Introduction
Table of Contents
Trichosporon is a genus of yeast-like fungi that belongs to the phylum Basidiomycota. It is commonly found in the environment, especially in soil, water, and various organic matter. Trichosporon species can be opportunistic pathogens, and they are known to cause infections in both humans and animals, particularly in immunocompromised individuals.
The name “Trichosporon” is derived from Greek, where “tricho” means hair, and “sporon” means spore, referring to the characteristic elongated and segmented spores produced by these fungi.
They are characterized by their ability to form creamy-white to pale yellowish colonies on culture media. Microscopically, they are identified by their unique budding pattern, where multiple buds arise from a single mother cell in a “blastoconidial” arrangement. This distinguishes them from other yeast species with more conventional budding patterns.
In medical mycology, some Trichosporon species have been associated with various clinical conditions, including superficial skin infections, onychomycosis (fungal nail infections), and invasive systemic infections, such as fungemia, pneumonia, and disseminated infections in immunocompromised patients.
Identification and differentiation of various Trichosporon species can be challenging, requiring specialized laboratory techniques. Molecular methods, such as DNA sequencing, have become increasingly important for accurate species identification.
While some Trichosporon species are harmless saprophytes (organisms that obtain nutrients from decaying organic matter) in the environment, their role as opportunistic pathogens highlights the importance of understanding and monitoring their presence, particularly in healthcare settings where vulnerable individuals may be at risk of infection. Proper infection control measures and antifungal treatments are crucial in managing Trichosporon infections and reducing associated morbidity and mortality.
Morphology
The morphology of Trichosporon refers to the physical characteristics and structures of this genus of yeast-like fungi. Here are some key aspects of the morphology of Trichosporon:
- Cellular Structure: They are unicellular fungi, meaning they consist of single cells. Each cell is typically spherical or oval in shape and can reproduce asexually through budding.
- Budding: Trichosporon reproduces asexually by budding, a process in which a small daughter cell (bud) forms and eventually separates from the mother cell to become an independent cell. The budding pattern of Trichosporon is unique, as multiple buds can arise from a single mother cell, resulting in a “blastoconidial” arrangement.
- Pseudohyphae Formation: In addition to budding, some Trichosporon species can form pseudohyphae. Pseudohyphae are chains of connected cells that resemble hyphae, the filamentous structures found in true molds. This trait is not present in all Trichosporon species.
- Colonies: On culture media, Trichosporon colonies typically appear as creamy-white to pale yellowish colonies with a smooth or slightly wrinkled texture. The exact appearance may vary depending on the specific species.

- Hyphae Formation: Some Trichosporon species can produce true hyphae under certain conditions. These hyphae are septate, meaning they are divided into compartments by cross-walls called septa.
- Spores: They produce spores, but they are distinct from the spores found in typical molds. The spores of Trichosporon are elongated and segmented, resembling a “hair-like” appearance, which is the origin of the genus name (“tricho” means hair in Greek). These spores are often referred to as arthroconidia or “trichospores.”
- Size: The size of Trichosporon cells and spores may vary among species, but typically, the cells are in the range of a few micrometers in diameter.
Pathogenicity
They can exhibit varying degrees of pathogenicity, depending on the specific species and the host’s immune status. While some Trichosporon species are considered opportunistic pathogens that cause infections mainly in immunocompromised individuals, others may behave as commensals or harmless saprophytes, living on decaying organic matter in the environment without causing disease. Here are some key points regarding the pathogenicity of Trichosporon:
- Opportunistic Infections: They are commonly associated with opportunistic infections, particularly in individuals with compromised immune systems. These infections often occur in patients with underlying conditions, such as hematological malignancies, solid organ transplantation, prolonged use of broad-spectrum antibiotics, or those with human immunodeficiency virus (HIV) infection.
- Fungemia: One of the most significant clinical manifestations of Trichosporon infections is fungemia, which refers to the presence of Trichosporon species in the bloodstream. Fungemia can lead to severe complications and is associated with high mortality rates, especially in immunocompromised patients.
