of the normal coagulation process and the pathophysiology of bleeding disorders. Abnormal results can indicate a bleeding disorder, liver disease, vitamin K deficiency, or the presence of an anticoagulant drug. Proper interpretation of coagulation test results is essential for the diagnosis and management of patients with bleeding disorders.
List of Coagulation Tests
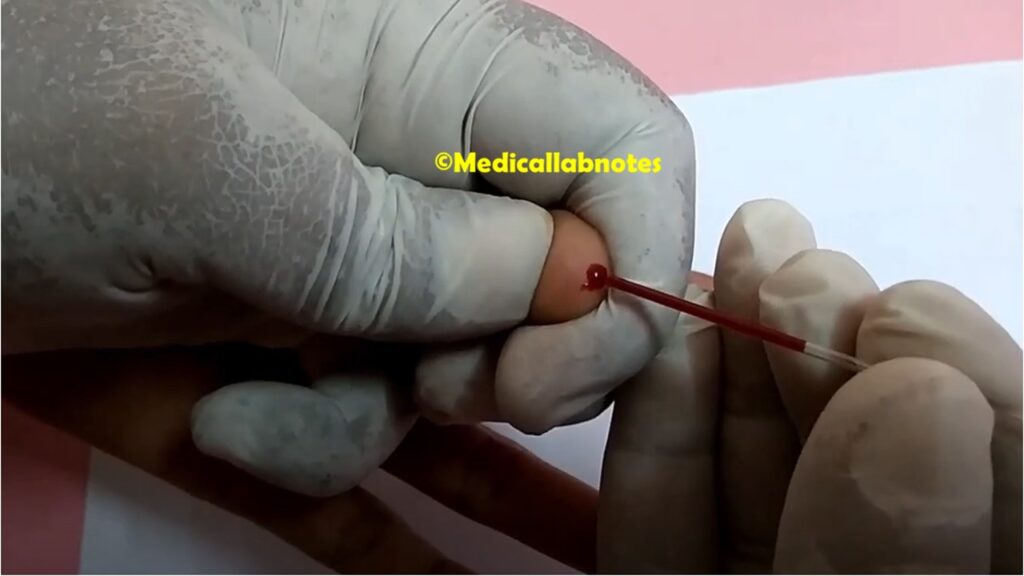
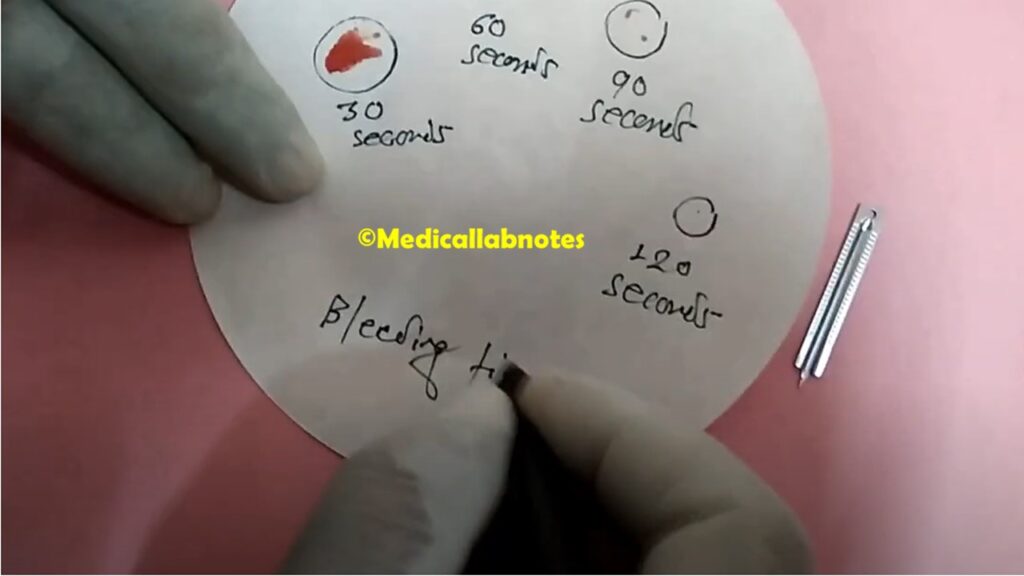
- Bleeding time-It is a type of coagulation test used to describe the amount of time it takes for bleeding to stop after a small cut or injury. It is a simple and non-invasive test that helps assess the function of platelets and blood vessels. During a bleeding time test, a healthcare provider will make a small incision in the skin, usually on the forearm, and measure the time it takes for the bleeding to stop. The test is usually performed with a standard lancet or a spring-loaded device called a Simplate. The normal range for bleeding time is typically between 2 to 9 minutes. However, the reference range may vary depending on the laboratory and the method used for the test. It is important to note that bleeding time is just one of several tests used to evaluate bleeding disorders, and the results should always be interpreted in conjunction with other clinical and laboratory findings.
