Introduction
Table of Contents
Staphylococcus saprophyticus is a species of bacteria that belongs to the genus Staphylococcus. It is a Gram-positive, coagulase-negative, and facultative anaerobic bacterium. Like other staphylococci, S. saprophyticus typically appears in clusters under a microscope, which is characteristic of its name, derived from the Greek words “staphyle” (meaning a bunch of grapes) and “kokkos” (meaning berry).

This bacterium is part of the normal microbial flora in the human body and is commonly found in healthy individuals’ gastrointestinal tract, genitourinary system, and skin. However, it is most well-known as a common cause of urinary tract infections (UTIs) in young sexually active women. It is considered one of the leading causes of UTIs in sexually active females, accounting for approximately 10-20% of all community-acquired UTIs.
The infection typically occurs when the bacteria ascend the urethra and colonize the urinary bladder, leading to symptoms such as frequent and painful urination, cloudy or bloody urine, and lower abdominal discomfort. UTIs caused by S. saprophyticus are usually less severe than infections caused by other pathogenic bacteria, such as Escherichia coli.
Treatment of S. saprophyticus UTIs usually involves antibiotics that are effective against this specific bacterium. However, it is crucial to identify the causative agent and determine its antibiotic susceptibility to ensure appropriate treatment.
In summary, Staphylococcus saprophyticus is a significant bacterium associated with urinary tract infections in sexually active young women, and proper diagnosis and timely treatment are essential to manage infections caused by this microorganism. As with any medical condition, if you suspect you have a UTI or any other health issue, it’s essential to consult a healthcare professional for proper evaluation and treatment.
Morphology
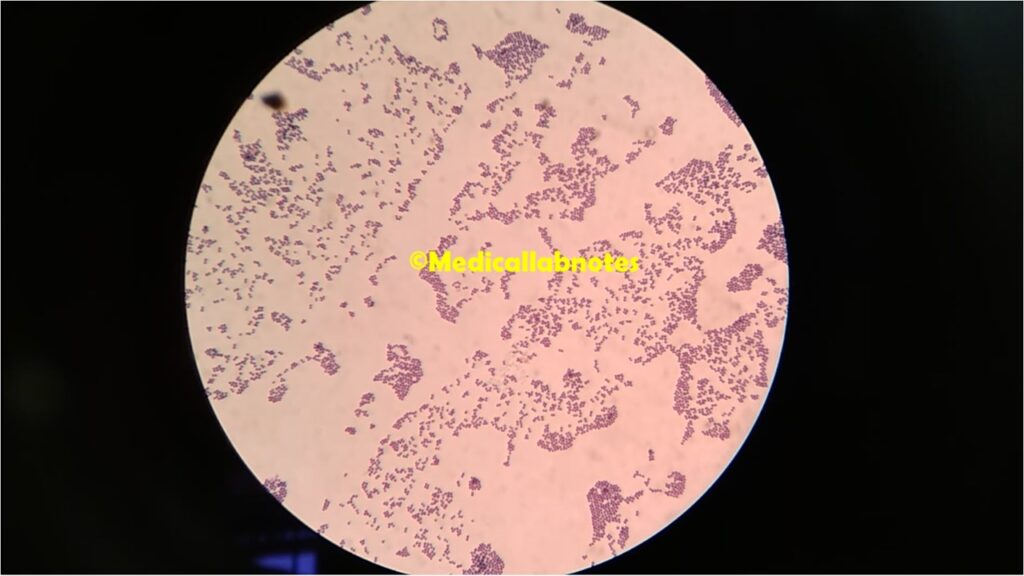
The morphology of Staphylococcus saprophyticus is characteristic of Gram-positive cocci, which means that under a microscope, the bacteria appear as round or spherical cells arranged in clusters. Here are some key features of the morphology of S. saprophyticus:

- Shape: S. saprophyticus cells are typically spherical or cocci-shaped, meaning they have a round appearance.
- Arrangement: The bacteria tend to form irregular clusters, resembling a bunch of grapes or clusters of berries. This clustering pattern is a distinguishing characteristic of staphylococci, and the genus name “Staphylococcus” is derived from the Greek words for “bunch of grapes.”
- Size: The average size of Staphylococcus saprophyticus cells ranges from 0.5 to 1.5 micrometers in diameter. However, individual cell sizes may vary within this range.
- Gram Staining: It is Gram-positive, which means it retains the crystal violet stain during the Gram staining procedure. The thick peptidoglycan layer in the cell wall of Gram-positive bacteria traps the crystal violet, causing them to appear purple under a microscope.
