Introduction
Table of Contents
Citrobacter farmeri is a Gram-negative, facultative anaerobic, rod-shaped bacterium. It belongs to the Enterobacteriaceae family, which also includes other well-known genera like Escherichia, Salmonella, and Klebsiella. The genus “Citrobacter” was named for its ability to utilize citrate as its sole carbon source.
Here’s a brief overview:
- Ecology and Habitat: Citrobacter species, including C. farmeri, can be found in various environments including soil, water, and the intestines of animals and humans. They’re part of the normal gut flora in some individuals but can also act as opportunistic pathogens.
- Clinical Significance: While not the most common cause of infections, Citrobacter species can cause a range of diseases, particularly in immunocompromised individuals. They have been associated with urinary tract infections, respiratory tract infections, septicemia, meningitis (especially in neonates), and other infections.
- Antibiotic Resistance: Like many other Enterobacteriaceae, certain strains of Citrobacter can acquire resistance to commonly used antibiotics. This resistance can be due to various mechanisms such as beta-lactamase production, efflux pumps, or alterations in target sites.
- Identification: In a laboratory setting, Citrobacter species can be differentiated from other Enterobacteriaceae by their ability to utilize citrate and produce a characteristic metabolic and biochemical profile on various test substrates.
- Treatment: Treatment of Citrobacter infections involves antibiotics, but the choice of antibiotic depends on the sensitivity pattern of the isolated strain. It’s always essential to perform susceptibility testing to guide appropriate therapy.
Morphology
Citrobacter farmeri shares the general morphological characteristics of many members of the Enterobacteriaceae family. Here’s a description of its morphology:
- Cell Shape: It is a rod-shaped bacterium, also described as bacilli.
- Gram Staining: It is Gram-negative, meaning that it doesn’t retain the violet crystal stain used in Gram staining but instead takes up the counterstain, which gives it a pink or red appearance under a microscope.
- Flagella: Citrobacter farmeri is motile, and this motility is often due to the presence of peritrichous flagella. “Peritrichous” means that the flagella are distributed all over the surface of the bacterium.
- Size: While the size can vary somewhat depending on the growth conditions and specific strain, a typical size for rod-shaped bacteria like Citrobacter is about 1-5 micrometers in length and about 0.5-1.0 micrometers in diameter.
- Capsule: Some strains can produce a capsule, which is a viscous layer outside the cell wall. The presence of a capsule can confer certain advantages to bacteria, such as resistance to phagocytosis by immune cells.
- Colonial Morphology: When grown on solid media, such as an agar plate, Citrobacter farmeri colonies are usually smooth, moist, and opaque with a shiny surface. The color of the colonies can vary depending on the type of media used.
Pathogenicity
Citrobacter farmeri, like other species within the Citrobacter genus, can be an opportunistic pathogen, meaning it can cause infections primarily in individuals with weakened immune systems or other predisposing factors.
Here are some points concerning the pathogenicity of Citrobacter farmeri:
Infections in Humans
Citrobacter farmeri can cause a range of infections, including but not limited to:
- Urinary tract infections (UTIs)
- Respiratory tract infections
- Bloodstream infections or septicemia
- Meningitis: Citrobacter species, particularly Citrobacter koseri (formerly known as Citrobacter diversus), have been notably associated with neonatal meningitis and the development of brain abscesses. While C. farmeri is less frequently implicated than C. koseri, it still poses a risk.
- Intra-abdominal infections
- Wound infections
Virulence Factors
While specific virulence factors can vary between strains, some associated with Citrobacter infections include:
- Capsules, which can protect the bacterium from phagocytosis by the host’s immune cells.
- Endotoxin (lipopolysaccharide or LPS) found in the outer membrane of Gram-negative bacteria, which can trigger inflammation and other immune responses.
- Ability to form biofilms, which can enhance resistance to antibiotics and the host’s immune response.
- Some strains may produce toxins or enzymes that can damage host tissues.
Risk Groups
While Citrobacter can colonize the intestines of healthy individuals without causing disease, certain populations are at a higher risk for infection, including:
- Neonates
- The elderly
- Immunocompromised individuals, such as those with HIV/AIDS, transplant recipients, or those undergoing chemotherapy.
- Individuals with underlying medical conditions like diabetes or chronic kidney disease.