- Clotting time-It is also known as coagulation time, which refers to the period of time that it takes for blood to form a clot. Blood clotting is an essential process that helps to prevent excessive bleeding and promote wound healing. When a blood vessel is damaged, the body initiates a complex series of reactions known as the coagulation cascade. This cascade involves the activation of various clotting factors, which ultimately leads to the formation of a blood clot. The clotting time can be affected by a variety of factors, such as medications, underlying medical conditions, and inherited clotting disorders. Blood clotting disorders can lead to either excessive bleeding or excessive clotting, both of which can be dangerous. To measure clotting time, a healthcare provider may perform a test known as prothrombin time (PT) or activated partial thromboplastin time (aPTT). These tests are commonly used to monitor the effectiveness of blood-thinning medications, such as warfarin or heparin, or to diagnose clotting disorders.

- Prothrombin time (PT)-It is a type of coagulation test of blood that measures the time it takes for blood to clot. It is often used to monitor the effectiveness of the anticoagulant medication, warfarin. Warfarin works by blocking the production of vitamin K-dependent clotting factors, including prothrombin. Prothrombin is a protein that is produced in the liver and is involved in the clotting process. When the level of prothrombin is low, the blood takes longer to clot. During the PT test, a small amount of blood is taken from a vein in the arm and mixed with a substance called a reagent, which initiates the clotting process. The time it takes for the blood to clot is then measured and compared to a standard reference range. The reference range varies depending on the laboratory and the specific reagent used. The results of the PT test are reported as the international normalized ratio (INR), which takes into account the variability in PT reference ranges between laboratories. The INR is used to adjust the dose of warfarin and maintain it within a therapeutic range.

- The fibrin degradation products (FDP) test is another type of coagulation test that measures the levels of fibrin degradation products in the blood. Fibrin degradation products are small protein fragments that are produced when the body breaks down blood clots. The test is usually ordered to help diagnose conditions related to excessive blood clotting or fibrinolysis (the breakdown of blood clots). The FDP test can help diagnose and monitor conditions such as disseminated intravascular coagulation (DIC), deep vein thrombosis (DVT), pulmonary embolism, and liver disease. Elevated levels of FDP in the blood can indicate that blood clots are being rapidly broken down in the body, which may be a sign of an underlying medical condition.
- Lupus Anti Coagulant, Panel-The Lupus Anticoagulant (LA) panel is a series of tests that are used to diagnose the presence of Lupus Anticoagulant antibodies in the blood. The Lupus Anticoagulant is a type of antibody that can cause excessive blood clotting, which can lead to the development of blood clots and other complications. The panel typically includes the following tests: Activated partial thromboplastin time (aPTT) – measures the time it takes for a blood clot to form. Dilute Russell viper venom time (dRVVT) – a more sensitive test that detects the presence of Lupus Anticoagulant antibodies. Prothrombin time (PT) – measures the time it takes for a blood clot to form using a different pathway than the aPTT. Mixing study – a test that is used to differentiate between the presence of Lupus Anticoagulant antibodies and other factors that may be causing the blood to clot. If the results of the panel show the presence of Lupus Anticoagulant antibodies, it may indicate that the patient has an increased risk of blood clots and may require further testing and treatment. It is important to note that the Lupus Anticoagulant panel is not used to diagnose Lupus itself, but rather to diagnose the presence of this specific type of antibody in the blood.