- Non-Motile: S. saprophyticus is a non-motile bacterium, meaning it lacks flagella and cannot move on its own.
- Catalase Test: Like other staphylococci, S. saprophyticus is catalase-positive. When exposed to hydrogen peroxide, the bacteria produce bubbles of oxygen gas, confirming their catalase activity.
Pathogenicity
Staphylococcus saprophyticus is primarily known for its pathogenicity, specifically as a common cause of urinary tract infections (UTIs) in young sexually active women. While it is a part of the normal microbial flora on the skin and mucous membranes of healthy individuals, it can become pathogenic under certain conditions. Here are some key points about the pathogenicity of Staphylococcus saprophyticus:
- Urinary Tract Infections (UTIs): Staphylococcus saprophyticus is a leading cause of community-acquired UTIs, particularly in sexually active women aged 15 to 30 years. The infection usually occurs when the bacteria ascend from the urethra to the urinary bladder. The close proximity of the urethra to the anus in females can facilitate the colonization of the urinary tract by bacteria during sexual activity or improper hygiene practices.
- Adhesion and Colonization: The ability of S. saprophyticus to adhere to the uroepithelial cells lining the urinary tract is a critical step in the development of UTIs. The bacteria possess specific adhesion factors that allow them to bind to host cells, facilitating colonization and subsequent infection.
- Virulence Factors: S. saprophyticus produces various virulence factors that aid in its ability to cause disease. Some of these factors include adhesins (proteins that help the bacteria stick to host cells), biofilm formation (enabling the bacteria to attach to surfaces and resist immune responses and antibiotics), and production of toxins and enzymes that can damage host tissues.
- Immune Evasion: Like other staphylococci, S. saprophyticus can evade the host immune response to some extent, allowing it to persist and cause infection in the urinary tract.
- Antibiotic Resistance: In recent years, some strains of S. saprophyticus have developed resistance to commonly used antibiotics, which can complicate treatment and contribute to recurrent or persistent infections.
It is important to note that while Staphylococcus saprophyticus is a significant cause of UTIs, it is generally less virulent and causes milder infections compared to other pathogenic bacteria, such as Staphylococcus aureus. Nevertheless, proper diagnosis and timely treatment with appropriate antibiotics are crucial to manage infections caused by this bacterium and prevent complications.
Lab Diagnosis
The laboratory diagnosis of Staphylococcus saprophyticus involves several steps to identify the bacterium accurately and differentiate it from other staphylococci and bacteria. The process typically includes the following techniques:

- Urine Sample Collection: The first step is to obtain a clean-catch midstream urine sample from the patient suspected of having a urinary tract infection. The sample should be collected in a sterile container to minimize the risk of contamination.
- Gram Staining: A small portion of the urine sample is placed on a microscope slide and subjected to Gram staining. Gram-positive cocci in clusters are observed, indicating the possible presence of staphylococci. The characteristic cluster arrangement can suggest the presence of Staphylococcus species.
- Culture: The urine sample is streaked onto appropriate agar plates, such as blood agar or MacConkey agar, and incubated at the appropriate temperature (usually 35-37°C) for 24-48 hours. Staphylococcus saprophyticus typically forms small, round, and opaque colonies on blood agar.
- Catalase Test: To differentiate S. saprophyticus from other Gram-positive cocci, such as Streptococcus species, a catalase test is performed. Staphylococcus species are catalase-positive, meaning they produce bubbles of oxygen gas when hydrogen peroxide is added to their colonies.
- Coagulase Test: It is coagulase-negative, which means it does not produce the enzyme coagulase. This test is crucial in differentiating it from Staphylococcus aureus, which is coagulase-positive.
- Novobiocin Susceptibility Test: S. saprophyticus is generally resistant to the antibiotic novobiocin. Therefore, a novobiocin susceptibility test is performed to help identify the bacterium. It involves applying novobiocin discs to the surface of the agar plate, and the zone of inhibition is measured to determine susceptibility.
- Biochemical Identification: Various biochemical tests, such as mannitol fermentation, urease production, and ornithine decarboxylase, can be performed to further confirm the identity of Staphylococcus saprophyticus.
- Antibiotic Susceptibility Testing: To guide appropriate treatment, antibiotic susceptibility testing is performed to determine which antibiotics are effective against the isolated strain of Staphylococcus saprophyticus.