Antibiotic Resistance
- Over time, some strains of Citrobacter farmeri have acquired resistance to commonly used antibiotics, which can complicate treatment and lead to more prolonged infections. It’s essential to perform antibiotic susceptibility testing to guide therapy when dealing with infections caused by this organism.
- Transmission: It can be transmitted via the fecal-oral route, especially in hospital settings, or through contaminated food and water. Proper hand hygiene and infection control measures are crucial to prevent the spread of Citrobacter infections, especially in healthcare environments.
Lab Diagnosis
Laboratory diagnosis of Citrobacter farmeri, like many other bacterial pathogens, involves both direct and indirect methods. Here’s an overview of the procedures commonly used for its detection and identification:
Specimen Collection
Depending on the suspected site of infection, appropriate specimens are collected. This might include urine (for UTIs), cerebrospinal fluid (for meningitis), blood (for septicemia), sputum (for respiratory infections), or wound swabs.
Direct Examination
- Gram Staining: This is a preliminary test. Citrobacter farmeri, being a Gram-negative bacterium, will appear as pink or red rods under the microscope.
- Microscopy: Presence of bacilli in samples, especially in cases like meningitis, can provide immediate but non-specific evidence of bacterial infection.

Culture
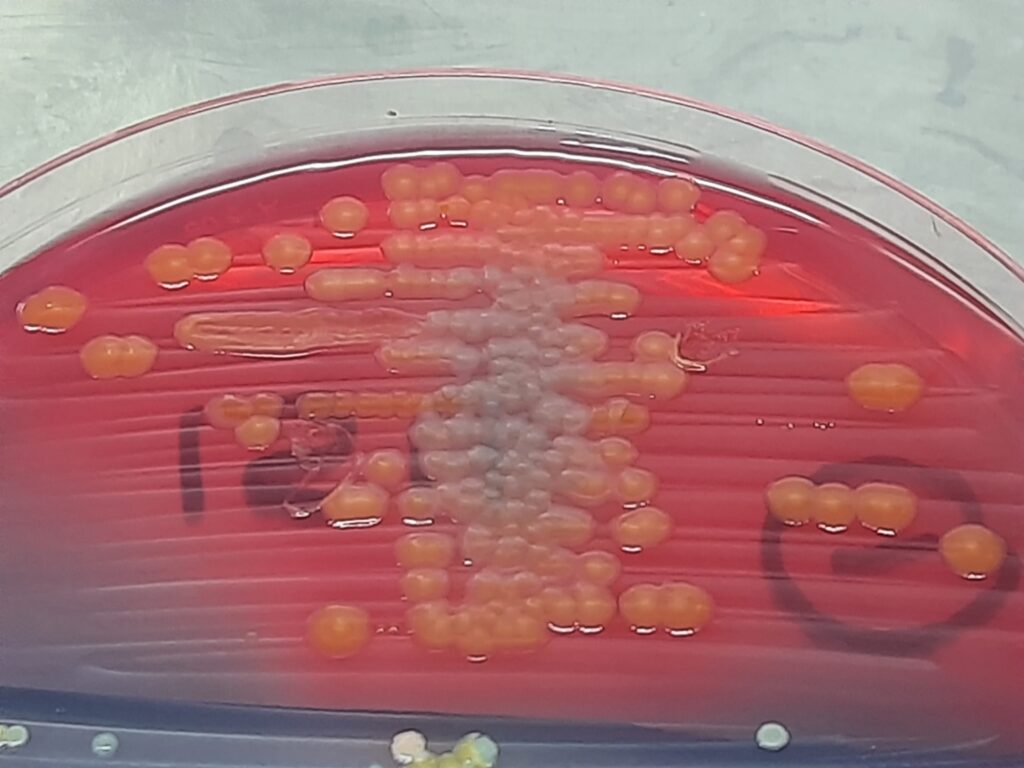
- Primary Isolation: Specimens are inoculated onto suitable media. Commonly used media include Blood agar and MacConkey agar. On MacConkey agar, Citrobacter farmeri will produce lactose-fermenting colonies which will appear pink.
- Colonial Morphology: On blood agar, colonies are typically smooth, moist, and shiny. Hemolytic activity can be checked on this medium as well.