- Factor V, functional-Factor V, also known as proaccelerin, is a protein that plays an important role in blood clotting. It is a co-factor in the coagulation cascade, which is a complex series of reactions that ultimately leads to the formation of a blood clot. Factor V functions as a co-factor for factor Xa, which is an enzyme that converts prothrombin to thrombin. Thrombin then converts fibrinogen to fibrin, which is the main component of a blood clot. Factor V is synthesized in the liver and is found in the blood plasma. Its activity is regulated by other proteins in the coagulation cascade, including protein C and protein S. Mutations in the Factor V gene can lead to an increased risk of blood clots and a condition known as Factor V Leiden thrombophilia.
- Factor VII functional-Factor VII (FVII) is a protein that plays an important role in the coagulation cascade, which is the body’s process for forming blood clots to prevent excessive bleeding. FVII is produced in the liver and circulates in the bloodstream in an inactive form. The activation of FVII involves a series of enzymatic reactions that ultimately convert it to its active form, FVIIa. FVIIa then binds to tissue factor, a protein that is released by injured cells, to initiate the coagulation cascade. The functional assay for FVII measures the ability of FVIIa to activate factor X, which is another protein involved in the coagulation cascade. This assay is used to diagnose bleeding disorders and monitor patients receiving anticoagulant therapy. Low levels of FVII activity can lead to an increased risk of bleeding, while high levels can increase the risk of thrombosis (formation of blood clots).
- Factor VIII Functional-Factor VIII (FVIII) is an important protein involved in blood clotting. It is a co-factor for the activation of factor X, which is a critical step in the formation of blood clots. FVIII deficiency or dysfunction can lead to a bleeding disorder called hemophilia A. Factor VIII functional assay is a laboratory test used to measure the activity of FVIII in the blood. This test is used to diagnose and monitor hemophilia A and to determine the effectiveness of treatment with replacement therapy. In this assay, a sample of the patient’s blood is mixed with a reagent that activates the coagulation pathway. The time it takes for a blood clot to form is measured, and the activity of FVIII is calculated based on the clotting time. The results of the FVIII functional assay are reported as a percentage of normal FVIII activity. A normal FVIII level is between 50% and 150% of the activity found in healthy individuals. Hemophilia A patients typically have less than 5% FVIII activity and may require replacement therapy with FVIII concentrates to prevent bleeding episodes.
- D-dimer-It is a blood test that measures the level of a protein fragment called D-dimer in the blood. D-dimer is produced when blood clots are broken down and can be a sign of blood clotting in the body. The D-dimer test is most commonly used to help diagnose deep vein thrombosis (DVT) and pulmonary embolism (PE), which are both types of blood clots. It may also be used to help diagnose other conditions that involve blood clotting, such as disseminated intravascular coagulation (DIC) and stroke. A high level of D-dimer in the blood does not necessarily mean that a person has a blood clot, as D-dimer can be elevated in a number of other conditions such as pregnancy, recent surgery, and certain types of cancer. Therefore, the D-dimer test is usually used in combination with other tests and clinical evaluations to help diagnose blood clotting disorders. It’s important to note that the D-dimer test is not a screening test and is usually only performed if a person is suspected of having a blood clotting disorder. If you have any concerns about your risk of blood clots or the D-dimer test, you should speak to your doctor.
- Fibrinogen-It is a protein found in the blood that is essential for blood clotting and thus it is also a type of coagulation test. A fibrinogen test measures the level of fibrinogen in the blood, which is an indicator of the body’s ability to form a blood clot. The fibrinogen test is performed by taking a blood sample from a vein in the arm. The blood sample is then sent to a laboratory for analysis. The test can be done as part of a routine blood test or as part of a series of tests to diagnose a specific condition. The normal range for fibrinogen levels in the blood is between 200 and 400 milligrams per deciliter (mg/dL). Elevated levels of fibrinogen in the blood may be a sign of inflammation, infection, or tissue damage. Low levels of fibrinogen may indicate liver disease, kidney disease, or a genetic disorder. Fibrinogen tests are commonly used to diagnose and monitor certain conditions, such as deep vein thrombosis (DVT), pulmonary embolism, and disseminated intravascular coagulation (DIC). They may also be used to monitor the effectiveness of treatment for these conditions or to assess the risk of bleeding or clotting before surgery.