- Disseminated Infections: In severe cases, Trichosporon infections can spread from the bloodstream to various organs and tissues, causing disseminated infections. Organs commonly affected include the liver, spleen, kidneys, lungs, and brain.
- Pulmonary Infections: Trichosporon species can cause pneumonia in susceptible individuals, leading to respiratory symptoms and complications.
- Superficial Infections: Although less common, Trichosporon can cause superficial skin infections, particularly in warm and humid climates.
- Onychomycosis: Trichosporon onychomycosis is a type of fungal infection that affects the nails, causing discoloration and thickening.
- Allergic Manifestations: In some cases, exposure to Trichosporon species can lead to allergic reactions, such as hypersensitivity pneumonitis, especially in individuals who are exposed to large amounts of fungal spores in their environment.
Lab Diagnosis
The laboratory diagnosis of Trichosporon infections involves a combination of different methods to identify the fungus and determine its species. Since some of them can cause opportunistic infections, accurate and timely diagnosis is crucial for appropriate management. The following are the key steps and techniques involved in the laboratory diagnosis of Trichosporon:
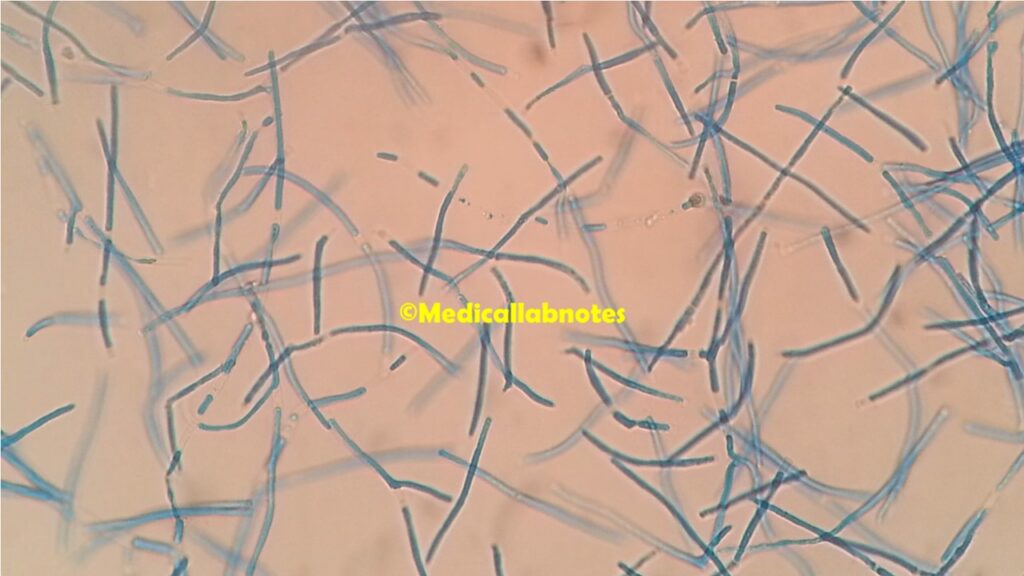
- Microscopic Examination: A direct microscopic examination of clinical samples is often the initial step. They typically appear as yeast-like cells with a characteristic budding pattern, where multiple buds arise from a single mother cell in a “blastoconidial” arrangement. In some cases, pseudohyphae formation may also be observed.
- Culture: Isolation of the fungus in culture is essential for further identification and species determination. Clinical specimens, such as blood, tissue, respiratory secretions, or nail clippings, are inoculated onto appropriate culture media, such as Sabouraud dextrose agar or chromogenic agar. Trichosporon colonies usually appear as creamy-white to pale yellowish colonies with a smooth or slightly wrinkled texture.
- Biochemical Tests: Traditional biochemical tests, such as carbohydrate assimilation tests, can help differentiate Trichosporon from other yeast-like fungi. However, these tests may not always provide reliable species identification.
- Molecular Techniques: Molecular methods, such as DNA sequencing, have become increasingly important for accurate species identification of Trichosporon. Polymerase chain reaction (PCR) assays targeting specific regions of the fungal DNA can be performed to identify the fungus to the species level. DNA sequencing of the PCR products can then be compared with databases to determine the exact species.