Biochemical Identification
- Triple Sugar Iron (TSI) Agar: Citrobacter species generally produce gas and acid from glucose and lactose or sucrose, resulting in an “A/A” reaction (yellow slant/yellow butt) with or without gas production.
- Citrate Utilization: Positive; the organism uses citrate as its sole carbon source.
- Urease Production: Typically negative for C. farmeri.
- Indole Production: Reactions can vary; testing helps differentiate between Citrobacter species.
- Motility: Citrobacter farmeri is usually motile.
Other tests can include lysine decarboxylase, ornithine decarboxylase, and other enzyme-based assays to further differentiate from other Enterobacteriaceae.

Antimicrobial Susceptibility Testing
This test determines which antibiotics are effective against the isolated strain of Citrobacter farmeri. It’s crucial for guiding appropriate treatment.
Molecular Methods
- Polymerase Chain Reaction (PCR): Can be used to detect specific genes or sequences unique to Citrobacter farmeri.
- Sequencing and Genomic Analysis: In specialized or research settings, genomic analysis can be done to study strain-specific attributes, virulence factors, or antibiotic resistance genes.
Serotyping
Not commonly done for routine identification but can be useful for epidemiological studies or outbreaks.
Treatment
The treatment for infections caused by Citrobacter farmeri typically involves antibiotics. However, the choice of antibiotic should be based on the type and location of the infection, patient factors, and most importantly, antibiotic susceptibility testing results. Some strains of Citrobacter farmeri, like other Enterobacteriaceae, may develop resistance to certain antibiotics, making susceptibility testing crucial.
Empirical Treatment
Before the results of susceptibility testing are available, a broad-spectrum antibiotic or combination might be given, especially if the infection is severe.
Commonly Effective Antibiotics
- Cephalosporins: Third-generation cephalosporins like ceftriaxone or cefotaxime are often effective. Ceftazidime or cefepime (fourth-generation) can also be used.
- Fluoroquinolones: Such as ciprofloxacin or levofloxacin.
- Aminoglycosides: Like gentamicin or amikacin.
- Carbapenems: Imipenem, meropenem, or ertapenem can be effective, especially against multi-drug resistant strains.
- Extended-spectrum penicillins: Piperacillin, often in combination with tazobactam (as piperacillin-tazobactam).
- Trimethoprim-sulfamethoxazole: Can be effective against some strains.
Treatment Considerations
- Meningitis: Due to its ability to penetrate the blood-brain barrier, ceftriaxone or cefotaxime are commonly used for Citrobacter-associated meningitis.
- Urinary Tract Infections (UTIs): For uncomplicated UTIs, shorter courses of antibiotics like ciprofloxacin or trimethoprim-sulfamethoxazole may be effective. More complicated infections might require longer treatments.
Resistance Concerns
Some Citrobacter farmeri strains can produce extended-spectrum beta-lactamases (ESBLs) or become resistant to carbapenems, which can make infections more challenging to treat. In such cases, consultation with an infectious disease specialist is often warranted.
Supportive Care
Depending on the severity and location of the infection, supportive care might be necessary. This can include fluids, electrolyte management, pain management, and other measures.
Prevention and Control
Proper hand hygiene and infection control measures can help prevent the spread of Citrobacter infections, especially in healthcare environments. For patients with indwelling catheters or other medical devices, ensuring that these are regularly checked and changed when necessary can also help prevent infections.
Prevention
Prevention of Citrobacter farmeri infections involves a combination of standard hygiene practices, proper healthcare procedures, and awareness. Here are the primary measures to prevent infections caused by this opportunistic pathogen:
Hand Hygiene
- The most effective way to prevent the spread of many infections, including those caused by Citrobacter species.
- Regular handwashing with soap and water for at least 20 seconds.
- In healthcare settings, or when soap and water aren’t available, use an alcohol-based hand sanitizer with at least 60% alcohol.
Infection Control in Healthcare Settings
- Proper sterilization and disinfection of medical instruments and surfaces.
- Use of personal protective equipment (PPE) like gloves, gowns, and masks when necessary.
- Adherence to guidelines for the prevention of hospital-acquired (nosocomial) infections, especially in intensive care units.
- Isolate patients with multidrug-resistant Citrobacter infections to prevent its spread to other patients.
Proper Catheter Care
- Many Citrobacter infections are associated with the use of indwelling devices like urinary catheters.