- Mean normal PT-The Prothrombin test, also known as the PT test, is a common coagulation test that measures the time it takes for your blood to clot. The results of the test are usually reported as the International Normalized Ratio (INR), which is a standardized way of reporting PT results. The mean normal PT refers to the average or normal range of results for the PT test. The mean normal PT can vary depending on the laboratory where the test is performed, but it is typically between 11 and 13 seconds. However, it’s important to note that the normal range can vary depending on factors such as age, sex, and medical history. When the PT test result is higher than the mean normal value, it may indicate a bleeding disorder or a problem with the blood clotting system. On the other hand, if the PT result is lower than the mean normal value, it may indicate a higher risk for blood clots. Your healthcare provider can help you interpret your PT test results and determine if any further testing or treatment is necessary.
- Factor IX functional-Factor IX is a protein that plays an important role in the blood clotting cascade. A deficiency in factor IX can lead to a bleeding disorder called hemophilia B. Factor IX functional assay is a laboratory test that measures the activity of factor IX in the blood. It is typically used to diagnose and monitor hemophilia B. During the test, a small amount of blood is drawn from the patient and mixed with a substance that initiates the clotting process. The time it takes for the blood to clot is measured, and the result is compared to a reference range to determine the patient’s factor IX activity level. A normal factor IX activity level is typically between 50% and 150%. Hemophilia B patients have factor IX activity levels below 50%. The severity of hemophilia B is classified based on the level of factor IX activity, with mild hemophilia B having activity levels between 5% and 40%, moderate hemophilia B having levels between 1% and 5%, and severe hemophilia B having activity levels below 1%. The results of the factor IX functional assay are used to guide treatment decisions, such as the dosing of factor IX replacement therapy.
- Factor V Leiden, Mutant Detection- Factor V Leiden is a genetic mutation that affects the function of a blood clotting protein called factor V. This mutation is associated with an increased risk of blood clots, which can lead to serious health problems such as deep vein thrombosis (DVT), pulmonary embolism, and stroke. Factor V Leiden mutation detection can be performed using a variety of methods, including DNA analysis techniques such as polymerase chain reaction (PCR), restriction fragment length polymorphism (RFLP), and DNA sequencing. These methods are used to identify specific changes in the DNA sequence of the factor V gene that is associated with the Factor V Leiden mutation. PCR is a widely used method for detecting the Factor V Leiden mutation. This technique involves amplifying a specific region of the DNA sequence using primers that are designed to bind to the mutated DNA sequence. After amplification, the DNA product is analyzed using gel electrophoresis or other methods to determine if the mutation is present. RFLP is another method that can be used to detect the Factor V Leiden mutation. This technique involves using enzymes that cut the DNA at specific locations based on the presence or absence of the mutation. The resulting DNA fragments are then analyzed to determine if the mutation is present. DNA sequencing is a more precise method for detecting the Factor V Leiden mutation. This technique involves determining the complete DNA sequence of the factor V gene and then comparing it to a reference sequence to identify any differences or mutations. Overall, these methods are highly accurate and reliable for detecting the Factor V Leiden mutation. They can be used for diagnostic testing, as well as for screening individuals who may be at risk for the mutation. If you have concerns about the possibility of having the Factor V Leiden mutation, it is best to speak with your healthcare provider, who can provide guidance on testing and management options. Von-Willebrand Factor Antigen-Von Willebrand Factor (vWF) is a large glycoprotein that is involved in the process of blood clotting. vWF is synthesized by endothelial cells and megakaryocytes and is released into the bloodstream. Its primary function is to mediate the adhesion of platelets to the site of injury in the blood vessels. vWF is measured in the blood by a laboratory test called Von-Willebrand Factor Antigen (vWF: Ag). This test measures the quantity of vWF in the blood and is used to diagnose and monitor conditions related to bleeding disorders such as von Willebrand disease (VWD), a genetic disorder that affects the ability of the blood to clot. The normal range for vWF: Ag in the blood is typically between 50% to 150% of the reference range. Levels below this range can indicate VWD or other bleeding disorders, while levels above this range may indicate a higher risk of blood clots. It is important to note that vWF: Ag levels can vary depending on age, sex, and other factors, and should be interpreted in conjunction with other clinical and laboratory findings.
