Found in Giemsa staining of BAL. Possible pathogen?
Table of Contents
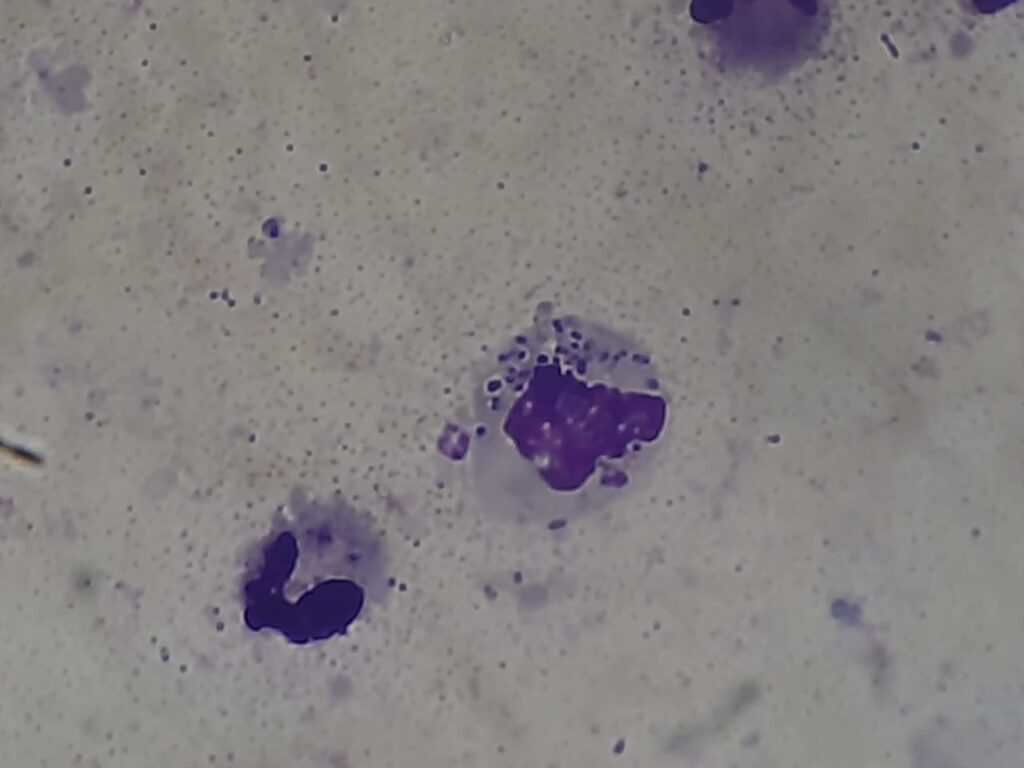
Morphological Features (Center)
- A dense, violet-stained cluster of small, round to oval intracellular structures.
- Surrounded by a faint cellular boundary suggestive of foamy macrophage cytoplasm.
- The inclusion-like structures may appear as dot-like or crescentic bodies.
Possible Pathogen
- The structure is suggestive of Pneumocystis jirovecii (formerly P. carinii), a fungal pathogen seen in immunocompromised patients, especially in:
- HIV/AIDS
- Post-transplant
- Cancer chemotherapy
Supporting Features for Pneumocystis
- Giemsa stain may highlight:
- Foamy exudate (“cotton candy” appearance) in alveolar spaces
- Trophozoites or cyst-like forms (difficult to confirm without a silver stain or immunofluorescence)
Recommendations
- Confirm with Gomori methenamine silver (GMS) or an immunofluorescent stain specific for Pneumocystis.
- Consider PCR for Pneumocystis jirovecii for high sensitivity, especially in cancer patients with atypical pneumonia.
Is it possible to be LD bodies?
Based on the Giemsa-stained BAL image:
The central violet-stained cluster of intracellular forms could resemble Leishman-Donovan (LD) bodies, especially in their:
- Small, round to oval intracellular appearance,
- Presence within macrophage-like host cells.
LD Bodies vs. Pneumocystis jirovecii – Key Differentiating Points
| Feature | LD Bodies (Leishmania donovani) | Pneumocystis jirovecii |
|---|---|---|
| Seen in | Kala-azar / Visceral leishmaniasis | Immunocompromised patients (HIV, cancer, etc.) |
| Host cell | Inside macrophages | Alveolar foamy exudate or inside macrophages |
| Size & shape | 2–4 µm, oval with nucleus + kinetoplast | Round to oval, sometimes crushed cysts or foamy |
| Stain (Giemsa) | Clear nucleus and rod-shaped kinetoplast | Diffuse cytoplasmic stain without kinetoplast |
| Preferred sample | Bone marrow, splenic aspirate, blood smears | BAL fluid (best for Pneumocystis) |
| Geographic relevance | Endemic in Terai/Nepal (esp. Leishmaniasis) | Widespread, especially in HIV/TB coinfection |
Conclusion
- LD bodies are possible, but less likely in BAL samples unless:
- There is a systemic dissemination of leishmaniasis involving the lungs (very rare).
- Pneumocystis jirovecii remains more probable given:
- The specimen (BAL),
- The patient context (cancer),
- The cluster pattern and cytoplasmic clearing.
