Introduction
Table of Contents
- Taxonomy: Member of the Micrococcaceae family. Its nomenclature has evolved significantly; first described as Micrococcus in 1974, it was reclassified as Kocuria in 1995 and finally into the genus Rothia in 2018.
- Natural Habitat: Part of the normal flora of the skin, oropharynx, and upper respiratory tract. It is occasionally found in the gastrointestinal and vaginal microbiota.
Pathogenicity
While typically considered a low-grade commensal, it causes serious infections primarily in immunocompromised patients or those with indwelling medical devices.

- Clinical Manifestations: Commonly causes bacteremia (36.3% of cases) and infective endocarditis (13.7%). Other documented infections include septic arthritis, spinal osteomyelitis, peritonitis (especially in dialysis patients), and rare brain abscesses.

- Risk Factors: Vulnerable populations include oncology patients, transplant recipients, neonates, and individuals with central venous catheters.
- Invasive Potential: Recent cases demonstrate its ability to cause disseminated disease even in some immunocompetent individuals.

Lab Diagnosis
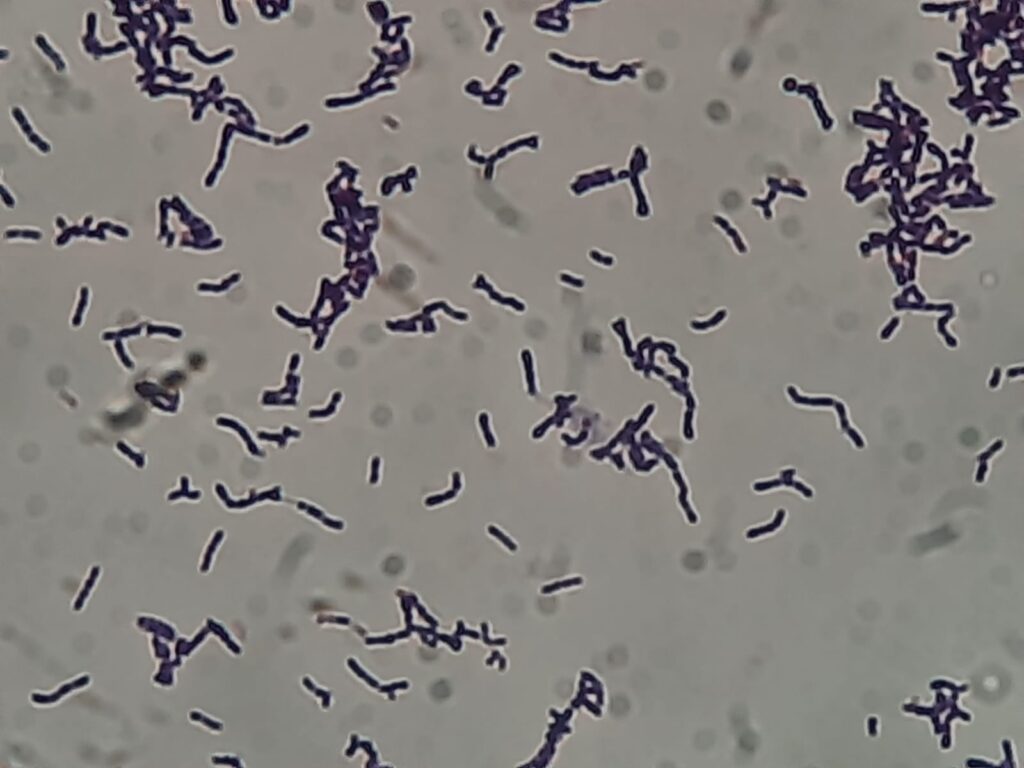
- Morphology: Gram-positive, non-motile, facultative anaerobic cocci. Under the microscope, they often appear as tetrads or irregular clusters, resembling Staphylococcus species.
- Culture: Grows on blood agar (BA) after 48 hours, forming pale cream to pale orange, dull, or matte convex colonies.
- Biochemical Profile: Catalase-positive, oxidase-negative, and coagulase-negative. It is susceptible to bacitracin and resistant to lysostaphin and lysozyme.
- Modern Identification: Because it is often misidentified as Coagulase-Negative Staphylococci (CoNS), labs use MALDI-TOF MS or automated systems like the Vitek 2 for faster, more accurate results. 16S rRNA sequencing remains the gold standard for definitive identification.
Treatment
There are no official clinical breakpoints, so treatment is often guided by expert consultation and raw Minimum Inhibitory Concentration (MIC) values.
- Antibiotics:
- First-line: Vancomycin is highly reliable and frequently used for serious infections.
- Other Effective Agents: Linezolid, rifampicin, teicoplanin, and certain beta-lactams, such as ampicillin/sulbactam or meropenem.
- Source Control: Crucial for success; removal of indwelling catheters is often necessary to resolve persistent bacteremia, as the organism has a high affinity for plastic surfaces.
Prevention
- Infection Control: Strict adherence to Central Line-Associated Bloodstream Infection (CLABSI) bundles, including proper hand hygiene and regular review of line necessity.
- Clinical Vigilance: Clinicians should not automatically dismiss R. kristinae as a “contaminant” when isolated from repeat sterile site cultures.
Keynotes
- Taxonomic History: Literature searches should include both Kocuria kristinae and Rothia kristinae to capture decades of relevant data.
- Clinical Pitfall: Its phenotypic similarity to Staphylococcus leads to frequent diagnostic under-recognition.
- Resistance: While many strains are susceptible to vancomycin, some reports have identified multidrug-resistant strains, making susceptibility testing essential.
Further Readings
- https://pmc.ncbi.nlm.nih.gov/articles/PMC11991707
- https://www.researchgate.net/publication/393909771_Unusual_Localization_of_Rothia_kristinae_Infection_First_Report_of_an_Intracerebral_Abscess_in_a_Pediatric_Patient
- https://www.researchgate.net/publication/393909771_Unusual_Localization_of_Rothia_kristinae_Infection_First_Report_of_an_Intracerebral_Abscess_in_a_Pediatric_Patient
- https://pmc.ncbi.nlm.nih.gov/articles/PMC7525060
- https://www.researchgate.net/publication/400257674_Disseminated_Rothia_kristinae_Infection_A_Case_Highlighting_an_Emerging_Pathogen
- https://www.gbif.org/species/165567773
- https://www.ovid.com/journals/idcpr/pdf/10.1097/ipc.0000000000001465~rothia-kristinae-nosocomial-sepsis-with-prolonged-bacteremia
- https://www.researchgate.net/publication/392885823_Rothia_kristinae_Nosocomial_Sepsis_With_Prolonged_Bacteremia_in_a_Critically_Ill_Extremely_Premature_Infant
- https://pmc.ncbi.nlm.nih.gov/articles/PMC4313135
- https://www.researchgate.net/publication/393909771_Unusual_Localization_of_Rothia_kristinae_Infection_First_Report_of_an_Intracerebral_Abscess_in_a_Pediatric_Patient