- Protein C functional- Protein C is a vitamin K-dependent protein that plays an essential role in regulating blood coagulation. It is synthesized in the liver and circulates in the bloodstream as an inactive precursor protein. When activated, protein C functions as an anticoagulant by inhibiting the activity of factors V and VIII, which are important for blood clot formation. Protein C activation occurs through a process involving thrombin and thrombomodulin. Thrombin, a key enzyme in blood clotting, binds to thrombomodulin on the surface of endothelial cells lining blood vessels. This complex then activates protein C, which in turn cleaves and inactivates factors V and VIII, thereby reducing the risk of excessive blood clotting. In addition to its anticoagulant function, protein C also has anti-inflammatory properties and helps to maintain the integrity of the endothelium, the inner lining of blood vessels. A deficiency in protein C can lead to an increased risk of venous thromboembolism, a condition characterized by the formation of blood clots in the veins.
- Protein S functional- Protein S is a glycoprotein that plays an important role in the regulation of blood coagulation. It is synthesized in the liver and circulates in the blood in both free and bound forms. Protein S acts as a cofactor for activated protein C (APC), which cleaves and inactivates factors Va and VIIIa, key proteins in the blood coagulation cascade. By enhancing the activity of APC, protein S helps to prevent the formation of blood clots. In addition to its anticoagulant function, protein S has also been shown to have anti-inflammatory and cell-protective effects. It can bind to phosphatidylserine (PS), a phospholipid that is exposed on the surface of apoptotic cells, and thus play a role in the clearance of apoptotic cells by phagocytes. Protein S has also been implicated in the regulation of angiogenesis, cell proliferation, and cell migration. Protein S deficiency, which can be inherited or acquired, is associated with an increased risk of venous thrombosis and other thrombotic events. People with protein S deficiency may require anticoagulant therapy to prevent or treat blood clots.
- Anti Thrombin III functional- It is a protein that plays a crucial role in regulating blood clotting (coagulation) by inhibiting the activity of several clotting factors, including thrombin and factor Xa. The functional assay of anti-thrombin III measures the ability of this protein to inhibit the activity of clotting factors. This test is used to diagnose and monitor the treatment of conditions associated with abnormal blood clotting, such as deep vein thrombosis (DVT), pulmonary embolism (PE), and disseminated intravascular coagulation (DIC). The AT III functional assay involves measuring the time it takes for thrombin or factor Xa to clot a sample of plasma that has been pre-treated with a standardized amount of AT III. The clotting time is compared to the normal control, and the results are expressed as a percentage of normal activity. Low levels of AT III activity can increase the risk of developing blood clots, while high levels may indicate the presence of a clotting disorder or liver disease. The results of the AT III functional assay must be interpreted in conjunction with other laboratory tests and clinical findings.
- International Normalized Ratio (INR)-It is a standardized measure of blood clotting time. It is used to monitor the effectiveness of anticoagulant medications, such as warfarin, in people who are at risk of blood clots or have a history of cardiovascular disease. The INR is calculated by comparing the prothrombin time (PT) of a patient’s blood to a standardized reference value. The PT measures the time it takes for blood to clot in response to a clotting agent. The INR provides a more accurate and consistent measurement of blood clotting time across different laboratories and testing methods, which is important for ensuring that patients receive appropriate doses of anticoagulant medications. The target INR range for a patient depends on their individual medical history and condition but generally falls between 2.0 and 3.0 for most indications. Higher INR values indicate a longer clotting time and a higher risk of bleeding, while lower values indicate a shorter clotting time and a higher risk of blood clots.