- MALDI-TOF Mass Spectrometry: Matrix-assisted laser desorption/ionization time-of-flight mass spectrometry (MALDI-TOF MS) is a rapid and increasingly popular method for identifying fungi, including Trichosporon species. This technique can provide reliable identification by comparing mass spectra of the fungal proteins to an extensive database.
- Antifungal Susceptibility Testing: Antifungal susceptibility testing may be performed to determine the most effective antifungal agents for treatment. Trichosporon species may exhibit varying degrees of resistance to certain antifungal drugs, so susceptibility testing can help guide therapy.
- Histopathological Examination: In cases of invasive infections, histopathological examination of tissue biopsies can reveal the presence of the fungus within tissues. It can also provide valuable information about the nature and extent of the infection.
Treatment
The treatment of Trichosporon infections, also known as trichosporonosis, generally involves antifungal therapy. However, the choice of antifungal agent and treatment approach may vary depending on the severity of the infection, the site of infection, the specific Trichosporon species involved, and the patient’s immune status. Here are some general treatment principles for managing Trichosporon infections:
- Antifungal Therapy: Systemic antifungal agents are the mainstay of treatment for Trichosporon infections. The most commonly used antifungals include:
- Amphotericin B: This broad-spectrum antifungal drug is often the first-line therapy for severe and invasive Trichosporon infections. It can be administered intravenously, and its lipid formulations may be preferred due to reduced nephrotoxicity.
- Azoles: Triazoles, such as voriconazole, itraconazole, and posaconazole, have shown activity against some Trichosporon species and are often considered as alternative or adjunctive therapies, especially for less severe infections. Voriconazole is generally preferred when available.
- Echinocandins: Caspofungin, micafungin, and anidulafungin are antifungals belonging to the echinocandin class. While they are not typically the first-line agents for Trichosporon infections, they may be considered in certain cases, especially if there is resistance to other antifungals.
- Combination Therapy: In severe cases or cases with resistance to single-agent therapy, combination antifungal therapy may be considered. The combination of an azole and an echinocandin, or an azole and amphotericin B, has been used in some refractory infections.
- Antifungal Susceptibility Testing: Performing antifungal susceptibility testing is essential, especially when dealing with invasive or recurrent infections. This helps guide the choice of the most effective antifungal agent.
- Duration of Treatment: The duration of antifungal therapy can vary depending on the site and severity of the infection, as well as the patient’s response to treatment. In many cases, therapy may continue for several weeks or even months.
- Supportive Care: In addition to antifungal therapy, supportive care is crucial in managing patients with these fungal infections, especially those with severe underlying conditions and compromised immune systems.
- Source Control: In cases of localized infections, such as onychomycosis or skin infections, source control measures, such as surgical debridement or removal of infected nails, may be necessary to facilitate treatment efficacy.
Prevention
Preventing these fungal infections involves a combination of general infection control measures and specific strategies targeted at reducing the risk of exposure to the fungus. Here are some key preventive measures:
- Infection Control in Healthcare Settings:
- Adhere to standard precautions: Healthcare personnel should consistently follow standard infection control precautions, including hand hygiene, personal protective equipment (PPE) use, and safe handling of patient care equipment.
- Isolation precautions: Patients with known or suspected these fungal infections should be placed in appropriate isolation precautions, as determined by the specific mode of transmission.
- Environmental Control:
- Maintain a clean environment: Regular cleaning and disinfection of patient care areas, especially in high-risk areas like intensive care units, can help reduce the presence of Trichosporon in the environment.
- Proper ventilation: Ensuring adequate ventilation in healthcare facilities and avoiding stagnant water sources can help prevent the accumulation of fungal spores in the air.
- Antifungal Stewardship:
- Rational use of antifungal agents: Prudent use of antifungal medications can help reduce the risk of selecting for antifungal-resistant strains of Trichosporon. Antifungal stewardship programs promote appropriate use and dosage of antifungal drugs.
- Education and Training:
- Healthcare personnel: Regular training and education of healthcare workers about infection control practices and the prevention of healthcare-associated infections are essential.
- Patients and caregivers: Educate patients and their caregivers about preventive measures, particularly those who are immunocompromised or at higher risk for infections.