- Ensure that catheters are inserted using sterile technique, checked regularly, and removed as soon as they are no longer needed.
Safe Food Practices
- Even though foodborne transmission is less common, it’s always wise to practice safe food handling to prevent any bacterial infections.
- Wash hands before handling food.
- Cook meat to recommended temperatures.
- Wash fruits and vegetables thoroughly.
- Avoid cross-contamination by using separate cutting boards for raw meats and produce.
Safe Water
- Ensure that drinking water is from a safe source.
- In areas where water quality is questionable, boil or use appropriate disinfection methods before consumption.
Awareness and Training
- Healthcare workers should be trained about the risks of Citrobacter and other opportunistic pathogens, and how to prevent their spread.
- Regularly update protocols and guidelines based on current research and recommendations.
Antimicrobial Stewardship
- Responsible use of antibiotics can reduce the development of antibiotic-resistant strains of bacteria, including Citrobacter farmeri.
- Prescribe antibiotics only when necessary and ensure that the full course is completed.
- Regularly review and update hospital antibiotic policies.
Surveillance and Reporting
- In healthcare settings, monitor for outbreaks or increased rates of Citrobacter infections.
- Reporting can help identify patterns and implement control measures more effectively.
Keynotes
Here are some keynotes on Citrobacter farmeri:
- Classification: Citrobacter farmeri is a Gram-negative, rod-shaped bacterium belonging to the Enterobacteriaceae family.
- Habitat: It can be found in various environments, including water, soil, and the intestines of humans and animals.
- Opportunistic Pathogen: While it can exist harmlessly in the gut, C. farmeri can cause infections, especially in immunocompromised individuals.
- Infections: It has been associated with urinary tract infections, respiratory infections, septicemia, meningitis, and more.
- Virulence Factors: C. farmeri may produce capsules, endotoxins, and has the ability to form biofilms, which aid in its pathogenicity.
- Lab Diagnosis: Detection typically involves specimen collection, Gram staining, culturing on selective media, and biochemical tests. Molecular methods like PCR can be used for precise identification.
- Antibiotic Resistance: Some strains have developed resistance to commonly used antibiotics, making susceptibility testing vital for appropriate treatment.
- Treatment: Antibiotic treatment is based on the type of infection and the antibiotic susceptibility profile of the isolated strain. Commonly used antibiotics include cephalosporins, fluoroquinolones, and carbapenems.
- Prevention: Emphasis on hand hygiene, proper infection control in healthcare settings, safe food and water practices, and antimicrobial stewardship.
- Unique Feature: The genus “Citrobacter” is named for its ability to utilize citrate as its sole carbon source, a feature that can be used in laboratory identification.
Further Readings
- Textbooks:
- “Manual of Clinical Microbiology” by the American Society for Microbiology. This manual offers an exhaustive view on clinical microbiology, including a comprehensive section on the Enterobacteriaceae and Citrobacter species.
- “Medical Microbiology” by Murray, Rosenthal, and Pfaller. This textbook provides a foundation in infectious diseases and the organisms behind them, including Citrobacter.
- Research Journals: Look up articles specifically on Citrobacter farmeri in reputable journals such as:
- Journal of Clinical Microbiology
- Clinical Infectious Diseases
- Antimicrobial Agents and Chemotherapy
- Infection Control and Hospital Epidemiology
- Databases:
- PubMed: A free search engine accessing primarily the MEDLINE database of references and abstracts on life sciences and biomedical topics. Simply input “Citrobacter farmeri” to find a multitude of scientific articles on the topic.
- CDC (Centers for Disease Control and Prevention): The CDC website may have information and guidelines related to infections caused by Citrobacter species, especially in the context of nosocomial infections.
- Organizational Guidelines:
- IDSA (Infectious Diseases Society of America): They provide clinical practice guidelines for various pathogens and infections, and you might find references or guidelines related to Enterobacteriaceae or even more specific pathogens.
- Review Articles: These provide comprehensive overviews on specific topics. You might find review articles on the pathogenicity, antibiotic resistance, or clinical manifestations of Citrobacter infections.
- Case Studies: These can be invaluable for understanding the real-world presentation, diagnosis, and management of infections caused by Citrobacter farmeri.

Howdy! I simply would like to give a huge thumbs up for the good information you could have right here on this post. I will probably be coming again to your blog for more soon.