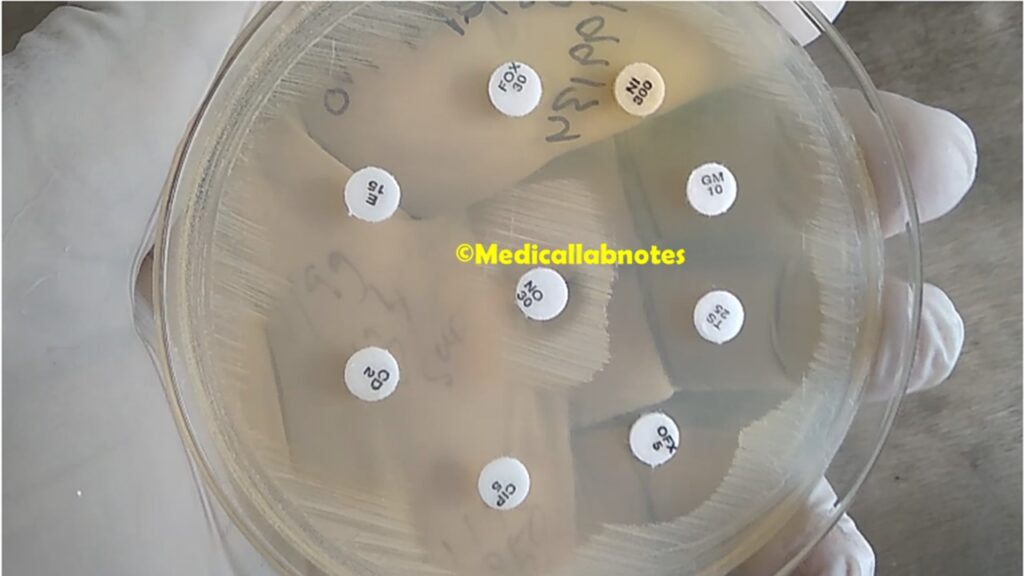
Treatment
The treatment of Staphylococcus saprophyticus infections, especially urinary tract infections (UTIs), involves antibiotic therapy. However, it is essential to consider antibiotic susceptibility testing results to ensure effective treatment, as some strains of S. saprophyticus may exhibit resistance to certain antibiotics. Here are the typical treatment options for S. saprophyticus infections:
- Antibiotics: The most common antibiotics used to treat uncomplicated urinary tract infections caused by Staphylococcus saprophyticus include:
- Trimethoprim-sulfamethoxazole (TMP-SMX)
- Nitrofurantoin
- Fluoroquinolones (such as ciprofloxacin or levofloxacin)
- Empiric Treatment: In some cases, when the urine sample is collected for culture and sensitivity testing, empiric antibiotic therapy may be initiated based on the most likely pathogens and their common susceptibility patterns. However, it is crucial to reassess the treatment once the culture results become available to ensure appropriate coverage if the isolated strain of S. saprophyticus is resistant to the initial choice of antibiotics.
- Duration of Treatment: The duration of antibiotic treatment depends on the severity of the infection and the specific antibiotic used. In most uncomplicated UTIs, a short course of 3 to 7 days is sufficient. For more complicated infections or if the patient has underlying health issues, the treatment duration may be extended.
- Follow-up: Patients need to complete the full course of antibiotics as prescribed by their healthcare provider, even if they start feeling better before finishing the medication. Failure to complete the treatment could lead to recurrent infections or antibiotic resistance.
- Antibiotic Resistance: As with any bacterial infection, antibiotic resistance is a concern. If the isolated strain of S. saprophyticus is resistant to the initial antibiotics, the healthcare provider may need to adjust the treatment regimen based on the sensitivity results.
- Supportive Measures: In addition to antibiotic therapy, patients are encouraged to drink plenty of fluids to help flush out the bacteria from the urinary tract. Additionally, pain relievers may be recommended to alleviate discomfort or pain associated with the UTI.
Prevention
Preventing S. saprophyticus infections, particularly urinary tract infections (UTIs), involves adopting certain hygiene and lifestyle practices to reduce the risk of bacterial colonization and infection. Here are some preventive measures:
- Hygiene Practices:
- Practice good hand hygiene by washing hands with soap and water regularly, especially before eating and after using the restroom.
- Use proper wiping techniques after using the restroom (front to back for females) to prevent the transfer of bacteria from the anal area to the urinary tract.
- Urination and Hydration:
- Urinate regularly and promptly when you feel the need to empty your bladder. Holding urine for an extended period may increase the risk of bacterial growth in the urinary tract.
- Drink plenty of fluids to maintain adequate urine output, which helps flush out bacteria from the urinary system.
- Sexual Activity:
- Practice safe sex by using condoms to reduce the risk of sexually transmitted infections, which can increase the risk of UTIs.