- Environmental Monitoring:
- Periodic monitoring of environmental surfaces and air quality in healthcare settings can help identify potential sources of Trichosporon and assess the effectiveness of infection control measures.
- Nail Salons and Beauty Centers:
- Ensuring proper hygiene and sanitation practices in nail salons and beauty centers can help prevent the transmission of Trichosporon nail infections.
- Immunocompromised Patients:
- Close monitoring of immunocompromised patients, such as those with cancer, transplant recipients, or individuals with HIV, is crucial. Early detection and treatment of infections can improve outcomes.
- Research and Surveillance:
- Ongoing research and surveillance of these infections can provide valuable data on the prevalence, risk factors, and antifungal susceptibility patterns of the fungus. This information can guide preventive strategies and treatment approaches.
Keynotes
Trichosporon is a genus of yeast-like fungi belonging to the phylum Basidiomycota.
Keynotes on Trichosporon:
- Morphology:They are unicellular fungi that reproduce through budding. They form unique elongated and segmented spores resembling “hair-like” structures.
- Opportunistic Pathogen: They can cause opportunistic infections, particularly in immunocompromised individuals, leading to conditions like fungemia, pneumonia, and disseminated infections.
- Environment: Trichosporon is commonly found in soil, water, and organic matter, where some species act as saprophytes, breaking down decaying material.
- Clinical Infections: They are associated with superficial skin infections, onychomycosis (nail infections), and systemic infections in vulnerable patients.
- Diagnosis: Laboratory diagnosis involves microscopy, culture, biochemical tests, molecular techniques (DNA sequencing), and MALDI-TOF mass spectrometry for accurate identification.
- Antifungal Treatment: Treatment of Trichosporon infections typically involves systemic antifungal agents such as amphotericin B, azoles (e.g., voriconazole), and echinocandins (e.g., caspofungin).
- Antifungal Resistance: Some of them may exhibit resistance to certain antifungal drugs, necessitating susceptibility testing and, in some cases, combination therapy.
- Prevention: Infection control measures in healthcare settings, environmental hygiene, prudent antifungal use, and education are crucial in preventing Trichosporon infections.
- Immune Status: These infections are more likely to occur in individuals with weakened immune systems, such as those with cancer, organ transplants, or HIV/AIDS.
- Research: Ongoing research and surveillance are important to better understand Trichosporon infections, their epidemiology, and optimal management strategies.
Further Readings
- “Clinical manifestations and molecular identification of Trichosporon spp. isolates causing invasive infections” (Journal of Clinical Microbiology, 2013) – This study discusses the clinical presentation of Trichosporon infections and the use of molecular techniques for species identification.
- “Epidemiology, clinical characteristics, and outcome of candidemia caused by Trichosporon species in critically ill patients” (International Journal of Infectious Diseases, 2018) – This article provides insights into the epidemiology and clinical characteristics of candidemia caused by Trichosporon species in critically ill patients.
- “Antifungal susceptibility testing of Trichosporon species and role of ERG11 and ERG5 genes in azole resistance” (Antimicrobial Agents and Chemotherapy, 2019) – This research explores antifungal susceptibility testing in Trichosporon species and the genetic basis of azole resistance.
- “Trichosporon infections in hematologic malignancy” (Hematology/Oncology Clinics of North America, 2017) – This review focuses on Trichosporon infections in individuals with hematologic malignancies, including incidence, risk factors, and treatment strategies.
- “Trichosporonosis, an emerging fungal infection in solid organ transplant recipients” (Transplant Infectious Disease, 2014) – This article highlights the emergence of Trichosporon infections in solid organ transplant recipients and the importance of early diagnosis and treatment.
- “Environmental distribution of Trichosporon species: A systematic review and meta-analysis” (Fungal Biology, 2018) – This systematic review provides insights into the environmental distribution of Trichosporon species.
- “Trichosporon infection in immunocompromised host: A systematic review and meta-analysis” (Indian Journal of Medical Microbiology, 2021) – This meta-analysis examines Trichosporon infections in immunocompromised hosts, including risk factors and outcomes.