Recommendation
To differentiate confidently:
- Perform Giemsa at higher magnification (1000X) to check for:
- Kinetoplast + nucleus = LD body
- Consider PCR or special stains:
- For Pneumocystis: GMS stain or PCR
- For Leishmania: PCR or splenic/bone marrow aspirate
Note: The above image of mag.1000X with 4X optical zoom
Image: Giemsa stain, BAL specimen
Magnification: 1000X with 4X optical zoom
This level of detail supports close examination of intracellular structures.
Key Observations
- Intracellular clusters within a macrophage-like cell
- Oval to round basophilic (purple) bodies
- Some appear to have two internal structures, suggesting:
- A nucleus and possibly a kinetoplast (characteristic of Leishmania donovani amastigotes)
Interpretation
Leishman-Donovan (LD) bodies are strongly possible, based on:
- Giemsa staining characteristics
- Presence of:
- Central nucleus
- Rod-shaped kinetoplast
- Intracellular clustering in a host cell (likely macrophage)
- High-resolution morphology (1000X + zoom) supports this ID
But Consider
Although rare, pulmonary leishmaniasis has been reported—especially in immunocompromised patients (e.g., cancer, HIV). In such patients, LD bodies can appear in BAL.
Suggested Confirmatory Steps
- Repeat smear and examine multiple fields under oil immersion.
- Perform PCR or rK39 serology for Leishmania if clinically suspected.
- Rule out Pneumocystis or Histoplasma, which may also mimic.
Conclusion
The morphology seen in this high-magnification Giemsa-stained BAL is consistent with Leishman-Donovan bodies. While rare in the lung, it is possible in immunocompromised or disseminated cases. Further confirmation with molecular or serologic tests is advisable.
A comparison chart or flowchart to distinguish LD bodies from other intracellular pathogens (like Histoplasma or Pneumocystis)
Comparison Chart: LD Bodies vs Histoplasma vs Pneumocystis
| Feature | Leishman-Donovan (LD) Bodies | Histoplasma capsulatum | Pneumocystis jirovecii |
|---|---|---|---|
| Size | 2–4 μm | 2–5 μm | 4–7 μm (cyst); 1–3 μm (troph) |
| Location | Intracellular (macrophages) | Intracellular & extracellular | Alveolar exudates, sometimes within macrophages |
| Shape | Oval with nucleus + rod-shaped kinetoplast | Small oval or round yeast-like cells | Cysts are cup-shaped or crushed-disc; trophs are irregular |
| Staining (Giemsa) | Blue nucleus + pink kinetoplast | Blue cytoplasm, small central basophilic dot | Foamy appearance; pale or faint stain |
| Preferred Host Cell | Macrophage cytoplasm | Macrophage cytoplasm | Exudates or alveolar lining |
| Associated Disease | Visceral leishmaniasis (Kala-azar) | Histoplasmosis | Pneumocystis pneumonia (PCP) |
| Geographic Link | Terai (Nepal), India, Africa | Endemic in river valleys (US, Asia) | Worldwide (esp. HIV/AIDS, transplant) |
| Special Stains | Giemsa, rK39 serology, PCR | PAS, GMS, culture | GMS, DFA, PCR |
| Clinical Clues | Fever, hepatosplenomegaly, pancytopenia | Cough, weight loss, mediastinal lymphadenopathy | Dry cough, hypoxia, bilateral infiltrates |
Diagnostic Flowchart: Intracellular Bodies in BAL (Giemsa)
BAL smear → Giemsa stain (1000X + Zoom)
│
▼
Small intracellular round/oval structures observed
│
┌────────────────┼─────────────────┐
▼ ▼ ▼
LD bodies? Histoplasma? Pneumocystis?
│ │ │
Nucleus + Tiny yeast Foamy exudate
rod kinetoplast like dots Crushed disc/cyst forms
in macrophages in macrophages no clear nucleus
│ │ │
▼ ▼ ▼
rK39 / PCR PAS / GMS stain GMS / DFA / PCR
Spleen/BM Culture, antigen BAL PCR, silver stain
aspirate detection (confirmatory)
Summary Points
- LD Bodies = Nucleus + kinetoplast; macrophage-bound.
- Histoplasma = Tiny budding yeasts; PAS/GMS positive.
- Pneumocystis = No budding; foamy matrix; best with GMS or DFA.
Further Readings
- https://pmc.ncbi.nlm.nih.gov/articles/PMC11898755/
- https://onlinelibrary.wiley.com/doi/10.1002/dc.24280
- https://www.researchgate.net/publication/11200058_Comparison_of_methods_for_identification_of_Pneumocystiscarinii_in_bronchoalveolar_lavage_fluid
- https://pmc.ncbi.nlm.nih.gov/articles/PMC5490308/
- https://pubmed.ncbi.nlm.nih.gov/31322837/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC4920866/
- https://www.semanticscholar.org/paper/Diagnosis-of-Pneumocystis-pneumonia-by-lavage-at-a-Dahiya-Mathur/abf10505a51caefd2687f8c074d49476d37d37c8
- https://journals.lww.com/cddr/fulltext/2022/06010/diagnosis_of_post_kala_azar_dermal_leishmaniasis.17.aspx
- https://www.mdpi.com/2309-608X/9/8/812
- https://www.pathologyoutlines.com/topic/skinnontumorleishmaniasis.html