- Urinate before and after sexual intercourse to help clear any bacteria that might have entered the urethra during activity.
- Avoid Irritants:
- Avoid using potentially irritating products in the genital area, such as strong soaps, douches, or scented hygiene products.
- Wear breathable and comfortable underwear, and avoid tight-fitting clothing that may trap moisture and create a favorable environment for bacterial growth.
- Antibiotic Prophylaxis:
- In some cases, healthcare providers may prescribe low-dose antibiotics for individuals prone to recurrent UTIs caused by Staphylococcus saprophyticus.
- Maintain a Healthy Immune System:
- A strong immune system helps the body fight off infections more effectively. Maintain a healthy lifestyle with a balanced diet, regular exercise, adequate sleep, and stress management.
- Avoid Catheter Use:
- If possible, avoid using urinary catheters, as they increase the risk of UTIs.
- Regular Health Check-ups:
- Regularly visit your healthcare provider for routine check-ups and discuss any symptoms or concerns related to urinary health.
Keynotes
Staphylococcus saprophyticus is a Gram-positive, coagulase-negative bacterium that is a common cause of urinary tract infections (UTIs), especially in sexually active young women. Here are some keynotes on S. saprophyticus:
- UTI Pathogen: Staphylococcus saprophyticus is a significant cause of community-acquired urinary tract infections, particularly in young sexually active women. It accounts for approximately 10-20% of all community-acquired UTIs.
- Gram-Positive Cocci: Under the microscope, S. saprophyticus appears as Gram-positive cocci, arranged in characteristic grape-like clusters.
- Coagulase-Negative: S. saprophyticus is coagulase-negative, which helps differentiate it from more pathogenic Staphylococcus species like Staphylococcus aureus.
- Pathogenicity: Although part of the normal microbial flora, S. saprophyticus can cause disease under certain conditions, particularly when it ascends the urethra and colonizes the urinary bladder, leading to UTIs.
- UTI Symptoms: UTIs caused by Staphylococcus saprophyticus typically present with symptoms such as frequent and painful urination, cloudy or bloody urine, and lower abdominal discomfort.
- Adhesion Factors: The bacterium possesses adhesins that aid in binding to the uroepithelial cells of the urinary tract, facilitating colonization and infection.
- Antibiotic Susceptibility: Treatment of Staphylococcus saprophyticus infections involves antibiotics such as trimethoprim-sulfamethoxazole (TMP-SMX), nitrofurantoin, and fluoroquinolones. However, antibiotic resistance may be a concern, and susceptibility testing is crucial to guide appropriate treatment.
- Prevention: Preventive measures include practicing good hygiene, staying well-hydrated, maintaining regular urination habits, practicing safe sex, and avoiding irritants in the genital area.
- Lower Virulence: Staphylococcus saprophyticus is generally considered less virulent than other pathogenic Staphylococcus species, leading to milder UTI symptoms.
- Empiric Treatment: In the case of suspected UTIs, empiric antibiotic therapy may be initiated based on common pathogens and their susceptibilities while awaiting culture results.
- Diagnostic Tests: Laboratory diagnosis involves Gram staining, culture, catalase testing, coagulase testing, and biochemical identification to differentiate S. saprophyticus from other bacteria.
Further Readings
- Stapleton AE. Staphylococcus saprophyticus: a common cause of urinary tract infection in women. Urol Clin North Am. 1999;26(4):691-701.
- Flores-Mireles AL, Walker JN, Caparon M, Hultgren SJ. Urinary tract infections: epidemiology, mechanisms of infection and treatment options. Nat Rev Microbiol. 2015;13(5):269-284.
- Ryan KJ, Ray CG (editors). Sherris Medical Microbiology. 6th edition. McGraw-Hill Medical, 2014. (Chapter 21: Staphylococci).
- Murray PR, Rosenthal KS, Pfaller MA (editors). Medical Microbiology. 8th edition. Elsevier, 2015. (Chapter 22: Staphylococci).
- Centers for Disease Control and Prevention (CDC): The CDC website contains information on bacterial infections, including Staphylococcus species, their characteristics, and treatment options. Website: https://www.cdc.gov/
- World Health Organization (WHO): The WHO provides global health information and resources, which may include data on bacterial infections and antibiotic resistance. Website: https://www.who.int/
- National Institutes of Health (NIH): The NIH offers a wealth of research articles and publications on various topics, including infectious diseases and microbiology. Website: https://www.nih.gov/

I have recently started a site, the info you offer on this website has helped me tremendously. Thanks for all of your time & work.