Introduction
Table of Contents
Second-line drug susceptibility testing (SL-DST) for tuberculosis is a crucial laboratory procedure designed to detect resistance to anti-TB drugs used when first-line treatment fails (i.e., multidrug-resistant TB – MDR-TB).
- Purpose: To guide the selection of effective, individualized treatment regimens for patients with rifampin-resistant (RR-TB) or MDR-TB, ensuring improved outcomes and reduced transmission.
- Target Drugs: Second-line drugs, primarily Fluoroquinolones (FQ: Levofloxacin, Moxifloxacin), clofazimine (CFZ), and injectable agents (Amikacin, Capreomycin, but now replaced with oral drugs), as well as newer agents like Bedaquiline (BDQ), Linezolid (LZD), Delamanid (DLM), and Pretomanid (Pa),
- When to Perform: Recommended for all patients with Rifampicin-resistant TB/MDR-TB.
- Methods: Includes phenotypic (culture-based) methods (like MGIT 960, LJ proportion method) and genotypic (molecular) methods (like Line Probe Assay (SL-LPA) or Xpert XDR).
Principle
SL-DST measures the susceptibility of Mycobacterium tuberculosis to specific agents by determining the Critical Concentration (CC)—the lowest concentration of a drug that inhibits at least 95% of wild-type strains.
- Phenotypic (Liquid/Solid Culture): The patient’s TB strain is grown in liquid (MGIT) or solid (LJ) media containing specific second-line drug concentrations. If the strain grows, it is considered resistant; if growth is inhibited, it is susceptible.
- Genotypic (Molecular): Detects specific genetic mutations known to cause resistance (e.g., gyrA mutations for fluoroquinolones).
Procedure (Phenotypic – Liquid Culture Method)
The WHO Technical Manual for Drug Susceptibility Testing outlines the following:
- Sample Collection: Sputum samples from patients with suspected MDR-TB.
- Inoculum Preparation: MTB strain is isolated and cultured (usually from a positive primary culture) to a standard concentration.
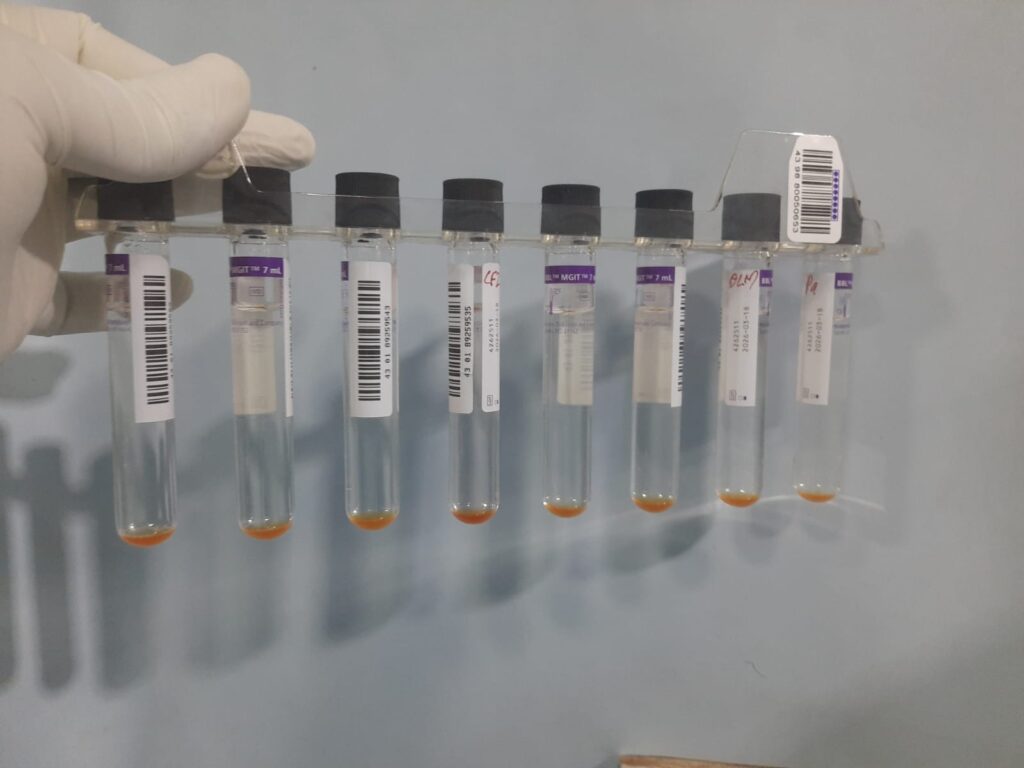
- Inoculation: Inoculum is added to liquid medium (e.g., BACTEC MGIT) containing the drug (e.g., Levofloxacin or Amikacin) and to a control tube (drug-free).
- Incubation: The tubes are incubated in an automated system, usually for up to 6–8 weeks.
- Monitoring: The system continuously monitors for growth (via fluorescence).
Result Interpretation
Results are generally reported as Susceptible or Resistant.
- Susceptible: The growth in the drug-containing tube is less than 100 growth units (GU) or within defined limits, indicating the drug inhibits the bacteria.
- Resistant: The growth in the drug-containing tube reaches 100 GU before or at the same time as the growth control tube, indicating the bacteria can grow despite the drug.
- Limitations: Phenotypic DST can be slow; however, rapid molecular tests like Xpert XDR provide quick results within hours.
Keynotes
- Highest Priority: Testing for Fluoroquinolones (Levofloxacin/Moxifloxacin) is the highest priority among second-line drugs.
- Treatment Should Not Wait: Initiating treatment should not be delayed while waiting for DST results, but results should be used to adjust the regimen.
- Technical Difficulty: SL-DST is more complex and less reproducible than first-line DST, requiring high-quality laboratory infrastructure.
- Cross-Resistance: Resistance to one drug in a class (e.g., Kanamycin) often indicates resistance to others in the same class (e.g., Amikacin).
- Quality Control: Stringent quality control is necessary due to the narrow margin between therapeutic and toxic concentrations of many second-line drugs.
Further Readings
- https://www.ncbi.nlm.nih.gov/books/NBK539506/table/annex6.tab9/
- https://tbksp.who.int/en/node/3148
- https://pmc.ncbi.nlm.nih.gov/articles/PMC5576040/
- https://www.stoptb.org/sites/default/files/imported/document/BoardDocs/15/2.08-11_Rolling_out_diagnostics_in_the_field/2.08-11.3_DST_policy__0.pdf
- https://tbksp.who.int/en/node/3155
- https://www.intechopen.com/chapters/43723
- https://publications.ersnet.org/content/erj/25/3/564
- https://www.ncbi.nlm.nih.gov/books/NBK539506/table/annex6.tab9/
- https://www.who.int/publications/i/item/WHO-HTM-TB-2008.392
- https://globaltb.njms.rutgers.edu/wmatbcourse/module02/02-10c.html
- https://pmc.ncbi.nlm.nih.gov/articles/PMC9301132/
- https://ntep.in/index.php/node/4426/cdstlt-second-line-drug-testing
- https://journals.asm.org/doi/10.1128/spectrum.02506-24
- https://tbksp.who.int/en/node/3108