- Activated partial thromboplastin time (APTT)- It is also a common coagulation test in Clinical Laboratories that measures the time it takes for blood to clot. APTT is used to monitor and evaluate the effectiveness of blood-thinning medications (anticoagulants) such as heparin and to diagnose bleeding disorders or clotting disorders. During the APTT test, a sample of the patient’s blood is collected and mixed with a substance that activates the clotting process. The time it takes for a clot to form is then measured. Normal APTT results may vary depending on the laboratory, but generally, it ranges from 25 to 35 seconds. If the APTT is prolonged, it may indicate a bleeding disorder, such as hemophilia, von Willebrand disease, or liver disease. Alternatively, a short APTT may suggest a clotting disorder, such as thrombophilia. It’s essential to interpret the results of the APTT test in the context of the patient’s clinical history and other laboratory tests.
- APTT Control-The APTT Control test is an important quality control measure that helps to ensure the accuracy and reliability of the APTT test. It is essential to perform this test regularly to maintain the quality of the laboratory’s testing procedures.
- Factor X-The Factor X test, also known as the FX assay or the coagulation Factor X assay, is a type of coagulation test in medical laboratories used to measure the level of Factor X in the blood. Factor X is a protein that plays a crucial role in the blood clotting process, and its deficiency or dysfunction can lead to bleeding disorders. The Factor X test is typically performed as part of a series of tests called a coagulation panel or coagulation profile. The test involves taking a small sample of blood from a vein in the arm and analyzing it in a laboratory. The results of the test are usually reported as a numerical value, expressed as a percentage of the normal level of Factor X in the blood. The Factor X test may be ordered if a person is suspected to have a bleeding disorder or if they are taking medications that affect blood clotting. Abnormal results may indicate a deficiency or dysfunction of Factor X, which can lead to excessive bleeding or an increased risk of blood clots. It is important to note that the Factor X test is just one component of a comprehensive evaluation of blood clotting and bleeding disorders. Other tests, such as a prothrombin time (PT) test, activated partial thromboplastin time (aPTT) test, and platelet count, may also be ordered to help diagnose and monitor these conditions.
- Factor XII-The Factor XII test is another coagulation test that measures the activity level of Factor XII, also known as the Hageman factor. Factor XII is a clotting factor in the blood that is involved in the initiation of the intrinsic pathway of blood coagulation. The test is performed to evaluate the risk of thrombosis or bleeding disorders. It can also be used to diagnose or monitor certain medical conditions, such as hereditary angioedema (HAE), a rare genetic disorder that causes swelling in various parts of the body. The test involves taking a blood sample from the patient and measuring the level of Factor XII activity. It is usually done in a laboratory setting and results are typically available within a few days. It is important to note that a low Factor XII activity level does not necessarily indicate a bleeding disorder, as many people with low levels do not experience abnormal bleeding. Likewise, a high Factor XII activity level does not always indicate a risk of thrombosis. Therefore, the interpretation of the test results should be done in conjunction with other clinical information and testing.
Keynotes on Coagulation Test
Coagulation tests are a group of laboratory tests that are used to evaluate the clotting ability of blood. These tests can help diagnose and monitor bleeding disorders, such as hemophilia and von Willebrand disease, as well as clotting disorders, such as deep vein thrombosis and pulmonary embolism. Here are some keynotes on the coagulation test:
- Prothrombin Time (PT) – measures the time it takes for blood to clot, and is often used to monitor warfarin therapy and assess liver function.
- International Normalized Ratio (INR) – a standardized version of the PT that allows for the comparison of results between different laboratories.
- Activated Partial Thromboplastin Time (aPTT) – measures the time it takes for blood to clot after a chemical is added to activate the clotting process, and is often used to monitor heparin therapy.
- Thrombin Time (TT) – measures the time it takes for fibrinogen (a protein necessary for clotting) to be converted to fibrin (the protein that forms the clot).
- D-dimer – a blood test that can help diagnose or rule out a blood clot, such as deep vein thrombosis or pulmonary embolism.
- Platelet count – measures the number of platelets in the blood, which are necessary for blood clotting.
It is important to note that interpretation of coagulation test results requires knowledge of a patient’s medical history, medications they are taking, and any underlying medical conditions they may have. Therefore, results should always be interpreted in consultation with a healthcare provider.
